“Are you always working in the dark?” It is the kind of question colleagues from other departments ask, half-jokingly, when they step into a radiology reading room. The lights are low, the monitors glow, and the outside world can feel a bit removed. But the question behind it is a real one: what that kind of environment does to the people who spend most of their day in it.
A review published in Insights into Imaging takes a closer look.
Anna Landsmann, EDiR, of Kantonsspital Baden, affiliated with the University of Zurich, in Baden, Switzerland, and colleagues examined how working for long periods in low-light conditions may affect radiologists’ internal rhythms, mood, and cognitive performance.
A workplace that signals night during the day
In practice, radiology reading rooms are usually kept at around 20 to 40 lux, and sometimes even lower depending on the subspecialty. Radiologists may spend eight to 10 hours a day in these conditions, often with little exposure to daylight.
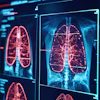
 Low-light clinical environments can create a constant twilight effect, raising questions about how such conditions shape attention, fatigue, and daily rhythms.Tima Miroshnichenko/Pexels
Low-light clinical environments can create a constant twilight effect, raising questions about how such conditions shape attention, fatigue, and daily rhythms.Tima Miroshnichenko/Pexels
For comparison, typical office lighting is around 300 to 500 lux, while daylight outdoors can reach 10,000 lux or more, meaning radiologists may spend most of the day at less than one percent of natural daylight intensity. In practical terms, that places a typical radiology workday closer to indoor twilight than daylight.
Light does more than make things visible. It acts as a signal that helps keep the body aligned with the day. When that signal is reduced over long stretches, sleep patterns, alertness, and emotional balance can start to drift. The review links limited light exposure to fatigue, sleep disruption, and depressive symptoms, while noting that it is difficult to separate these effects from other factors in daily practice.
Findings from chronobiology research point in a similar direction. Limited daylight during daytime hours can shift internal timing in ways that resemble mild forms of shift work. Even during a normal workday, the body may not fully register it as daytime.
The authors also refer to studies showing that 76.7% of radiologists report at least one dimension of burnout, such as emotional exhaustion or depersonalization. In the review, this figure is drawn from prior survey-based studies, reflecting broader working conditions rather than lighting alone. The work environment is only one part of that picture, but it is part of it.
Designed for images, not for people
Low-light conditions in radiology are intentional. They help improve image contrast and reduce glare, which supports accurate interpretation. Over time, this requirement has shaped not just how images are read, but how entire workspaces are built.
What is less often reconsidered is whether those environments still make sense in the same way today. Radiology has moved from film to fully digital workflows, but the physical setup of reading rooms has changed more slowly. Modern diagnostic monitors now offer higher brightness and contrast than earlier systems, raising questions about how much complete darkness is still technically necessary.
The contrast more noticeable when placed alongside general workplace expectations in Europe.
At the EU level, guidance states that workplaces should have access to natural light wherever possible, although it does not specify how this applies to radiology settings.
In Austria, the Arbeitsstättenverordnung, or Workplace Ordinance, requires natural light, a visual connection to the outside, and appropriate artificial lighting in permanent workspaces. In practice, however, radiology reading rooms are often designed without direct daylight exposure, reflecting the priority given to diagnostic conditions.
Similar approaches can be seen in other European countries. Daylight access is generally considered important, but radiology is frequently treated as an exception.
A broader shift in design
At the same time, there has been a broader shift in how healthcare environments are designed. In many areas, more attention is now paid to how light, space, and atmosphere affect both patients and staff. Studies in healthcare design have linked access to daylight with reduced stress, improved mood, and better overall well-being for both patients and healthcare workers.
In other high-reliability professions, including aviation and intensive care, fatigue and circadian disruption have been associated with measurable declines in attention, slower reaction times, and increased error rates.
Radiology stands slightly apart from that trend. While patient-facing areas are often redesigned with well-being in mind, reading rooms tend to follow long-established technical standards.
The question also looks different depending on geography. In northern Europe, where daylight is limited during winter months, awareness of how light affects mood and energy is well established. In some settings, workplaces have started to integrate light-based strategies to support daily rhythms. Radiology departments, however, often still follow traditional low-light setups.
More than a wellbeing issue
The impact may not stop at how radiologists feel. In other fields where attention and precision matter, fatigue and poor sleep have been linked to lapses in concentration and slower decision-making. Landsmann and colleagues suggest this raises a practical question for radiology as well, whether working for long hours in low-light conditions could affect how images are read over time.
"The issue also reflects how the specialty is evolving," they wrote.
Imaging demand is increasing across Europe, including in countries such as Austria, where utilization is already high. Austria is among the countries with high imaging utilization in Europe, with more than 300 CT and MRI examinations per 1,000 population annually.
At the same time, radiology faces ongoing challenges in attracting and retaining staff, and how the work is experienced may play a role. The reading room is often associated with long hours, limited daylight, and a certain degree of isolation. That perception, and the environment itself, may influence how the field is viewed by trainees and early-career doctors.
In that context, lighting becomes part of a broader question about sustainability. It is not only about workload or staffing levels, but also about how daily work is structured.
Landsmann and colleagues point to several practical adjustments, including lighting systems that can be adapted throughout the day, indirect light sources to reduce strain, access to daylight during breaks, and layouts that separate dark reading areas from brighter spaces for collaboration.
The goal is not to change the need for low-light conditions during image interpretation, but to introduce more flexibility around it. The authors note that more data are needed, particularly studies that follow how such changes affect health and performance over time.
For now, the reading room remains dim, and the question from colleagues still lingers: “Are you always working in the dark?” The answer is yes. The more difficult question is how long that model can continue.
The full study is available here.