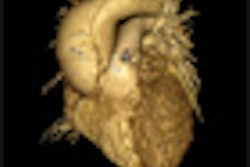
VIENNA - Cardiovascular MRI is becoming increasingly appealing in population-based research, but accurate measurement of the diameters of the aorta and pulmonary trunk remains a key difficulty that needs to be addressed, according to participants at yesterday morning's well-attended vascular refresher course.
A major problem faced with semiautomated or automated measurements is working out the exact location of the outer wall of the vessel, stated session moderator Prof. Jonathan Gillard, professor of neuroradiology at the University of Cambridge School of Clinical Medicine, U.K. Finding the lumen is generally straightforward, but seeing the outer wall is often tricky and can lead to errors.
 Prof. Jonathan Gillard, professor of neuroradiology at the University of Cambridge School of Clinical Medicine, U.K. All images provided by ESR.
Prof. Jonathan Gillard, professor of neuroradiology at the University of Cambridge School of Clinical Medicine, U.K. All images provided by ESR.
"It's especially complicated in the thoracic aorta," concurred Dr. Birger Mensel, from the Institute for Diagnostic Radiology and Neuroradiology, Ernst-Moritz-Arndt-University Greifswald, Germany. "There is often a very small distance between the ascending aorta and the pulmonary trunk. In most cases, there is a small amount of fat, which is of high signal. You can use this to differentiate between the lumen and the wall, but sometimes it is hard to find the correct division line."
For the diameters of the thoracic and abdominal aorta and the pulmonary trunk, no definition exists to distinguish normal diameter variation from a pathologically enlarged aorta, and there is a need for a validated, simple, and reliable measurement technique to analyze large vessels, he explained.
 Dr. Birger Mensel, from the Institute for Diagnostic Radiology and Neuroradiology, Ernst-Moritz-Arndt-University Greifswald, Germany.
Dr. Birger Mensel, from the Institute for Diagnostic Radiology and Neuroradiology, Ernst-Moritz-Arndt-University Greifswald, Germany.
"Such a method should enable measurement from MR images without contrast medium administration, since stricter criteria apply to their use in volunteers participating in epidemiologic research," said Mensel. "The most valid method to measure a vessel diameter is the orthogonal measurement, which means perpendicular to the blood flow. Unfortunately this method requires very time-consuming image postprocessing when performed manually and for a large number of datasets."
A simple and widely used method is to measure the diameters from axial imaging slices, but until now, no validation of this measurement method has existed.
In their study presented at ECR 2012, Mensel and his colleagues sought to validate the diameter measurements from plain, axial MRI sequences. They used imaging data from 50 male volunteers, all of whom were examined according to a standardized MRI protocol. The aorta and pulmonary trunk were first imaged with a plain axial VIBE (volume-interpolated breath-hold examination) sequence. The gold standard, contrast-enhanced MR angiography (CE-MRA), was performed with T1 FLASH sequence in the coronal plane.
The diameters of the vessels were measured at six predefined anatomical sites: the ascending aorta, aortic arch, descending aorta, the supra- and infrarenal aorta, and the pulmonary trunk. All measurements were performed in both sequences by two independent observers.
 Dr. Martin Simon, from the Clinic for Radiology and Nuclear Medicine, University Hospital of Schleswig-Holstein, Campus Luebeck.
Dr. Martin Simon, from the Clinic for Radiology and Nuclear Medicine, University Hospital of Schleswig-Holstein, Campus Luebeck.
"For true orthogonal diameter measurement, double oblique reformations of coronal and sagittal CE-MRA sequences were generated in each of the six segments," said Mensel. "On plain VIBE images, diameters were measured in strictly axial slices without any postprocessing."
Comparison of the diameters measured from CE-MRA and VIBE images revealed a strong correlation with coefficients ranging from 0.74 to 0.95. Mean bias did not exceed 6%, and limits of agreement were below 15%. Intraobserver agreement yielded impressive results, with a mean bias of less than 2% and the limits of agreement of less than 15 %, while interobserver agreement showed a mean bias of less than 2% and the limits of agreement were below 10 %, he concluded.
In the same session, radiologists from Luebeck, Germany, presented results from a study aimed at evaluating the accuracy of a triphasic MDCT protocol for detecting aortic dissections, intramural hematoma, and vascular complications in suspected cases of acute aortic syndrome. Over 32 months, they studied 432 patients, and MDCT confirmed the diagnosis in 56 patients.
Intramural hematoma of the pulmonary trunk were more frequent than expected, said lead presenter Dr. Martin Simon, from the Clinic for Radiology and Nuclear Medicine, University Hospital of Schleswig-Holstein, Campus Luebeck. Nonenhanced scans are indispensable and are a prerequisite for accurate detection of intramural hematoma in patients with suspected acute aortic syndrome.
Originally published in ECR Today March 2, 2012.
Copyright © 2012 European Society of Radiology