Cardiac CT exams used to evaluate patients' heart health could deliver the added benefit of screening for osteoporosis -- an especially valuable use given the prevalence of the modality, according to a study published on 14 July in Radiology.
The relatively common use of chest CT is what makes it a good candidate for this kind of double duty, wrote a team led by Dr. Josephine Therkildsen of Herning Hospital in Denmark.
"Patients may undergo chest CT for numerous reasons," the team noted. "The prevalence of chest CT imaging provides unique opportunity for opportunistic [osteoporosis] testing."
Traditional ways of assessing osteoporosis risk include bone mineral density (BMD) testing using dual-energy x-ray absorptiometry (DEXA). But DEXA's uptake is low among eligible patients, the group noted -- a fact of some concern, since osteoporosis is treatable.
"Osteoporosis is a prevalent, underdiagnosed, and treatable disease associated with increased morbidity and mortality," Therkildsen said in a statement released by the RSNA. "Effective antiosteoporotic treatment exists and so, identifying individuals with greater fracture rate who may benefit from such treatment is imperative."
The researchers investigated whether cardiac CT could offer a way to screen for osteoporosis while also assessing heart health: Since these exams visualize the thoracic vertebrae, it's easy to add a bone mineral density test to the procedure, as it doesn't add time or radiation to the exam, the authors noted.
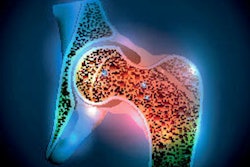
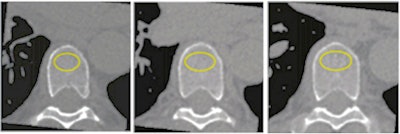 A participant's noncontrast-enhanced axial CT with volume of interest (yellow circles) in the trabecular bone compartment of three vertebrae for bone mineral density measurements. Images and caption courtesy of the RSNA.
A participant's noncontrast-enhanced axial CT with volume of interest (yellow circles) in the trabecular bone compartment of three vertebrae for bone mineral density measurements. Images and caption courtesy of the RSNA."We believe that opportunistic BMD testing using routine CT scans can be done with little change to normal clinical practice and with the benefit of identifying individuals with a greater fracture rate," Therkildsen said.
Their study included 1,487 patients who underwent cardiac CT for evaluation of heart disease, and who also had bone mineral density testing of three thoracic vertebrae using quantitative software. The group found that of the total study cohort, 179 (12%) individuals had very low bone mineral density.
These patients were followed for three years, and of these 179, 80 (5.3%) ended up being diagnosed with a fracture; of the 80 fractures, 31 were osteoporosis-related, Therkildsen and colleagues wrote. Patients with very low bone mineral density as detected by CT had a greater risk of fracture and osteoporosis-related fracture compared with their normal bone mineral density counterparts.
| Fracture risk based on CT-derived bone density values | ||
| Bone mineral density on CT | Unadjusted hazard ratio, any fracture | Unadjusted hazard ratio, osteoporosis-related fracture |
| Normal (> 120 mg/cm3) | -- | -- |
| Low (80-120 mg/cm3) | 1.5 | 5.5 |
| Very low (< 80 mg/cm3) | 2.6 | 8.1 |
"Our study shows that routine cardiac CT can be used to identify participants with low BMD who have a greater fracture rate," the team concluded.
Using cardiac CT for osteoporosis screening could increase compliance, wrote Dr. Miriam Bredella of Massachusetts General Hospital in Boston in an accompanying editorial.
"The majority of women and men who are eligible do not undergo osteoporosis screening, and many osteoporotic fractures occur in individuals who have never been screened," she wrote. "Given the low rates of osteoporosis screening by using [DEXA], the identification and validation of other techniques might increase the number of individuals undergoing screening."







![Overview of the study design. (A) The fully automated deep learning framework was developed to estimate body composition (BC) (defined as subcutaneous adipose tissue [SAT] in liters; visceral adipose tissue [VAT] in liters; skeletal muscle [SM] in liters; SM fat fraction [SMFF] as a percentage; and intramuscular adipose tissue [IMAT] in deciliters) from MRI. The fully automated framework comprised one model (model 1) to quantify different BC measures (SAT, VAT, SM, SMFF, and IMAT) as three-dimensional (3D) measures from whole-body MRI scans. The second model (model 2) was trained to identify standardized anatomic landmarks along the craniocaudal body axis (z coordinate field), which allowed for subdividing the whole-body measures into different subregions typically examined on clinical routine MRI scans (chest, abdomen, and pelvis). (B) BC was quantified from whole-body MRI in over 66,000 individuals from two large population-based cohort studies, the UK Biobank (UKB) (36,317 individuals) and the German National Cohort (NAKO) (30,291 individuals). Bar graphs show age distribution by sex and cohort. BMI = body mass index. (C) After the performance assessment of the fully automated framework, the change in BC measures, distributions, and profiles across age decades were investigated. Age-, sex-, and height-adjusted body composition reference curves were calculated and made publicly available in a web-based z-score calculator (https://circ-ml.github.io).](https://img.auntminnieeurope.com/mindful/smg/workspaces/default/uploads/2026/05/body-comp.XgAjTfPj1W.jpg?auto=format%2Ccompress&fit=crop&h=112&q=70&w=112)






