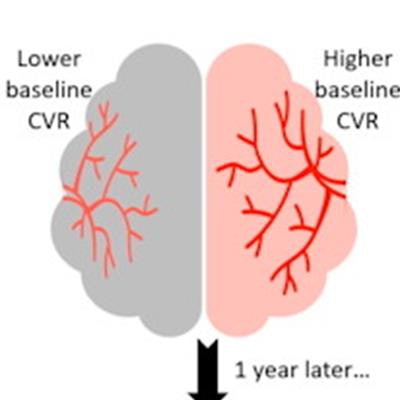
MRI shows that cerebrovascular (CVR) reactivity is a predictor of small-vessel disease severity after one year in patients with mild stroke, according to research presented on 7 June at the International Society of Magnetic Resonance in Medicine (ISMRM) annual meeting.
In her presentation, doctoral candidate Emilie Sleight of the University of Edinburgh in Scotland discussed her team's research, which found that CVR impairment is linked to small-vessel disease burden and predicts worse burden from white-matter hypersensitivities and perivascular space after one year.
"This work showed that CVR is a potential biomarker for small-vessel disease and should be considered for future studies and clinical trials," she said.
Sporadic cerebral small-vessel disease is the cause of about 20% of strokes and most vascular dementias, Sleight noted. No treatment is available for this, and understanding of the mechanisms behind the disease remains poor.
MRI can visualize brain tissue damage caused by small vessel disease, including white-matter hyperintensities, lacunes, microbleeds, perivascular spaces, and atrophy. Because small-vessel disease is of vascular origin, there may be a relationship between MRI findings and vascular dysfunction, Sleight said.
Her group sought to explore CVR reactivity any links between impairment and tissue damage and the progression of such damage one year after stroke diagnosis. They conducted a study that used data from the university's Mild Stroke Study 3 (MSS3), which recruited 182 small-vessel disease patients with minor ischemic stroke (stroke score of 1 out of 4). Within three months after having a stroke, the patients presented for baseline 3-tesla MR imaging, which the researchers used to quantify CVR reactivity; they returned for follow-up after a year. MRI exams visualized patients' intermittent breath intake of carbon dioxide (CO2) gas and medical gas to map CVR and acquired blood oxygen level-dependent images.
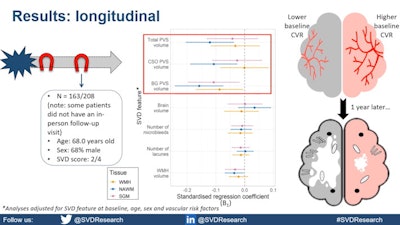 Research from the University of Edinburgh presented at the ISMRM annual meeting found that MRI links cerebrovascular reactivity and small-vessel disease in mild stroke patients. Here, data shows that those with lower reactivity have higher volumes of white matter hyperintensity and perivascular spaces. Image courtesy of Emilie Sleight.
Research from the University of Edinburgh presented at the ISMRM annual meeting found that MRI links cerebrovascular reactivity and small-vessel disease in mild stroke patients. Here, data shows that those with lower reactivity have higher volumes of white matter hyperintensity and perivascular spaces. Image courtesy of Emilie Sleight.Patients with lower CVR reactivity at baseline had higher white matter hyperintensity volumes and a higher number of lacunes and microbleeds, the group reported, but there were no significant differences in brain volumes or perivascular space volumes between high and low CVR activity.
For longitudinal analysis, one year after baseline analysis, the team included data from 163 patients with median small-vessel disease score of two. It found increased white-matter hyperintensity volumes in those with lower CVR, suggesting underlying damage that was not visible at baseline imaging. These results remained true even after adjusting for factors such as sex, age, and vascular risk. Additionally, it reported that those with lower CVR reactivity at baseline saw a significant increase in perivascular space volume.
Sleight said she and her team hope future research will refer to these findings to better understand the mechanisms behind small-vessel disease develop a successful treatment method for it, adding that they plan to look next at CVR data at a follow-up of three years.