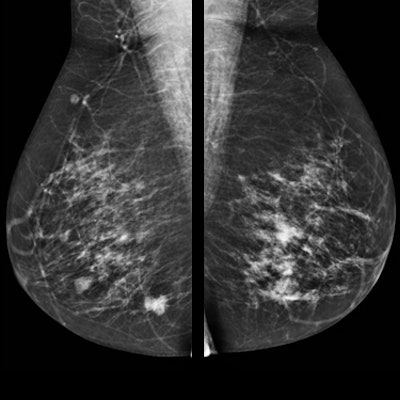
Contrast-enhanced mammography (CEM) may be an alternative to breast MRI for preoperative staging of invasive lobular carcinoma, suggests findings published on 13 May in the European Journal of Radiology.
Researchers led by Dr. Marc Lobbes, PhD, from Maastricht University in the Netherlands found that both imaging methods overestimate tumor size in patients diagnosed with invasive lobular carcinoma, as well as have no significant difference in diagnostic odds ratios between the two. CEM did, however, demonstrate a statistically significant improvement in specificity.
"Based on the results ... preoperative staging of invasive lobular carcinoma using CEM instead of MRI has a comparable diagnostic performance, not only when assessing maximum tumor size but also for the detection of multifocal and/or contralateral breast cancer foci," Lobbes and co-authors wrote.
About 10% of breast cancers are invasive lobular, which is more frequently tied to multifocal and contralateral breast cancer. This type also has histologic characteristics that make it difficult to detect on conventional imaging methods. These include stromal invasion by single files of cells and little disturbance to nearby breast architecture.
Accurate preoperative staging is important in determining the best treatment strategies. Previous research suggests that breast MRI is most accurate in tumor sizing, including for invasive lobular carcinoma. However, the technology is not as accessible as other imaging modalities and can be labor-intensive.
Previous studies also suggest that CEM measures up to breast MRI in terms of tumor sizing and detecting cancers. Lobbes and colleagues wanted to put the two modalities to the test. They investigated the agreement between the two for measuring tumor size, as well as compared their ability to detect multifocal invasive lobular carcinoma and contralateral breast cancer foci.
The study included 305 invasive lobular carcinoma cases from women with an average age of 63.7 years. The researchers noted that preoperative staging was done using MRI in 266 cases and CEM in 77 cases, with some cases overlapping.
They found that MRI overestimated tumor size by 1.5 cm while CEM did the same by 2.1 mm, respectively. The authors wrote that size measurements for invasive lobular carcinoma tend to become less accurate in larger tumors above 3 cm, no matter which imaging method is used.
"In these larger tumors, the risk of involved surgical margins increases," they wrote.
The team also found that while MRI had the advantage for sensitivity, that difference wasn't significantly different. CEM, however, showed higher specificity and the difference was statistically significant. And the modalities also demonstrated comparable sensitivity and specificity for contralateral breast cancer.
| Comparison between CEM, MRI for invasive lobular carcinoma staging | |||
| MRI | CEM | p-value | |
| Sensitivity (multifocal disease) | 85.7% | 77.8% | 0.685 |
| Specificity (multifocal disease) | 79.2% | 91.5% | 0.046 |
| Sensitivity (contralateral breast cancer) | 96% | 87.5% | 0.979 |
| Specificity (contralateral breast cancer) | 92.1% | 98.6% | 0.099 |
The team also found that CEM showed higher diagnostic odds ratios for both multifocal disease and contralateral breast cancer compared to MRI. However, it deemed these differences to be non-significant (p = 0.56 and p = 0.78, respectively).
The study authors also wrote that they are preparing a related study where women undergo both CEM and MRI in a short time window. They added that this should have larger, prospective data for "sufficient statistical power."
Still, they affirmed that their published study showed that CEM is able to match breast MRI's performance for assessing tumor size and diagnosing multifocal or contralateral breast cancer.
Disclosure: Lobbes received several speaker's fees and a research grant from GE Healthcare, Hologic, Bayer, and Guerbet. Co-author Dr. Joachim Wildberger from the university received institutional grants and speaker's fees from Agfa, Bayer, Bard Medical, GE Healthcare, Optimed, Philips Healthcare, and Siemens Healthineers.


















![Overview of the study design. (A) The fully automated deep learning framework was developed to estimate body composition (BC) (defined as subcutaneous adipose tissue [SAT] in liters; visceral adipose tissue [VAT] in liters; skeletal muscle [SM] in liters; SM fat fraction [SMFF] as a percentage; and intramuscular adipose tissue [IMAT] in deciliters) from MRI. The fully automated framework comprised one model (model 1) to quantify different BC measures (SAT, VAT, SM, SMFF, and IMAT) as three-dimensional (3D) measures from whole-body MRI scans. The second model (model 2) was trained to identify standardized anatomic landmarks along the craniocaudal body axis (z coordinate field), which allowed for subdividing the whole-body measures into different subregions typically examined on clinical routine MRI scans (chest, abdomen, and pelvis). (B) BC was quantified from whole-body MRI in over 66,000 individuals from two large population-based cohort studies, the UK Biobank (UKB) (36,317 individuals) and the German National Cohort (NAKO) (30,291 individuals). Bar graphs show age distribution by sex and cohort. BMI = body mass index. (C) After the performance assessment of the fully automated framework, the change in BC measures, distributions, and profiles across age decades were investigated. Age-, sex-, and height-adjusted body composition reference curves were calculated and made publicly available in a web-based z-score calculator (https://circ-ml.github.io).](https://img.auntminnieeurope.com/mindful/smg/workspaces/default/uploads/2026/05/body-comp.XgAjTfPj1W.jpg?auto=format%2Ccompress&fit=crop&h=112&q=70&w=112)