Using a clinical decision model developed by Dutch researchers for pediatric wrist trauma could cut unnecessary emergency x-ray imaging for the condition by 22% -- thereby reducing children's radiation exposure and healthcare costs, according to a study published online in Pediatric Radiology.
Wrist trauma is one of the most common reasons for children's visits to the emergency department, and over the past four decades, the number of distal forearm fractures, the most common type of injury following wrist trauma, has increased, wrote the group led by Dr. Annelie Slaar of the University of Amsterdam.
 Dr. Annelie Slaar from the University of Amsterdam.
Dr. Annelie Slaar from the University of Amsterdam.The rise in incidence has sparked a surge in cost -- to the tune of more than $2 billion per year in the U.S. -- in part because more x-rays are being performed to diagnose the injury. But no guidelines exist to help emergency physicians determine when x-ray imaging of wrist trauma is appropriate, and in a previous study, Slaar and colleagues found that only 51% of x-rays acquired for this reason actually showed a fracture (Pediatr Radiol, August 23, 2015).
"In our previous work, we found that half of the pediatric patients who received x-ray for blunt trauma of the wrist had normal radiographs," Slaar told AuntMinnie.com via email. "So for this study, we sought to develop and test a clinical decision rule that would help physicians decide whether an x-ray is really needed."
Wrist rules
The study included 787 children who received x-rays for wrist trauma between April 2011 and April 2014. The children's median age was 11 years. They were divided into two groups: one served as the cohort for the development of the clinical protocol (408 patients) and the other as the cohort for the protocol's validation (379 patients).
Slaar's team included six variables in its decision model, which it called the Amsterdam Pediatric Wrist Rules:
- Age
- Swelling of the forearm near the wrist
- Visible deformation
- Tenderness at palpation
- Tenderness at palpation of the anatomical snuffbox (the triangular depression at the wrist when the thumb is fully extended)
- Painful supination
Of the total number of children included in the study, 364 had a distal forearm fracture (46.3%) and 423 did not (53.7%). By group, 194 children in the protocol development cohort (47.5%) and 170 in the validation group (44.9%) had a distal forearm fracture.
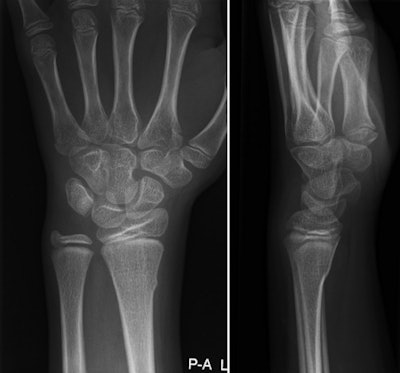 Buckle fracture of the distal radius in a 9-year-old girl. Left, posteroanterior view; right, lateral view. Images courtesy of Dr. Annelie Slaar.
Buckle fracture of the distal radius in a 9-year-old girl. Left, posteroanterior view; right, lateral view. Images courtesy of Dr. Annelie Slaar.The six-variable clinical model had a specificity of 95.9% for detecting distal forearm fractures. In 2009, 8,930 per 100,000 children presented with a wrist injury; using the protocol would have reduced the number of requested x-rays by almost 2,000 per 100,000, or 22%, the authors wrote. The protocol also could have reduced healthcare costs by 96,000 euros ($108,830 U.S.) per 100,000 children annually.
As for the clinical decision model's limitations, it would have missed 4% of the fractures in the validation cohort -- although the treatment and prognosis would not have been influenced by a missed or delayed diagnosis, according to Slaar and colleagues. And the protocol's specificity was fairly low, at 37.3%.
"We could have generated a higher specificity by using another threshold, but this would have led to a decrease in the sensitivity and thus an increase of missed fractures," they wrote. "Since we aimed to reduce the number of requested wrist radiographs, a threshold compromise between missed fractures and reduction of radiographs was chosen."
In any case, the study demonstrates that this type of clinical protocol is useful, the researchers concluded. They plan to conduct another study that will evaluate the effect of the protocol on the number of x-rays, emergency department wait times, and healthcare costs, with the decision tool available as a smartphone application.
"Our results show that unnecessary wrist imaging in children can be prevented -- which will reduce radiation exposure to these patients, healthcare costs, and workflow inefficiencies," Slaar told AuntMinnie.com. "We look forward to conducting our implementation study."