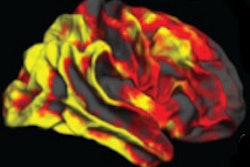
MRI scans have revealed that older adults with bouts of apathy may have smaller volumes of gray and white matter in areas of the brain associated with learning, memory, and internal communication, according to a study published online on 16 April in Neurology.
Researchers from the Netherlands, the U.S., and Iceland found that people with two or more symptoms of apathy had 1.4% less gray-matter volume and 1.6% less white-matter volume than individuals with fewer than two symptoms. The results did not change when patients with depression were excluded from the analysis.
"The key point [of the study] is that this apathy could be prevalent in this population and that it is different from depression," senior author Lenore Launer, PhD, chief of the neuroepidemiology section at the U.S. National Institute on Aging (NIA), told AuntMinnieEurope.com. "If people notice that relatives have a complete loss of interest and motivation and are unwilling to do new things, and they're concerned about it, they should have a clinician examine them."
 Lenore Launer, PhD, from the National Institute on Aging.
Lenore Launer, PhD, from the National Institute on Aging.
Getting older adults to seek therapy, however, may be difficult. More than half of participants (58%) said they prefer to stay at home, suggesting they may be less likely to seek help. This could contribute to an "underdetection" of apathy in the clinical setting, the authors wrote (Neurology, 16 April 2014).
Linking apathy and brain volume
Launer's research at the NIA is focused on understanding risk factors for comorbidities and processes that lead to late-life dementia. She and her colleagues developed several large community-based studies, including the Age, Gene/Environment Susceptibility (AGES)-Reykjavik Study discussed in the Neurology paper.
AGES-Reykjavik is based on a cohort of 5,764 men and women born between 1907 and 1935 in Reykjavik, Iceland. The Icelandic Heart Association (IHA) has followed these subjects since 1967 and began working with the NIA in 2001 to analyze the cohort.
One area of interest is in how the brain ages: Lead author Dr. Anne Grool, PhD, has been exploring a possible link between apathy and brain volume as measured by MRI, especially because apathy among older people has become increasingly recognized as a widespread problem.
"At this point, MRI is the best tool to estimate the size of the brain volumes," Launer said. "It also gives a very good estimate of where there are systemic lesions or small, subclinical infarcts in the brain."
"With the new PET imaging of amyloid and possibly tau [proteins, both of which have been associated with dementia], I think people will be looking into these brain regions," she continued. "It also would be interesting to look at the relationship between those markers of neurodegeneration and apathy symptoms."
Apathy measures
Grool and colleagues used 1.5-tesla MRI (Signa TwinSpeed, GE Healthcare) to assess 4,354 AGES-Reykjavik participants (average age, 76 ± 5 years; 59% female) with no signs of dementia.
The researchers also used the 15-item Geriatric Depression Scale (GDS-15) to measure depression, including three questions from the scale to gauge apathy. The three apathy items asked whether individuals had dropped activities and interests, preferred to stay at home instead of going out and trying new things, and were full of energy.
According to the results, 2,138 subjects had two or more apathy symptoms, and apathy and depression scores were significantly correlated. The researchers then examined the apathy symptoms with the MRI results and found a "significant trend toward smaller total brain volume, total gray-matter volume, and total white-matter volume," as the number of apathy symptoms increased.
For example, study subjects with no apathy symptoms had an average total gray-matter volume of 685 mL, while those with two or more symptoms had volume that was on average 9.5 mL less. Normal subjects had total white-matter volume of 391 mL, while those with two or more apathy symptoms had volume that was on average 6.1 mL less.
MRI also revealed a greater load of white-matter lesions in the frontal lobe: Patients with two or more apathy symptoms had an odds ratio of 1.08 for higher lesion load. This trend increased as the number of apathy symptoms increased. Differences in white-matter lesions in other areas of the brain were not statistically significant.
Normal aging?
Launer said that brain changes, to some degree, are part of the normal aging process. However, it's not expected that everyone will have these kinds of brain changes with accompanying changes in behavior.
"The changes are generally thought to reflect neurodegeneration, or dying neurons, in the gray matter, and vascular disease, which leads to white- and gray-matter damage," she said. "These pathologies do increase with age, but the hypothesis is that they represent disease processes that can be prevented or reduced."
What remains unknown is whether there are any "specific risk factors that lead to the specific changes that result in apathy, versus other types of changes in the brain that we are familiar with," she said.
To follow up this research, Launer and colleagues are conducting smaller studies to explore any associations between genetic and environmental factors and how they may affect brain size, as well as specific risk factors associated with apathy.
"I think what is important for the research that goes forward is that it could be part of the 'syndrome' of Alzheimer's disease," she said. "It is a comorbidity, but I don't think it's clear whether this is a comorbidity that would precede dementia; that will be very difficult to prove. Right now we are a long way off from determining exactly when these processes start in the brain."
![Overview of the study design. (A) The fully automated deep learning framework was developed to estimate body composition (BC) (defined as subcutaneous adipose tissue [SAT] in liters; visceral adipose tissue [VAT] in liters; skeletal muscle [SM] in liters; SM fat fraction [SMFF] as a percentage; and intramuscular adipose tissue [IMAT] in deciliters) from MRI. The fully automated framework comprised one model (model 1) to quantify different BC measures (SAT, VAT, SM, SMFF, and IMAT) as three-dimensional (3D) measures from whole-body MRI scans. The second model (model 2) was trained to identify standardized anatomic landmarks along the craniocaudal body axis (z coordinate field), which allowed for subdividing the whole-body measures into different subregions typically examined on clinical routine MRI scans (chest, abdomen, and pelvis). (B) BC was quantified from whole-body MRI in over 66,000 individuals from two large population-based cohort studies, the UK Biobank (UKB) (36,317 individuals) and the German National Cohort (NAKO) (30,291 individuals). Bar graphs show age distribution by sex and cohort. BMI = body mass index. (C) After the performance assessment of the fully automated framework, the change in BC measures, distributions, and profiles across age decades were investigated. Age-, sex-, and height-adjusted body composition reference curves were calculated and made publicly available in a web-based z-score calculator (https://circ-ml.github.io).](https://img.auntminnieeurope.com/mindful/smg/workspaces/default/uploads/2026/05/body-comp.XgAjTfPj1W.jpg?auto=format%2Ccompress&fit=crop&h=100&q=70&w=100)





![Overview of the study design. (A) The fully automated deep learning framework was developed to estimate body composition (BC) (defined as subcutaneous adipose tissue [SAT] in liters; visceral adipose tissue [VAT] in liters; skeletal muscle [SM] in liters; SM fat fraction [SMFF] as a percentage; and intramuscular adipose tissue [IMAT] in deciliters) from MRI. The fully automated framework comprised one model (model 1) to quantify different BC measures (SAT, VAT, SM, SMFF, and IMAT) as three-dimensional (3D) measures from whole-body MRI scans. The second model (model 2) was trained to identify standardized anatomic landmarks along the craniocaudal body axis (z coordinate field), which allowed for subdividing the whole-body measures into different subregions typically examined on clinical routine MRI scans (chest, abdomen, and pelvis). (B) BC was quantified from whole-body MRI in over 66,000 individuals from two large population-based cohort studies, the UK Biobank (UKB) (36,317 individuals) and the German National Cohort (NAKO) (30,291 individuals). Bar graphs show age distribution by sex and cohort. BMI = body mass index. (C) After the performance assessment of the fully automated framework, the change in BC measures, distributions, and profiles across age decades were investigated. Age-, sex-, and height-adjusted body composition reference curves were calculated and made publicly available in a web-based z-score calculator (https://circ-ml.github.io).](https://img.auntminnieeurope.com/mindful/smg/workspaces/default/uploads/2026/05/body-comp.XgAjTfPj1W.jpg?auto=format%2Ccompress&fit=crop&h=112&q=70&w=112)










