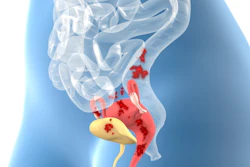
Endometriosis can present in many different organs and areas of the reproductive system, as well as nonreproductive, so radiological diagnosis must be systematic to not miss any locations within the pelvis. This was the view of Prof. Isabelle Thomassin-Naggara, chair of the ECR multidisciplinary session “Different faces of endometriosis: a diagnostic challenge.”
“Endometriosis is a complex disease with different symptoms notably chronic pelvic pain and also infertility, so diagnosing it without a big delay is one of the main challenges we have,” she said, adding that image analysis needed to consider functional features and physiopathology.
She noted that for adnexal endometriosis there was huge value in combining techniques for diagnosis, using transvaginal ultrasound (TVUS) as a first-line tool for typical endometrioma and MR for atypical disease. It remained vital therefore for radiologists to learn to read MRI using ESUR guidelines, available online and in a dedicated mobile app, so as not to miss any locations.
First-line tools
Dr. Sue Freeman, a consultant radiologist at Cambridge University Hospitals echoed this view in her presentation on the role of ultrasound and MRI in adnexal endometriosis management and the imaging features of malignant transformation.
“Ultrasound is a primary diagnostic tool in endometriosis, MRI is useful for problem solving and malignant transformation while rare, is essential not to miss,” she noted.
 Dr. Sue Freeman
Dr. Sue Freeman
She drew delegates’ attention to the four-step systematic approach for evaluating suspected endometriosis, the first step being to rule in or out the presence of adenomyosis and endometrioma.
“I think it would be fair to say that the first step is possibly the only step that some sonographers would use for looking at the pelvis and this isn’t good enough because just looking at the uterus for adenomyosis or the ovaries for an endometrioma would mean we would miss so much endometriosis if we stopped there. As we know only 20% to 40% of people with endometriosis will have an endometrioma,” she noted.
The second step is to start to gently move the uterus and the ovaries to find adhesions and site-specific tenderness. For adnexal endometriosis these first two steps are the most important, she added.
Endometrioma often presents with homogenous low level echoes and ground glass appearance, and also with hyperechoic mural foci -- which are probably little blood clots, she noted. More atypical appearance include septations, mural nodules (clots), fluid-fluid levels and no Doppler flow.
 Dr. Sue Freeman
Dr. Sue Freeman
“With ultrasound we can make blood clots wobble when soft tissue doesn’t do that. In cases of doubt we could use interval ultrasound or move on to MRI,” she said.
On T1- and T2-weighted MRI, adnexal endometriosis shares many of the same features visible on ultrasound such as black spot sign -- the equivalent of the hypoechoic foci, kissing ovaries, and hydrosalpinx and hematosalpinx. There will also be a 40% chance of seeing endometriotic deposits so radiologists should make a careful search of the pelvis.
But how can we distinguish between endometrioma and hemorrhagic cysts?
“We can usually tell [them apart] as cysts have a lace-like reticular pattern and sometimes a solid component where the clot is retracting with a concave shape and no vascularity. Importantly these often resolve within two weeks to two months,” she noted.
While rare, cancer must not be overlooked. On ultrasound, the commonest which are clear cell- and endometrioid carcinoma, will look like solid nodules with vascularity.
“These typically occur in larger endometriomas. We would see a soft tissue nodule that would enhance with gadolinium and restrict with diffusion-weighted imaging,” she noted. “It’s very important to use subtraction imaging to detect the enhancement of the nodule against the brightness of the edometrioma.”
ESUR Guidelines
Radiologists must look for different MRI phenotypes when imaging for endometriosis to avoid missing lesions, and these include fibrotic plaques or nodules, cystic or hemorrhagic components, adhesions with or without nodules, and distortion of normal anatomy, according to Dr. Miriam Dolciami, a radiologist at Agostino Gemelli University Polyclinic, Rome, whose presentation on deep endometriosis revealed how to read an MRI so as to not miss any location.
“The radiologist’s challenge is to see all features, from subtle signs in an almost negative scan -- to battlefield MRI,” she noted.
New elements to the ESUR 2025 consensus on endometriosis such as compartment-based image analysis, a standardized lexicon and the use of classification will help radiologists stay vigilant and improve detection and patient management, she added.
She pointed to her own recipe for not missing locations:
1. Appropriate MR protocol without unnecessary sequences.
2. Compartment-based scan analysis to ensure systematic evaluation of all sites.
3. Structured reporting with standardized terminology to improve detection, communication and surgical planning.
“Structured and surgery-oriented reporting ensures key features and sites are not overlooked, saves time, provides clarity in interpretation and enhances surgical decision-making and patient consultation,” she noted.
She flagged the "must-have" MR scans for detecting deep endometriosis which comprise at least two different 2D T2-weighted planes (sagittal and axial), a T1-weighted/T1-weighted-FS or 3D Dixon technique, and a sequence that visualizes the kidneys, with other optional sequences depending on the specific question.
Compartment-based analysis of images will help diagnosis and extra-pelvic sites such as the abdominal wall, sigmoid, cecum, appendix, small bowel, and diaphragm should not be missed, she added.
 Dr. Miriam Dolciami
Dr. Miriam Dolciami
Accurate diagnoses
The management of endometriosis has changed radically in the last 20 years, according to Dr. Ludovic Muzii, a gynecologist from Sapienza Hospital in Rome.
“Thirty years ago when I was a resident, [endometriosis] was a surgical disease in terms of diagnosis and treatment, and there were bad drugs with terrible side effects. Now with new drugs, new surgical techniques, improvements in IVF and in imaging, it is no longer a surgical disease,” he told delegates.
With the delay in diagnosis being four to eleven years from symptom onset, Muzii noted that the goal for gynecologists was not early diagnosis but an accurate one, and interaction with the imaging expert was not so much to plan surgery but to better plan management, which in the majority of cases was now medical therapy or IVF, he noted.
“The goal is not to eradicate the disease but rather to treat the symptoms, improve quality of life, and preserve fertility through a tailored approach based on many parameters,” he said.
He noted that imaging in a clinical context could evaluate ovarian reserve, protect fertility, identify and describe deep disease, predict surgical complexities and improve surgical outcomes.
“Optimal management requires close collaboration between the imaging expert and the reproductive endocrinology and infertility specialist,” he said.