
As the safety of gadolinium MRI contrast is hotly debated, one of the challenges has been detecting gadolinium deposition in living patients. Canadian researchers may have found a solution to the dilemma with an x-ray fluorescence (XRF) system that can noninvasively detect trace elements of gadolinium in exposed individuals.
In a pilot study, the XRF system showed significantly greater concentrations of gadolinium in the tibia of patients who had undergone an MRI scan with a gadolinium-based contrast agent (GBCA) than in control subjects. The researchers also found a positive, though not statistically significant, correlation between the dose of GBCA administered to patients and the levels of gadolinium concentration measured in their bones, according to a paper published online December 13 in Radiology.
"The elevated level of gadolinium in bone of the exposed group compared to the control is definitely a concern to our research group and further verifies that there is a lot more to unfold regarding gadolinium deposition in the body," said lead author Michelle Lord, a doctoral candidate at the McMaster University School of Biomedical Engineering in Hamilton, Ontario.
Down to the bone
The retention of residual gadolinium in patients who receive MRI contrast has become one of the most controversial topics in radiology in recent years. While gadolinium deposition is a documented phenomenon, it's less clear what effect any retained gadolinium may have on the health of patients. Some individuals -- such as the wife of action movie star Chuck Norris -- have blamed gadolinium for a range of ailments they call gadolinium deposition disease; however, researchers and regulatory authorities counter that there's no definitive proof that gadolinium causes any health issues.
While much of the attention on gadolinium has focused on deposits in brain tissue, accumulation of the heavy metal in bone is also blamed for some patients' conditions. For example, a May 2016 study by Semelka et al surveyed 50 patients who attributed their symptoms to GBCA exposure. The most common complaint (78%) among the subjects was bone and joint pain. In addition, a 2016 study by Murata et al found that gadolinium levels in bone were 23 times higher than gadolinium levels in the brain at autopsy.
"These findings suggest a large proportion of gadolinium retained in the body is located in the skeleton," Lord and colleagues wrote in their paper. "Since bone has been shown to be a major storage site for gadolinium and since the brain is difficult to assess with noninvasive methods because it is covered by the skull, a noninvasive technique to measure gadolinium level in bone would be a useful tool to monitor gadolinium deposition while investigating the clinical implications of gadolinium deposition."
The XRF technology
Researchers at McMaster have been working on an x-ray fluorescence system that detects gadolinium since 2014 or so. Similar systems have been used at the medical center for more than 30 years to measure lead.
"Our research group has previously used x-ray fluorescence technology to noninvasively measure other trace elements in the body, such as lead and strontium," Lord wrote in an email to AuntMinnie.com. "The growing concern of the safety of gadolinium-based contrast agents made us want to explore gadolinium measurements in particular."
X-ray fluorescence involves the use of high-energy photons, such as gamma rays, to excite an element, such as gadolinium; this in turns initiates the production of x-rays that are characteristic of that target. McMaster's XRF detector features four separate germanium elements in a cloverleaf formation, with each detector attached to its own set of pulse-processing electronics.
"The specific energy of our excitation source makes it ideal to excite any present gadolinium in the body and measure the resultant fluorescent x-rays," Lord explained. "Previous measurements of gadolinium in bone have been invasive, requiring a sample of bone to be removed from the body, or have been performed on an autopsy sample. A measurement technique such as x-ray fluorescence has the potential to provide information on gadolinium deposition in the body without any invasive procedures."
Gadolinium target
For the study published in Radiology, the researchers included six subjects from a study performed five years earlier that involved the injection of gadolinium contrast in healthy volunteers, as well as five people with self-reported GBCA exposure. These individuals were matched with 11 control subjects with no history of GBCA exposure.
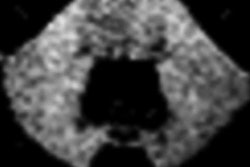
 Gadolinium retention was measured in the tibia with subjects placing their leg directly in front of the XRF source. The measurement was performed with a 180° set-up geometry. Image courtesy of Radiology.
Gadolinium retention was measured in the tibia with subjects placing their leg directly in front of the XRF source. The measurement was performed with a 180° set-up geometry. Image courtesy of Radiology.Of the 11 individuals exposed to gadolinium, eight had received gadobutrol (Gadovist, Bayer), one had received gadoteridol (ProHance, Bracco Imaging), one had received gadodiamide (Omniscan, GE Healthcare), and the status for one patient was unknown. The researchers also administered one dose of gadobutrol (1.0 mmol/mL) to the control subjects to test the method of prompt gamma neutron activation analysis (PGAA) to measure gadolinium deposition in muscle tissue.
The researchers specifically chose the tibia to measure gadolinium deposition because of its location in an extremity and its relatively thin layer of overlying tissue. Each subject sat with his or her leg held against a collimated cadmium source for 30 minutes.
Lord and colleagues discovered that gadolinium (Gd) concentration in bone was visibly higher in the group exposed to GBCAs (2.6 micrograms Gd/g bone mineral ± 1.6) than in the control group (-1.23 micrograms Gd/g bone mineral ± 0.94) (p = 0.05).
(A statistical variation can result in a negative gadolinium concentration, the researchers explained, hence the negative result of gadolinium concentration in the healthy control group.)
There also was a positive, though not statistically significant, correlation between the dose of GBCA administered and the gadolinium concentration measured in the bone. Gadolinium concentration in the bone increased by 0.39 micrograms Gd/g bone mineral (± 0.14) for each 1 mL of contrast administered (R2 = 0.41).
"Our ability to detect gadolinium in an individual five years after one injection may suggest that bone may act as a long-term storage site for gadolinium in the body," the researchers wrote. "Overall, our results indicate that our XRF system enables detection of gadolinium in our small pilot study."
Cautionary note
Lord and colleagues cautioned that the results are preliminary and more research is needed to validate them, especially given the small number of subjects.
"This was a small pilot study containing 11 individuals in each group, which made it hard to draw clinical conclusions," Lord said. "A larger study would provide us with more clinical information as well as the performance of the x-ray fluorescence system. Decreasing the detection limit of our system is a future improvement to allow for individual assessment of gadolinium retention in bone."
The researchers maintained that there are currently no methods to measure gadolinium levels noninvasively in vivo. That capability alone sets this XRF device apart from other methods of measuring gadolinium in bone, according to the group.
"The current x-ray fluorescence system is capable of detecting gadolinium in small populations and in certain individuals only," Lord said. "The current device would be useful for studying gadolinium bone levels of particular groups that receive more GBCA-enhanced MRI scans, such as multiple sclerosis patients, and comparing to gadolinium levels in a control group."
In addition, although the results are preliminary, many observers will no doubt ponder the potential ramifications of this study in the debate over GBCAs.
"Our laboratory is not in a clinical setting in which GBCAs are administered and has not changed any protocol with respect to patients receiving GBCA," Lord said. "However, with all the recent literature published on gadolinium retention in the body, we hope to see a change in protocol with respect to patients receiving GBCA in the near future in all clinical settings."











![Overview of the study design. (A) The fully automated deep learning framework was developed to estimate body composition (BC) (defined as subcutaneous adipose tissue [SAT] in liters; visceral adipose tissue [VAT] in liters; skeletal muscle [SM] in liters; SM fat fraction [SMFF] as a percentage; and intramuscular adipose tissue [IMAT] in deciliters) from MRI. The fully automated framework comprised one model (model 1) to quantify different BC measures (SAT, VAT, SM, SMFF, and IMAT) as three-dimensional (3D) measures from whole-body MRI scans. The second model (model 2) was trained to identify standardized anatomic landmarks along the craniocaudal body axis (z coordinate field), which allowed for subdividing the whole-body measures into different subregions typically examined on clinical routine MRI scans (chest, abdomen, and pelvis). (B) BC was quantified from whole-body MRI in over 66,000 individuals from two large population-based cohort studies, the UK Biobank (UKB) (36,317 individuals) and the German National Cohort (NAKO) (30,291 individuals). Bar graphs show age distribution by sex and cohort. BMI = body mass index. (C) After the performance assessment of the fully automated framework, the change in BC measures, distributions, and profiles across age decades were investigated. Age-, sex-, and height-adjusted body composition reference curves were calculated and made publicly available in a web-based z-score calculator (https://circ-ml.github.io).](https://img.auntminnieeurope.com/mindful/smg/workspaces/default/uploads/2026/05/body-comp.XgAjTfPj1W.jpg?auto=format%2Ccompress&fit=crop&h=112&q=70&w=112)




