The council of the Union Européenne des Médecins Spécialistes (UEMS, the European Union of Medical Specialists) has endorsed -- with only a slight amendment -- best practice guidance published last year by the European Society of Radiology (ESR) and the European Federation of Societies for Ultrasound in Medicine and Biology (EFSUMB).
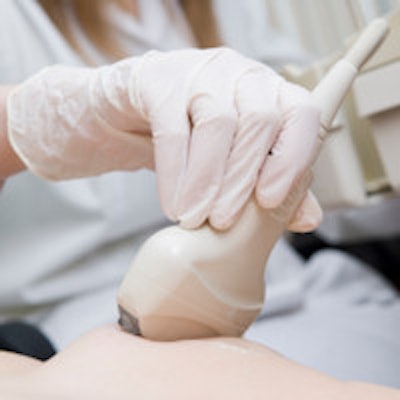
The guidance specifies that the availability of reports and images of all ultrasound examinations is important in clinical practice as a record of patient status at the time of the studies and as a point of references for future studies. ESR and EFSUMB consider it good clinical practice to provide accurate and retrievable recordings of all ultrasound examinations. They also recommend that all doctors using ultrasound should -- wherever possible -- organize workflow in ultrasound so that proper archiving of both images and reports of all studies can be regularly achieved.
 UEMS logo.
UEMS logo.
The UEMS council voted on 17 October in Granada, Spain, to add "where possible" to the statement that all ultrasound images should be stored and accurately reported. The guidelines had already been approved by the UEMS radiology section in March this year. The amendment was introduced prior to approval as discussions highlighted the lack of image storage capacities for hand held ultrasound machines.
The joint ESR-EFSUMB recommendation on archiving and reporting ultrasound examinations was published in the October 2013 edition of the open-access journal Insights into Imaging (Vol. 4:5, pp. 525-526), as well as in the April 2013 edition of the EFSUMB newsletter. This recommendation followed a survey by the ESR Working Group on Ultrasound, "Organization and practice of radiological ultrasound in Europe," which was published in the August edition of Insights into Imaging (Vol. 4:4, pp. 401-407).
The ESR Working Group's survey showed that most ultrasound images performed by radiologists are stored and a report is formulated, both of which are available for review at the time of the acute episode and for future reference. This is not always the case when other specialties are concerned, however. Problems reported are a lack of storage capacities for some handheld ultrasound devices and image storage facilities for smaller practices, where a link to a hospital PACS or other image archiving system is unavailable.
The published guidance is aimed at all doctors using ultrasound as "best clinical practice guidance," not just ESR and EFSUMB members. It presents some challenges, but it's important to overcome them to provide the best clinical care possible and ensure patient safety, enable quality control, and maintain standards. Another consideration is assisting doctors should they ever find themselves in a difficult medicolegal situation.


![Overview of the study design. (A) The fully automated deep learning framework was developed to estimate body composition (BC) (defined as subcutaneous adipose tissue [SAT] in liters; visceral adipose tissue [VAT] in liters; skeletal muscle [SM] in liters; SM fat fraction [SMFF] as a percentage; and intramuscular adipose tissue [IMAT] in deciliters) from MRI. The fully automated framework comprised one model (model 1) to quantify different BC measures (SAT, VAT, SM, SMFF, and IMAT) as three-dimensional (3D) measures from whole-body MRI scans. The second model (model 2) was trained to identify standardized anatomic landmarks along the craniocaudal body axis (z coordinate field), which allowed for subdividing the whole-body measures into different subregions typically examined on clinical routine MRI scans (chest, abdomen, and pelvis). (B) BC was quantified from whole-body MRI in over 66,000 individuals from two large population-based cohort studies, the UK Biobank (UKB) (36,317 individuals) and the German National Cohort (NAKO) (30,291 individuals). Bar graphs show age distribution by sex and cohort. BMI = body mass index. (C) After the performance assessment of the fully automated framework, the change in BC measures, distributions, and profiles across age decades were investigated. Age-, sex-, and height-adjusted body composition reference curves were calculated and made publicly available in a web-based z-score calculator (https://circ-ml.github.io).](https://img.auntminnieeurope.com/mindful/smg/workspaces/default/uploads/2026/05/body-comp.XgAjTfPj1W.jpg?auto=format%2Ccompress&fit=crop&h=100&q=70&w=100)






![Overview of the study design. (A) The fully automated deep learning framework was developed to estimate body composition (BC) (defined as subcutaneous adipose tissue [SAT] in liters; visceral adipose tissue [VAT] in liters; skeletal muscle [SM] in liters; SM fat fraction [SMFF] as a percentage; and intramuscular adipose tissue [IMAT] in deciliters) from MRI. The fully automated framework comprised one model (model 1) to quantify different BC measures (SAT, VAT, SM, SMFF, and IMAT) as three-dimensional (3D) measures from whole-body MRI scans. The second model (model 2) was trained to identify standardized anatomic landmarks along the craniocaudal body axis (z coordinate field), which allowed for subdividing the whole-body measures into different subregions typically examined on clinical routine MRI scans (chest, abdomen, and pelvis). (B) BC was quantified from whole-body MRI in over 66,000 individuals from two large population-based cohort studies, the UK Biobank (UKB) (36,317 individuals) and the German National Cohort (NAKO) (30,291 individuals). Bar graphs show age distribution by sex and cohort. BMI = body mass index. (C) After the performance assessment of the fully automated framework, the change in BC measures, distributions, and profiles across age decades were investigated. Age-, sex-, and height-adjusted body composition reference curves were calculated and made publicly available in a web-based z-score calculator (https://circ-ml.github.io).](https://img.auntminnieeurope.com/mindful/smg/workspaces/default/uploads/2026/05/body-comp.XgAjTfPj1W.jpg?auto=format%2Ccompress&fit=crop&h=112&q=70&w=112)








