“Breast pain alone isn’t a sign of breast cancer.”
That’s a notice that Dr. Matthew Wallis, senior member of the Breast Cancer Unit in Cambridge, U.K., would like to see in neon characters on breast imaging centers and websites across the country.
“For almost everybody, breast cancer is not painful, and nobody in Cambridge seems to understand that, at least not the patients,” he told delegates at the session on "Symptomatic Breast Imaging" at ECR 2026 where he discussed his views on the role of imaging for breast pain.
“Breast pain is normal. Over 50% of women will experience [it] in their lives and studies have found no evidence of greater risk of cancer in women with breast pain. In fact, for every cancer found in a woman referred with only breast pain you do at least nine benign biopsies,” he added.
Pointing to a study from the U.K. in 2022, he revealed that in a cohort of 10,830 women in a symptomatic breast cancer unit, among women referred for only breast pain, cancer incidence was 0.4%, lower than the background rate of cancer in asymptomatic women undergoing breast cancer screening at 0.8%.
But what about the reassurance that comes with a normal image? Wallis, recipient of the European Society of Breast Imaging (EUSOBI) gold medal in 2025, was skeptical and suggested that imaging could have the opposite effect.
 Dr. Matthew WallisCourtesy of Frances Rylands-Monk/ESR
Dr. Matthew WallisCourtesy of Frances Rylands-Monk/ESR
“There is no evidence that says [imaging] is any more reassuring than a proper clinical examination or explanation. In fact evidence suggests that it causes anxiety, stress, and uncertainty. Some studies show that imaging during an initial visit means that it is more likely to be used again later on,” he said.
In the discussion one delegate challenged this notion, noting that chatting with patients post-ultrasound did indeed reassure them but Wallis countered that this exchange could be provided by others, as radiologists were already overworked and under-resourced.
Contradictory guidance
Guidelines on imaging for breast pain from different bodies are conflicting, Wallis noted. The American College of Radiology (ACR) states that some sort of imaging should be used in women with breast pain alone for “clinically significant” pain such as focal or noncyclical, despite studies and evidence that would counter this indication, according to Wallis.
Meanwhile in the 2025 U.K. guidelines, the Royal College of Radiologists (RCR) and Association of Breast Surgery (ABS) agreed that imaging is not indicated in isolated breast pain if there are no other associated signs.
So how should the patient with only breast pain be managed in his opinion?
Wallis listed several steps: first, reassure the patient that breast pain does not signify breast cancer and breast cancer generally isn’t painful. Next, advise patients on the importance of a well-fitting bra that supports in the right places, and advocate judicious use of pain relief. Paracetamol, and if pain is likely to be musculoskeletal-related, topical anti-inflammatory wipes should be used before any pain-triggering activities and before bedtime. Finally, gentle dietary advice on fat and caffeine intake could be made, but only in cases of excessive use.
“This will lower the risk of esophageal cancer and if it helps the breast pain, then great!” he said.
Opportunistic screening
He noted that “Nature” cures most breast pain within three or four cycles.
“In summary there is no role for imaging in isolated breast pain,” Wallis noted.
But what about its role in opportunistic screening?
“Remember, not attending a first screen increases your chance of dying by 40%. So if you can, get [patients] to attend the first mammogram and subsequent screens,” he urged.
He pointed to "absymal" screening coverage across the U.K. and Europe’s member states, but warned against breast pain imaging being used as a form of opportunistic screening.
He explained that in Cambridge every woman over 40 years entering the unit gets a mammogram regardless of presence or absence of a lump or any other symptoms, before they’ve seen a clinician. While this strategy eases workflow, Wallis noted that the unit provides no information about the pros and cons of screening.
“I’m not sure that’s appropriate and I do wonder whether opportunistic screening without information equates to paternalistic care,” he told delegates, urging anyone anxious about the amount of information provided to patients on the topic to email him, ahead of the Cambridge Conference on Breast Cancer Imaging, 16 and 17 June 2026.
Discordant findings
In the session chaired by Dr. Maria Adele Marino from Messina University, Italy, Prof. Isabelle Thomassin-Naggara, head of imaging at Tenon Hospital, Paris, revealed how to act when pathology and imaging findings are discordant.
 Prof. Isabelle Thomassin-NaggaraCourtesy of Frances Rylands-Monk/ESR
Prof. Isabelle Thomassin-NaggaraCourtesy of Frances Rylands-Monk/ESR
“This situation must be handled carefully as it carries the risk of missing malignancy. Optimal communication between the radiologist, pathologist and surgeon is crucial,” noted Thomassin-Naggara, who is also president of France’s national society of women’s imaging, SIFEM, and board member of EUSOBI.
Understanding the causes of discordance, the impact on patient outcomes, and what action must be taken to ensure timely and accurate diagnosis while avoiding unnecessary procedures is vital, she added.
Discordance can occur when samples are too few and miss malignancy, while core-needle/micro-biopsies compared to other biopsy methods are also more likely to result in underestimation particularly when carried out without ultrasound guidance in real time. Underestimation is also higher in large non-mass lesions than in mass lesions, she said.
 Pathology and radiology should use standardized tables to describe lesions and locations, noted Prof. Isabelle Thomassin-Naggara.Courtesy of Frances Rylands-Monk/ESR
Pathology and radiology should use standardized tables to describe lesions and locations, noted Prof. Isabelle Thomassin-Naggara.Courtesy of Frances Rylands-Monk/ESR
Over 4% of discordance in interventional radiology for breast, skin, and colon procedures is caused by mislabeling, such as wrongly identifying the patient, or biopsying the wrong site, noted Thomassin-Naggara. To avoid the former, two unique patient identifiers are needed, and samples must be labelled in the presence of the patient.
More accurate targeting of biopsy sites could be achieved through use of the same standardized tables by radiology and pathology, she noted, adding that radiology reports needed to precisely describe lesions and their locations, and pathology reports to mention the presence of microcalcifications.
Case study
“You need to listen to your patient, especially when this patient has already had a cancer,” she noted pointing to a case of an 80-year-old patient with history of breast cancer, and flagging the importance of markers for small lesions.
In this case there was no palpable lesion but the patient insisted something felt changed. On mammography and tomosynthesis, a mass was discernible on the side where she had undergone surgery, while on ultrasound, a suspicious lesion was found in both breasts and both lesions were deemed BI-RADS 4C.
The patient underwent core-needle biopsy without markers, with two samples taken from the smaller lesion on the right, which yielded a pathology finding of a complex adenofibroma.
On the left, three samples provided a pathology result as fusiform and inflammatory cells. Given the patient’s history, the BI-RADS 4C category, and the discordance with pathology, the next step was MRI.
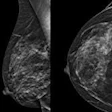
 80-year-old patient with history of breast cancer had a mass in the operated breast as shown here on mammography and tomosynthesis. Ultrasound found lesions in both breasts and these were deemed BIRADS 4C. Patient was biopsied without markers.Courtesy of Frances Rylands-Monk/ESR
80-year-old patient with history of breast cancer had a mass in the operated breast as shown here on mammography and tomosynthesis. Ultrasound found lesions in both breasts and these were deemed BIRADS 4C. Patient was biopsied without markers.Courtesy of Frances Rylands-Monk/ESR
 After biopsy, and findings of adenofibroma (r) and fusiform and inflammatory cells (l), MRI sequences showed suspicious lesions, and a second biopsy revealed invasive ductal carcinoma in the left breast.Courtesy of Frances Rylands-Monk/ESR
After biopsy, and findings of adenofibroma (r) and fusiform and inflammatory cells (l), MRI sequences showed suspicious lesions, and a second biopsy revealed invasive ductal carcinoma in the left breast.Courtesy of Frances Rylands-Monk/ESR
On MRI, both the left and right breast looked suspicious with ultrafast and diffusion sequences and another biopsy was ordered. This time vacuum-assisted biopsy revealed pseudoangiomatous stromal hyperplasia (PASH) on the right (imaging follow-up at nine months revealed nothing else) and infiltrating ductal carcinoma on the left. The patient was treated with surgery.
Markers could have improved accuracy, noted Thomassin-Naggara, who reminded delegates of the need for systematic use of post-biopsy markers in lesions of less than 5 mm, and in cystic or intraductal lesions and for targeted ultrasound after MRI.
To guide the multidisciplinary team’s decision-making on diagnosis, treatment planning and follow-up care, radiologists must be assertive, she noted:
- Be well prepared for the multidisciplinary team (MDT)
- Provide contextual information in the imaging report
- Present clear findings (with consistency between modalities)
- Use appropriate BI-RADS terminology
- Clarify uncertainty (position of calcifications, mass)
- Use visual aids (drawings) if multiple biopsies