Statins were doing their job. LDL cholesterol was down. The guidelines were being followed. But plaque was still progressing.
This is the central clinical gap: even with optimal low-density lipoprotein (LDL) control, many patients continue to experience plaque progression, a phenomenon known as residual cardiovascular risk, driven by inflammatory, genetic, and metabolic pathways that standard cholesterol metrics do not capture.
New results from the HURRICANE study, presented at ECR 2026, begin to put numbers to that gap.
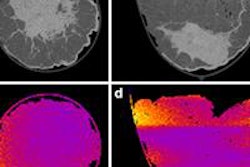
 "With photon-counting CT we can quantify plaque volume and its components objectively and track how they change over time," said Mariaelena Occhipinti, MD, PhD, of Fondazione Gabriele Monasterio Regione Toscana CNR in Pisa, Italy.Courtesy of Claudia Tschabuschnig
"With photon-counting CT we can quantify plaque volume and its components objectively and track how they change over time," said Mariaelena Occhipinti, MD, PhD, of Fondazione Gabriele Monasterio Regione Toscana CNR in Pisa, Italy.Courtesy of Claudia Tschabuschnig
Dr. Mariaelena Occhipinti, MD, PhD, of Fondazione Gabriele Monasterio Regione Toscana CNR in Pisa, Italy, reported findings from 93 patients with coronary artery disease (CAD) who completed 12-month follow-up. Most were on statins, LDL levels improved, yet plaque still progressed.
Moving past the “bloom”
Coronary CT angiography (CCTA) has long struggled with a core limitation: calcified plaque creates blooming artifacts that exaggerate stenosis, while noncalcified plaque remains difficult to quantify.
Dense calcium spreads beyond its true boundaries, leading to systematic overestimation of stenosis.
Photon-counting CT (PCCT) changes that at the detector level. Instead of converting x-rays into light and averaging signal, it counts individual photons and measures their energy. Combined with smaller detector pixels and reduced electronic noise, this architecture keeps calcium confined to its true boundaries, marking the most significant CT hardware shift in decades.
The impact is already measurable. Research published in Radiology showed that PCCT led to lower -- and more accurate -- CAD-RADS classifications in 54% of patients by reducing calcium-driven overestimation.
The HURRICANE study moves beyond this single timepoint advantage. Using paired PCCT scans and semiautomated analysis, Occhipinti’s team quantified how plaque volume and composition evolve over time.
Progression despite treatment
HURRICANE (Health Improvement by Understanding Residual Risk in CAD and New Targets for Treatment) is a prospective EU-funded study. Over 12 months, statin use increased from 65% to 78%, and the proportion of patients reaching LDL levels below 70 mg/dL rose from 37% to 51%.
Imaging told a different story. Total plaque volume increased from 417 to 498 mm³ in under a year (p < 0.0001). Calcified plaque drove much of the change, rising 28% from 214 to 275 mm³.
Patients with LDL levels below 70 mg/dL had more than double the plaque burden at both baseline and follow-up -- likely reflecting more advanced disease and therefore more aggressive treatment. Yet critically, the rate of progression was statistically similar regardless of LDL control.
This is the most clinically relevant finding: lowering LDL did not halt disease progression. In practical terms, this is residual risk made visible: disease activity continuing along pathways that lipid-lowering therapy alone does not address.
Another AuntMinnieEurope article has previously covered how photon-counting CT improves image quality and diagnostic confidence for coronary CTA compared to conventional systems. The HURRICANE data add a longitudinal dimension: plaque composition is shifting -- calcification increasing, total burden growing, even as treatment targets are met.
“Despite optimized medical therapy, CAD may progress rapidly in patients with stable CAD,” Occhipinti noted. At baseline, 59% of patients had extensive or obstructive disease; by one year, seven additional patients had progressed into that category.
Resolution still catching up with analysis
Quantitative analysis in the study was performed on standard-resolution PCCT datasets, as current commercial software cannot yet process ultra-high–resolution (UHR) data at scale.
This is an important limitation, but also a signal of what’s coming. The current results likely represent a floor rather than a ceiling of what PCCT can detect. As software catches up with UHR datasets, plaque characterization is expected to become even more granular, potentially revealing progression that is currently underestimated.
“This gives us space to still improve plaque characterization,” Occhipinti said.
Future analyses will integrate genetics and lipidomics to better explain why some patients progress despite LDL control, pointing toward inflammatory drivers, triglyceride-rich lipoproteins, and other mechanisms beyond standard lipid profiles.
The longer-term goal is more precise risk tracking: using serial imaging not just to confirm treatment success, but to identify when therapy is failing.
This is where PCCT may move beyond diagnostics into real-time disease monitoring and personalized treatment guidance.
Other photon-counting CT findings from ECR 2026
Lung and chest
At radiography-comparable dose, PCCT preserved airway wall metrics but underestimated emphysema, relevant for lung cancer screening.
For pulmonary nodules, PCCT at 78% lower dose outperformed standard CT for both radiologists and AI tools. Low-dose PCCT preserved ILD detection in inflammatory myopathy at a fraction of standard dose.
UHR-PCCT improved detection of ground-glass opacities and reticulations in systemic sclerosis. In sarcoidosis, 0.2 mm reconstructions visualized sub-millimeter micronodules with 30% to 50% dose reduction. For lung perfusion in CTEPH, PCCT correlated strongly with V/Q-SPECT (r = 0.72), suggesting potential as a single-modality alternative.
Vascular and neuro
Dual-layer spectral CT achieved an AUC of 0.99 for differentiating lipid-rich necrotic core in carotid plaques. PCCT with black-blood technique matched vessel wall MRI for noncalcified plaque (ICC = 0.96) and detected more high-risk plaques than conventional CTA.
For cerebral CTA, 90 kVp with sharp kernel improved vessel sharpness over standard protocols. In intracranial aneurysm follow-up, UHR-PCCT showed 100% accuracy for stent wall apposition and >93% for neck coverage. For below-the-knee peripheral artery disease, UHR-PCCT reached 94% per-segment diagnostic accuracy.
Funding
The HURRICANE study is supported by the PNRR-MAD-2022-12376550 project, Next Generation EU, funded by the European Commission.