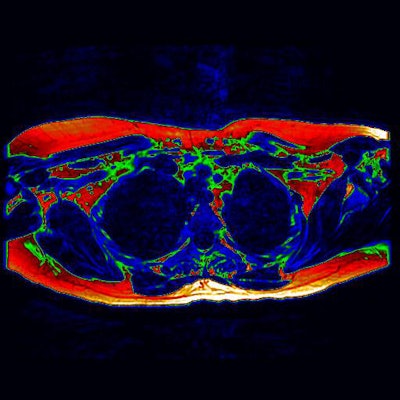
As a critical step toward new therapies to aid the fight against diabetes and obesity, British researchers for the first time are using MRI to show the presence of brown adipose tissue in a living adult.
A new study from Warwick Medical School and University Hospitals Coventry and Warwickshire National Health Service (NHS) Trust, published in the Journal of Clinical Endocrinology and Metabolism (January 2014, Vol. 99:1, pp. E117–E121), outlines the benefits of MRI instead of PET to better detect and visualize so-called brown fat.
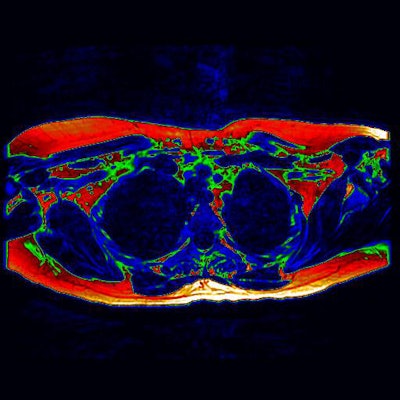 The digitally enhanced axial MRI of the upper chest (as if viewed from the feet) shows area of potential brown fat (green). Image courtesy of the University of Warwick.
The digitally enhanced axial MRI of the upper chest (as if viewed from the feet) shows area of potential brown fat (green). Image courtesy of the University of Warwick.Brown fat has drawn the interests of researchers due its ability to use energy and burn calories, thus controlling weight.
There is the potential to develop safe and effective ways of activating brown fat to promote weight loss and increase energy expenditure, but more data are needed, according to study co-author Dr. Thomas Barber from the department of metabolic and vascular health at Warwick Medical School.
Unlike PET data, which only displays activity, MRI shows brown fat content whether active or not to provide detailed insight into where it can be found in the adult body. This information could prove vital in the creation of future therapies that seek to activate deposits of brown fat.









![Overview of the study design. (A) The fully automated deep learning framework was developed to estimate body composition (BC) (defined as subcutaneous adipose tissue [SAT] in liters; visceral adipose tissue [VAT] in liters; skeletal muscle [SM] in liters; SM fat fraction [SMFF] as a percentage; and intramuscular adipose tissue [IMAT] in deciliters) from MRI. The fully automated framework comprised one model (model 1) to quantify different BC measures (SAT, VAT, SM, SMFF, and IMAT) as three-dimensional (3D) measures from whole-body MRI scans. The second model (model 2) was trained to identify standardized anatomic landmarks along the craniocaudal body axis (z coordinate field), which allowed for subdividing the whole-body measures into different subregions typically examined on clinical routine MRI scans (chest, abdomen, and pelvis). (B) BC was quantified from whole-body MRI in over 66,000 individuals from two large population-based cohort studies, the UK Biobank (UKB) (36,317 individuals) and the German National Cohort (NAKO) (30,291 individuals). Bar graphs show age distribution by sex and cohort. BMI = body mass index. (C) After the performance assessment of the fully automated framework, the change in BC measures, distributions, and profiles across age decades were investigated. Age-, sex-, and height-adjusted body composition reference curves were calculated and made publicly available in a web-based z-score calculator (https://circ-ml.github.io).](https://img.auntminnieeurope.com/mindful/smg/workspaces/default/uploads/2026/05/body-comp.XgAjTfPj1W.jpg?auto=format%2Ccompress&fit=crop&h=112&q=70&w=112)








