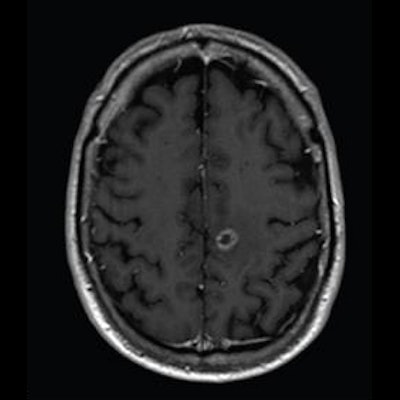
A 25% reduced dose of gadobutrol for contrast-enhanced brain MRI is "noninferior" to a standard dose of gadoterate, according to a study published on 17 June in the American Journal of Roentgenology.
The results could reduce contrast dose exposure in patients who undergo multiple exams with gadolinium-based contrast agents, said study corresponding author Dr. Jan Endrikat, PhD, of the University Medical School of Saarland in Germany in a statement released by the American Roentgen Ray Society (ARRS).
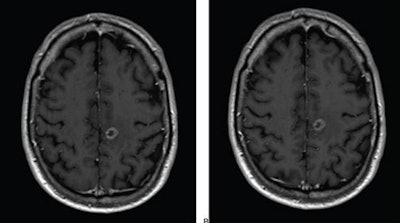 Axial T1-weighted MR images obtained using (A) standard-dose gadoterate and (B) reduced-dose gadobutrol four days later. Mean score across three readers for standard-dose gadoterate and reduced-dose gadobutrol was 3.4 and 3.4, respectively, for subjective lesion enhancement; 3.5 and 3.4, respectively, for lesion border delineation; and 2.9 and 2.9, respectively, for lesion internal morphology. Image and caption courtesy of the ARRS.
Axial T1-weighted MR images obtained using (A) standard-dose gadoterate and (B) reduced-dose gadobutrol four days later. Mean score across three readers for standard-dose gadoterate and reduced-dose gadobutrol was 3.4 and 3.4, respectively, for subjective lesion enhancement; 3.5 and 3.4, respectively, for lesion border delineation; and 2.9 and 2.9, respectively, for lesion internal morphology. Image and caption courtesy of the ARRS.The study included 141 patients with known or suspected central nervous system conditions who underwent contrast-enhanced brain MRI with standard-dose gadoterate (0.1 mmol/kg); if a lesion was found, the patients underwent a second MRI with reduced-dose gadobutrol (0.075 mmol/kg) within 15 days.
"Comparison of reduced-dose gadobutrol and standard-dose gadoterate versus unenhanced imaging demonstrated noninferiority using 20% margin for three primary efficacy measures: subjective lesion enhancement, lesion border delineation, lesion internal morphology," the ARRS said.










![Overview of the study design. (A) The fully automated deep learning framework was developed to estimate body composition (BC) (defined as subcutaneous adipose tissue [SAT] in liters; visceral adipose tissue [VAT] in liters; skeletal muscle [SM] in liters; SM fat fraction [SMFF] as a percentage; and intramuscular adipose tissue [IMAT] in deciliters) from MRI. The fully automated framework comprised one model (model 1) to quantify different BC measures (SAT, VAT, SM, SMFF, and IMAT) as three-dimensional (3D) measures from whole-body MRI scans. The second model (model 2) was trained to identify standardized anatomic landmarks along the craniocaudal body axis (z coordinate field), which allowed for subdividing the whole-body measures into different subregions typically examined on clinical routine MRI scans (chest, abdomen, and pelvis). (B) BC was quantified from whole-body MRI in over 66,000 individuals from two large population-based cohort studies, the UK Biobank (UKB) (36,317 individuals) and the German National Cohort (NAKO) (30,291 individuals). Bar graphs show age distribution by sex and cohort. BMI = body mass index. (C) After the performance assessment of the fully automated framework, the change in BC measures, distributions, and profiles across age decades were investigated. Age-, sex-, and height-adjusted body composition reference curves were calculated and made publicly available in a web-based z-score calculator (https://circ-ml.github.io).](https://img.auntminnieeurope.com/mindful/smg/workspaces/default/uploads/2026/05/body-comp.XgAjTfPj1W.jpg?auto=format%2Ccompress&fit=crop&h=112&q=70&w=112)





