Careful monitoring of colorectal cancer patients with PET/CT during initial treatment can predict outcomes, potentially improving success rates while reducing treatment costs, Italian researchers reported at this week's Society of Nuclear Medicine (SNM) meeting in Miami Beach, FL.
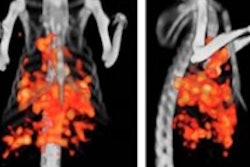
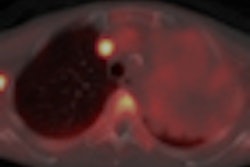
In 46 colorectal cancer patients with poor predicted outcomes, PET/CT exams acquired a couple of weeks after treatment positively correlated with surgical outcomes, according to the group.
The study examined the ability of F-18 FDG PET/CT to predict the effectiveness of combined radiation therapy, chemotherapy, and bevacizumab, a radiochemotherapy agent that suppresses angiogenesis.
Dr. Luigi Aloj and colleagues from Fondazione "G. Pascale" in Naples examined 46 patients with locally advanced rectal cancer and a poor prognosis. The patients were given three courses of chemotherapy during external radiation therapy, as well as bevacizumab for four days prior to the first two courses of chemotherapy.
In all, 37 participants responded positively to therapy -- a rate 15% higher than with previous treatment methods, the group said in a statement. Eight patients did not respond to treatment, and one refused surgery.
The PET/CT studies from the 12th day after treatment showed a positive correlation with outcomes confirmed at surgery. However, imaging studies acquired just before surgery were a poor indicator of how patients responded to treatment, Aloj and colleagues wrote.
The study offers more evidence that early and close monitoring with PET/CT during the first phase of a patient's course of treatment can increase the predictive value of response assessments, Aloj said. Further studies could utilize PET/CT not only to predict treatment response, but also to design more aggressive treatments for nonresponsive patients.










![Overview of the study design. (A) The fully automated deep learning framework was developed to estimate body composition (BC) (defined as subcutaneous adipose tissue [SAT] in liters; visceral adipose tissue [VAT] in liters; skeletal muscle [SM] in liters; SM fat fraction [SMFF] as a percentage; and intramuscular adipose tissue [IMAT] in deciliters) from MRI. The fully automated framework comprised one model (model 1) to quantify different BC measures (SAT, VAT, SM, SMFF, and IMAT) as three-dimensional (3D) measures from whole-body MRI scans. The second model (model 2) was trained to identify standardized anatomic landmarks along the craniocaudal body axis (z coordinate field), which allowed for subdividing the whole-body measures into different subregions typically examined on clinical routine MRI scans (chest, abdomen, and pelvis). (B) BC was quantified from whole-body MRI in over 66,000 individuals from two large population-based cohort studies, the UK Biobank (UKB) (36,317 individuals) and the German National Cohort (NAKO) (30,291 individuals). Bar graphs show age distribution by sex and cohort. BMI = body mass index. (C) After the performance assessment of the fully automated framework, the change in BC measures, distributions, and profiles across age decades were investigated. Age-, sex-, and height-adjusted body composition reference curves were calculated and made publicly available in a web-based z-score calculator (https://circ-ml.github.io).](https://img.auntminnieeurope.com/mindful/smg/workspaces/default/uploads/2026/05/body-comp.XgAjTfPj1W.jpg?auto=format%2Ccompress&fit=crop&h=112&q=70&w=112)





