It's essential to identify patients at risk of developing coronary artery disease (CAD) -- but also to limit unnecessary repeat imaging, according to a recent analysis of data from the Scottish Computed Tomography of the HEART (SCOT-HEART) trial.
“Determining which patients will develop CAD [enables] the targeting of preventative medical therapies ... [and] understanding the timeline of the development of CAD [helps] determine the optimal time interval for follow-up imaging,” wrote a team led by Lia Avigdor of the University of Edinburgh. The group's results were published on 5 March in European Radiology. Additionally, co-author Prof. Michelle Williams, PhD, spoke on the findings in a presentation at ECR.
Current risk-scoring approaches for CAD may underestimate risk in subgroups such as women and younger people, resulting in patients undergoing imaging to identify the presence of CAD and monitor its progression. But clinicians must consider the downstream risks of radiation exposure and unnecessary testing associated with serial cardiac imaging.
The SCOT-HEART trial followed 4,146 participants (age range, 18 to 75) for 10 years. In this analysis, Avigdor and colleagues randomly sorted patients into two groups of 2,073 participants each. One group had received standard care, and the other standard care plus recommended coronary CT angiography (CCTA). Of the second group, 1,778 underwent CCTA.
Overall, the researchers found that approximately one-third of patients who underwent CCTA and had normal results developed CAD over the 10-year study period that was identified on repeat imaging.
They also reported the following:
- Of the patients with baseline-normal CCTA, 193 subsequently underwent CT imaging within 10 years of the initial CCTA. Of these, 31 (6%) underwent repeat cardiac CT and 162 (31%) underwent subsequent chest CT.
- Of the 31 patients who had subsequent cardiac CT imaging, 17 (55%) underwent CCTA; 13 (42%) had CCTA and noncontrast CT for coronary artery calcium scoring; and one (3%) had noncontrast CT solely for coronary artery calcium scoring.
- CAD was identified on the subsequent imaging of 15 (48%) of these 31 patients.
- On subsequent CCTA imaging, 16 (53%) did not have evidence of CAD. CAD was identified in the other 15 patients, and classified as nonobstructive and mild or moderate in 14 of these.
- For the 162 who underwent subsequent chest CT, coronary artery calcification was identified in 41 (25%).
- The 162 patients with CAD identified on subsequent CT were older, more likely to smoke, and had a higher 10-year cardiovascular risk score compared to those who did not have subsequent chest CT imaging. The 31 patients with CAD on subsequent cardiac CT were more likely to smoke, but had no other differences from those without subsequent imaging.
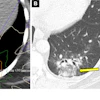
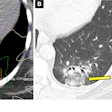
 Development of CAD in a 43-year-old male smoker, with atypical chest pain, hypercholesterolemia, and a family history of CAD. At baseline, the coronary artery calcium score was zero (A), and the coronary CT angiogram was normal (B). Noncontrast CT chest (C) 10 years later showed calcified plaques in the right coronary artery and left circumflex coronary artery.EJR
Development of CAD in a 43-year-old male smoker, with atypical chest pain, hypercholesterolemia, and a family history of CAD. At baseline, the coronary artery calcium score was zero (A), and the coronary CT angiogram was normal (B). Noncontrast CT chest (C) 10 years later showed calcified plaques in the right coronary artery and left circumflex coronary artery.EJR
While CAD on subsequent CT was not an independent predictor of the combined outcome of CAD death or nonfatal myocardial infarction or of all-cause mortality, these patients were more likely to undergo invasive coronary angiography and revascularization.
The findings suggest that more evaluation of the development and progression of CAD with serial CCTA is needed, along with further refining of risk-prediction metrics.
“Understanding the natural history of CAD development and progression would be invaluable for recommendations regarding optimal time intervals for follow-up imaging and initiation of preventative therapies,” the authors concluded.
Read the study findings here; a commentary on this study is also available.