
In the future, it will be essential to investigate the accuracy of chest reporting by radiographers more extensively, particularly throughout implementation into clinical practice and in comparison with senior radiologists, according to U.K. researchers who have just reported positive findings from a new study into role extension.
With its inception in 1994, Canterbury Christ Church University became the first center in the world to offer an accredited program for radiographers. Keith Piper, the program director of postgraduate clinical reporting at the university, and colleagues analyzed the objective structured examination (OSE) results of the first six cohorts of 40 radiographers who successfully completed the program in reporting of adult chest radiographs.
"The majority of the radiographers included in this study are now reporting adult chest examinations in clinical practice from a range of referral sources," they noted in an article posted online on 13 February by Radiography. "Implementation into practice is subject to routine audit and governance processes including an agreed scheme of work. Attendance at further clinico-radiological and multidisciplinary team meetings, as part of continuing professional development, should be facilitated/supported to enhance their reporting accuracy as advanced practitioners or consultant radiographers."
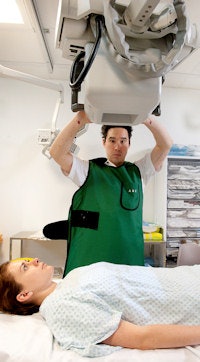 Following an accredited postgraduate education program, radiographers can correctly identify normal chest radiographs and provide a report on abnormal appearances. This and the home page image provided courtesy of Charles Fox/Barts Health National Health Service (NHS) Trust.
Following an accredited postgraduate education program, radiographers can correctly identify normal chest radiographs and provide a report on abnormal appearances. This and the home page image provided courtesy of Charles Fox/Barts Health National Health Service (NHS) Trust.
The authors studied 100 chest radiographs, which included a range of abnormal cases (prevalence of abnormal examinations approximated 50%) and also constituted cardiac, pulmonary, pleural, interstitial, inflammatory, neoplastic, and traumatic appearances on patients referred from a range of referral sources. Normal variants and incidental findings also were included. True/false positive and negative fractions were used to mark the responses, which were also scored for agreement with the previously expected answers based on agreement between three consultant radiologists' reports.
The mean sensitivity and specificity rates for all six cohorts (4,000 reports) were 95.4% and 95.9%, respectively. The mean agreement rate was 89%, and the most common errors were related to heart size, hilar enlargement or pleural effusion (false positive), and skeletal appearances or pneumothoraces (false negative).
Overall, the results suggest that this group of 40 radiographers can report on the broad range of adult chest pathologies with satisfactory accuracy under examination conditions. Although lessons can be learned from these initial experiences, generally the types of errors made are likely to be similar to those made in the practical setting by senior radiologists of varying experience.
"These OSE results suggest therefore that in an academic setting, and following an accredited postgraduate education program, this group of radiographers has the ability to correctly identify normal chest radiographs and are able to provide a report on the abnormal appearances to a high standard," the authors wrote. "Further work is required to confirm the clinical application of these findings."
According to Piper, who is also principal lecturer in the department of allied health professions at Canterbury, interpreting the chest x-rays in the context of an academic examination may have influenced the decision threshold of the radiographers. Some of the sample chose to err on the side of caution, especially given the relative consequence of a false-negative cancer diagnosis, he stated.
It is possible that benign lesions, such as hamartomas, scars, and granulomas, found on essentially normal images in the OSE were described as abnormal lung lesions due to clinical review bias. In addition, there are several normal variants such as nipple shadows, skin lesions, and superimposition of vascular shadows that may simulate lung nodules, and in these cases a clinical history of "hemoptysis" or "smoking history" may have influenced the students' decision, he explained.
"The influence of clinical history on chest x-ray interpretation is equivocal; several studies have suggested this leads to improved accuracy, and other studies found no statistically significant difference in chest x-ray interpretation undertaken with or without the relevant clinical history," the researchers wrote. "It is 'generally accepted that access to previous images and reports is useful' when interpreting x-rays, and this has been suggested as a method of error reduction. In the current study, the radiographers did not have access to previous x-rays, which may have contributed to the higher false-positive rate for pulmonary nodules; a lesion that is unchanged over a significant time is more likely to represent a benign pathology."
A further limitation of this study was the absence of an external reference standard to provide incontrovertible confirmation -- by repeated follow-up or further imaging, such as CT -- of normality or the presence and type of pathology, including the progression of any disease. In the absence of such evidence, concordant reports independently produced by three consultant radiologists may be used to assess other observers in this way, noting that the performance of an individual undertaking a reporting role should be indistinguishable from the performance of an "average" practitioner or specialist, they concluded.











![Overview of the study design. (A) The fully automated deep learning framework was developed to estimate body composition (BC) (defined as subcutaneous adipose tissue [SAT] in liters; visceral adipose tissue [VAT] in liters; skeletal muscle [SM] in liters; SM fat fraction [SMFF] as a percentage; and intramuscular adipose tissue [IMAT] in deciliters) from MRI. The fully automated framework comprised one model (model 1) to quantify different BC measures (SAT, VAT, SM, SMFF, and IMAT) as three-dimensional (3D) measures from whole-body MRI scans. The second model (model 2) was trained to identify standardized anatomic landmarks along the craniocaudal body axis (z coordinate field), which allowed for subdividing the whole-body measures into different subregions typically examined on clinical routine MRI scans (chest, abdomen, and pelvis). (B) BC was quantified from whole-body MRI in over 66,000 individuals from two large population-based cohort studies, the UK Biobank (UKB) (36,317 individuals) and the German National Cohort (NAKO) (30,291 individuals). Bar graphs show age distribution by sex and cohort. BMI = body mass index. (C) After the performance assessment of the fully automated framework, the change in BC measures, distributions, and profiles across age decades were investigated. Age-, sex-, and height-adjusted body composition reference curves were calculated and made publicly available in a web-based z-score calculator (https://circ-ml.github.io).](https://img.auntminnieeurope.com/mindful/smg/workspaces/default/uploads/2026/05/body-comp.XgAjTfPj1W.jpg?auto=format%2Ccompress&fit=crop&h=112&q=70&w=112)




