Breast imaging features analyzed by AI could help predict cardiovascular events in women, suggest findings published on 9 March in the European Heart Journal.
Breast arterial calcifications (BACs) that are automatically quantified by AI are an independent predictor of major adverse cardiovascular events (MACE) and mortality, wrote a team led by Dr. Theodorus Dapamede, PhD, from Emory University in Atlanta, GA. The researchers highlighted that this approach adds prognostic value to the Predicting Risk of cardiovascular disease EVENTs (PREVENT) score.
“This approach may provide an opportunistic cardiovascular risk assessment during routine mammography screening without additional radiation exposure to guide earlier and more effective preventive care for women,” Dapamede and colleagues wrote.
Prior research has established connections between BAC found on mammograms and cardiovascular disease risk. While the PREVENT calculator measures risk for cardiovascular disease, it relies on clinical and laboratory data and doesn't involve an anatomic assessment of cardiac vasculature.
The group developed its transformer-based segmentation model to maintain high sensitivity while reducing false-positive detections related to artifacts or nonvascular calcifications. The model makes way for a standardized, automated quantification of BAC as an absolute physical metric (in mm2), it highlighted.
Dapamede and colleagues studied whether AI-based automatic quantification of BAC from screening mammograms predicts cardiovascular disease and mortality beyond PREVENT scores.
The retrospective cohort study included 123,762 women from two healthcare systems -- Emory Healthcare and Mayo Clinic Enterprise -- who had screening mammograms. The team used a transformer-based neural network for segmentation to calculate BAC severity by the following: zero (0 mm2), mild (>0–10 mm2), moderate (>10 mm2 to 25 mm2), and severe (>25 mm2).
Dapamede and colleagues found BACs in 16.1% of the Emory cohort and 20.6% of the Mayo Clinic cohort. Compared with zero BAC, mild, moderate, and severe BAC all proved to be prognostic for any MACE.
Comparison of BAC categories by hazard ratio | ||
BAC category | Emory cohort | Mayo Clinic cohort |
Zero | 1 (reference) | 1 (reference) |
Mild | 1.32 | 1.28 |
Moderate | 1.75 | 1.79 |
Severe | 3.29 | 2.8 |
The researchers also found a pronounced dose-response relationship in both cohorts, where increasing BAC severity corresponded to increases in event rates.
In the Emory cohort, the incidence of MACE increased more than eightfold, from 5.96 per 1,000 person-years in women with zero BAC to 48.89 per 1,000 person-years in those with severe BAC. The team found that event rates were consistently higher in the Mayo Clinic cohort compared with the Emory cohort across all levels of BAC severity.
Finally, each 1 mm2 increase in BAC conferred an additional 2% to 3% risk for MACE (p < 0.001).
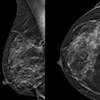
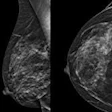
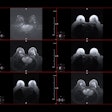
 Examples of mammograms with mild, moderate, and severe breast arterial calcification quantified by an AI model developed by researchers from Emory University and Mayo Clinic Enterprise. (Left) Original image. (Right) AI model heat map with breast arterial calcification score shown above.Images republished under a Creative Commons license (CC-BY-NC).
Examples of mammograms with mild, moderate, and severe breast arterial calcification quantified by an AI model developed by researchers from Emory University and Mayo Clinic Enterprise. (Left) Original image. (Right) AI model heat map with breast arterial calcification score shown above.Images republished under a Creative Commons license (CC-BY-NC).
This approach could prove to be an opportunistic and effective cardiovascular risk assessment method in women, without added radiation exposure, the study authors highlighted.
“Its predictive value is independent of traditional risk factors and PREVENT scores suggesting that BAC screening could enhance early cardiovascular risk detection in women undergoing routine mammography,” they wrote.
The results of the implementation of BAC as an independent predictor of cardiovascular disease risk and mortality in women, wrote Dr. Lori Daniels, from the University of California, San Diego, in an accompanying editorial.
"Regardless of the reporting metric ultimately adopted, it is time to shift BAC from observation to implementation, leveraging a touchpoint women already trust, to advance prevention for what remains the leading cause of death among women," Daniels wrote.
Read the full study here.