Concerns about the possible link between gadolinium-based contrast agents and nephrogenic systemic fibrosis (NSF) have led to an increase in noncontrast-enhanced MR angiography (MRA), particularly for abdominal imaging, according to a paper in the October issue of the European Journal of Radiology.
MRA is particularly relevant for imaging renal arteries and portal and hepatic veins, especially for patients with decreased renal function or renal disease, noted lead study author Mitsue Miyazaki, PhD, acting director of MRI for the Toshiba Medical Research Institute (EJR, October 2011, Vol. 80:1, pp. 9-23).
Miyazaki and co-author Dr. Hiroyoshi Isoda, from the department of diagnostic imaging and nuclear medicine at Kyoto University in Japan, also found that abdominal 3-tesla MRA can be more effective than 1.5-tesla MRA, because the greater magnet strength offers high signal intensities and longer T1 values of tissue signals to produce higher resolution images. The authors, however, did caution that there are limitations to 3-tesla MRA due to wavelength issues at the higher magnet strength and specific absorption rate limits, which "require special consideration in imaging of the abdomen."
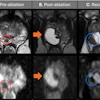
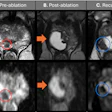
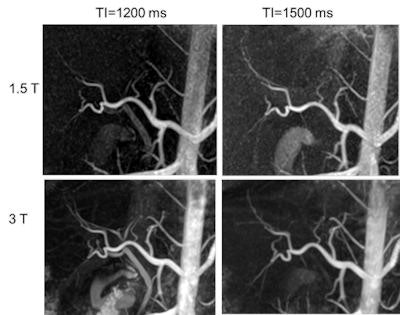 Hepatic artery using time-spatial labeling inversion pulse (time-SLIP) at different TI times at both 1.5- and 3-tesla. Note that long T1 at 3 tesla gives better background suppression even at TI=1500 ms. All images courtesy of Mitsue Miyazaki, PhD, and Dr. Hiroyoshi Isoda.
Hepatic artery using time-spatial labeling inversion pulse (time-SLIP) at different TI times at both 1.5- and 3-tesla. Note that long T1 at 3 tesla gives better background suppression even at TI=1500 ms. All images courtesy of Mitsue Miyazaki, PhD, and Dr. Hiroyoshi Isoda.NSF incidence
NSF can be avoided when physicians use low doses of gadolinium-based contrast agents for patients with an estimated glomerular filtration rate of between 30 and 59 mL/min/m2 and if they never administer these agents to patients with renal disease and an estimated glomerular filtration rate of less than 30 mL/min/m2, according to previous studies.
Those strict guidelines have made noncontrast-enhanced renal MRA the imaging technique of choice for patients who may be at risk for NSF or are susceptible to adverse reactions from a gadolinium-based contrast agent.
Hepatic venous imaging, for example, is a necessity for patients about to have surgical procedures, such as a liver transplantation. Traditionally, contrast-enhanced CT or MRI has been used for preoperative imaging of the hepatic vascular anatomy, but gadolinium-based contrast agents can have adverse side effects, particularly for patients with inadequate renal function.
Contrast-enhanced imaging also may be problematic between the hepatic vein and surrounding tissue because of strong background signal from the liver parenchyma and the portal veins in the hepatic venous phase. Even gadolinium-enhanced MRA examinations can produce images with limited spatial resolution. To remedy the issue, the authors cited a study led by Dr. Katsuyoshi Ito from Toyo University in Japan, which used respiratory-gated time-spatial labeling inversion pulse (time-SLIP) to successfully visualize the hepatic veins and eliminate signal overlap from aorta and portal rates (Journal of Magnetic Resonance Imaging, May 2009, Vol. 29:5, pp. 1224-1229).
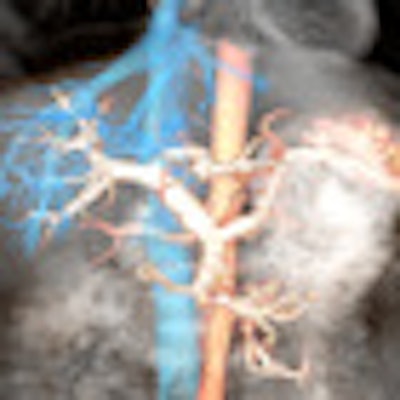
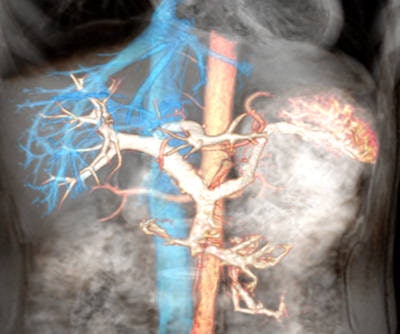 Overlaid images of aorta (red) superior vena cava with hepatic veins (blue) and portal venous system (white) using various time-SLIP techniques.
Overlaid images of aorta (red) superior vena cava with hepatic veins (blue) and portal venous system (white) using various time-SLIP techniques.Renal MRA
As for renal artery imaging by MRA, based on previous research, the authors recommend a wide field-of-view coronal scan using time-SLIP instead of a transaxial scan to visualize both renal arteries and accessory arteries.
"The transaxial scan achieves higher transaxial in-plane resolution and a better inflow effect than the coronal scan," they wrote. "This is because there is no pulse affecting the signal outside of the tagging area in the transaxial scan, whereas the coronal-orientation scan is affected by signals outside of the tagging area."
However, renal MRA does have limitations. Longer scans are required for patients with slow blood flow, and clinicians must consider the time it takes aortic blood to travel to the renal artery branches when determining the tagging pulse to ensure the MRA examination covers both kidneys.
In evaluating the capabilities of 3-tesla MRA, Miyazaki and Isoda reviewed previous research that found noncontrast-enhanced MRA to have many challenges as a result of the wavelength problem at higher field strengths. Still, the issues are not insurmountable.
3T versus 1.5T
A German study, led by Dr. Rotem Shlomo Lanzman from the department of radiology at University Hospital Düsseldorf, compared noncontrast-enhanced renal MRA at 1.5- and 3-tesla in 20 healthy volunteers with no history of renovascular disease.
Both1.5- and 3-tesla MRA were performed for all subjects with a maximum time of two weeks between imaging sessions. Researchers evaluated the image quality of axial and coronal maximum intensity projection reconstructions of the abdominal aorta and ostium of renal artery, the main renal artery, and both outside and inside branches of the renal parenchyma.
Lanzman and colleagues found no difference in the evaluation of the first and second branch segments, but discovered noncontrast-enhanced 3-tesla MRA exhibited a "significant improvement" over 1.5-tesla MRA of the third and the fourth branch segments. The authors credited the difference to longer T1 images of tissues at 3-tesla than at 1.5-tesla (American Journal of Roentgenology, March 2010, Vol. 194:3, pp. 794-798).
Abdominal MRA at 3-tesla is promising because of its high signal intensities and the longer T1 values of tissue signals, Miyazaki and Isoda concluded. However, the restrictions due to wavelength problems and specific absorption rate limits require special consideration in imaging of the abdomen.