Researchers have identified measurable and distinct quantitative CT (QCT) histogram patterns in the lungs of welders that differ from those caused by cigarette smoking, according to a study published May 6 in the Canadian Respiratory Journal.
The study also confirms that occupational welding fume exposure progressively erodes lung function -- findings that could improve diagnosis of welder's pneumoconiosis, a condition that is routinely missed, wrote a team led by Merve Demirci Atik, MD, of Dokuz Eylul University in Izmir, Turkey.
"Diagnosing welder's pneumoconiosis via radiology is challenging and often underestimated due to the high smoking rates among welders," Atik and colleagues explained. "A definitive diagnosis is crucial for early termination of exposure, as well as the worker’s compensation and legal rights."
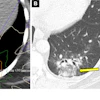
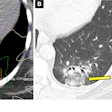
Ill-defined centrilobular nodules are the most common radiological sign of welding fume exposure, the team wrote, noting that they are also frequently seen in smoking-related respiratory bronchiolitis -- making smoking a confounding factor in the diagnosis of welder’s pneumoconiosis. The group investigated any QCT patterns associated with welding fume exposure, while also accounting for the effects of cigarette smoking. It also assessed any relationship between welding fume exposures and pulmonary function test results.
The research included a cohort of 136 men (66 welders and 70 controls), all of whom underwent non-contrast chest CT imaging. The welders' average age was 40, while the control group's average age was 42. More than half the welders (51.5%) and 61.4% of the control participants were current smokers. Mean career length of the welders was 21 years.
The investigators estimated individuals' welding fume exposure index and tracked cigarette pack-years. Two radiologists blinded to welding fume exposure information analyzed CT histogram measurements both manually and using imaging analysis software; the histogram measured the shape of the lung attenuation distribution on CT via skewness and kurtosis curves. The study cohort was divided into four groups: unexposed, welding fumes only, cigarette smoke only, and both.
 An explanatory schematization of the quantitative CT (histogram analysis) method. Atik/Canadian Respiratory Journal
An explanatory schematization of the quantitative CT (histogram analysis) method. Atik/Canadian Respiratory Journal
 Histogram curves of the four distinct exposure groups.Atik/Canadian Respiratory Journal
Histogram curves of the four distinct exposure groups.Atik/Canadian Respiratory Journal
The researchers reported a statistically significant difference between those exposed only to welding fumes and those who smoked only, with the two exposures pulling the histogram in opposite directions. When they conducted an analysis adjusted for smoking-pack years, the proportion of low-density lung voxels in the –949 to –850 Hounsfield Units (HU) range decreased significantly with welding fume exposure (p = 0.037), while voxels above –750 HU -- a range associated with ground-glass opacities -- increased, suggesting parenchymal infiltration rather than the air-trapping pattern more characteristic of smoking.
The study also found significant decreases in a measure called FEF 25–75 (i.e. the flow rate between 25% and 75% of vital lung capacity), which may indicate the presence of small airway disease and which could be an early functional signal of fume-related lung injury, the team noted.
The results confirm that welding fume exposure and cigarette smoking both lead to chronic inflammation and functional loss in the lungs, but more research is needed to distinguish between the two, according to the authors.
"[More research] will help avoid underdiagnosis of pneumoconiosis, which is a barrier to preventing progression and securing legal compensation, especially among welders who smoke," they concluded.
Access the full study here.