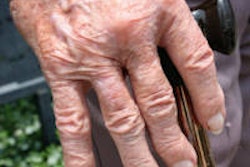
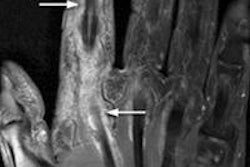
A new molecular imaging technique that can visualize inflammation in the joints was unveiled at this week's Society of Nuclear Medicine and Molecular Imaging (SNMMI) meeting taking place in St. Louis.
Dutch researchers used PET and SPECT, both of which image physiological processes, with the help of specialized detectors that pick up signals from injected radionuclide imaging agents.
In this case, the researchers evaluated antifibroblast activation protein (FAP) antibodies involved in the inflammation associated with rheumatoid arthritis. They used radiotracers that combine the molecular compound 28H1, which can bind to FAP in the body, with the radionuclides indium-111 (In-111), used in conjunction with SPECT imaging systems, and zirconium (Zr-89), used with PET systems.
The research is novel because radiolabeled anti-FAP antibodies have never been used before in molecular imaging for rheumatoid arthritis, according to lead author Peter Laverman, PhD, assistant professor of nuclear medicine from the department of radiology and nuclear medicine at Radboud University Medical Center in Nijmegen, the Netherlands.
The preclinical study used small animal scanners. Both In-111 28H1 and Zr-89 28H1 showed significantly increased imaging agent uptake in inflamed joints. The uptake was three to four times higher with these agents than another antibody agent evaluated as a control. The researchers also evaluated FDG to image inflammation, but uptake was not associated with the severity of inflammation. This experimental model proved 28H1 tagged with either In-111 or Zr-89 is a superior method for imaging arthritis.
"To the best of our knowledge, high-contrast images of this kind were unheard of until now," Laverman said. He estimated it may take two or more years to accumulate enough research to get the agents approved for arthritis imaging in mainstream clinical practice.











![Overview of the study design. (A) The fully automated deep learning framework was developed to estimate body composition (BC) (defined as subcutaneous adipose tissue [SAT] in liters; visceral adipose tissue [VAT] in liters; skeletal muscle [SM] in liters; SM fat fraction [SMFF] as a percentage; and intramuscular adipose tissue [IMAT] in deciliters) from MRI. The fully automated framework comprised one model (model 1) to quantify different BC measures (SAT, VAT, SM, SMFF, and IMAT) as three-dimensional (3D) measures from whole-body MRI scans. The second model (model 2) was trained to identify standardized anatomic landmarks along the craniocaudal body axis (z coordinate field), which allowed for subdividing the whole-body measures into different subregions typically examined on clinical routine MRI scans (chest, abdomen, and pelvis). (B) BC was quantified from whole-body MRI in over 66,000 individuals from two large population-based cohort studies, the UK Biobank (UKB) (36,317 individuals) and the German National Cohort (NAKO) (30,291 individuals). Bar graphs show age distribution by sex and cohort. BMI = body mass index. (C) After the performance assessment of the fully automated framework, the change in BC measures, distributions, and profiles across age decades were investigated. Age-, sex-, and height-adjusted body composition reference curves were calculated and made publicly available in a web-based z-score calculator (https://circ-ml.github.io).](https://img.auntminnieeurope.com/mindful/smg/workspaces/default/uploads/2026/05/body-comp.XgAjTfPj1W.jpg?auto=format%2Ccompress&fit=crop&h=112&q=70&w=112)




