In interventional radiology, radiation exposure is shaped by dozens of small decisions made in real time: how close the operator stands, how the C-arm is angled, whether shielding is used, and how tightly the beam is collimated.
But unlike other clinical risks, radiation offers no immediate feedback. There is no pain, no visible signal, no intuitive sense of escalation. Without that feedback loop, unsafe habits can persist unnoticed. That is where visibility, through dosimetry or simulation, turns radiation from an abstract concept into something operators can respond to in the moment.
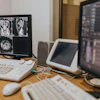
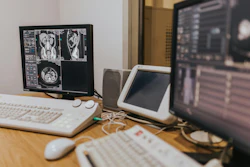
Move toward the C-arm and the dose rate climbs in real time. Step behind a ceiling-mounted shield and it drops. Change the pulse rate, the collimation, the projection angle, and the radiation field responds instantly. These dynamics were demonstrated by Silas Fuchs of Kiel, Germany, at ECR 2026 in Vienna, where he put on a VR headset in front of a live audience and showed radiation you can actually see.
Making the invisible visible
 "The main goal is always to make radiation visible and to make it interactive and intuitive to use," said Silas Fuchs, of Kiel, Germany, developer of the BfS virtual reality training tool. Courtesy of Claudia Tschabuschnig
"The main goal is always to make radiation visible and to make it interactive and intuitive to use," said Silas Fuchs, of Kiel, Germany, developer of the BfS virtual reality training tool. Courtesy of Claudia Tschabuschnig
Fuchs is a developer at Northdocks, the company that built the training tool in cooperation with Germany's Federal Office for Radiation Protection. The application runs on a standalone VR headset, with no external tracking hardware required, inside a virtual cath lab.
Users move freely through the space, interact with shielding, adjust equipment settings, and watch their real-time dose display respond to every decision. Equip the avatar with a thyroid shield and lead goggles and the numbers drop. Remove them, step closer to the source, skip the collimation, and they climb.
The simulation approximates radiation behavior rather than modeling every device-specific variable. Fuchs acknowledged that factors such as beam filtration differences between machine generations are not fully captured. The goal is not precise dosimetry.
Outside the congress halls, a multicenter crossover study across eight hospitals found that immersive VR training significantly and consistently reduced occupational radiation exposure among IR nurses, with effects that were immediate, statistically significant, and reproducible across two cohorts trained a year apart. A separate crossover study by Mwangi et al found that interventional cardiologists showed the largest reductions of any professional group, with an effect size of 4.37 in stratified analysis.
A free version of the BfS tool is available via the BfS platform, with a commercial version offering additional features. Fuchs noted that the shift to standalone headsets has been significant: earlier versions required a dedicated gaming PC and external trackers, creating real barriers to routine training use. That barrier is now largely gone.
However, a review of extended reality in radiology education found remaining challenges from economic barriers to difficulties integrating tools into existing curricula. The hardware problem is largely solved, the institutional problem is not.
What neuro-IR adds to the picture
The stakes are particularly high in neuro-interventional procedures, where dose dynamics differ from body IR in ways that are easy to underestimate. This comes at a time when a 2025 study in Neuroradiology on occupational radiation exposure among radiologic technologists in interventional neuroradiology found that eye lens dose is a specific and recurring concern, with radiation protection glasses playing a meaningful but variable role depending on procedure type and positioning.
 "We as seniors really have to guide our young staff to have this in mind, even though they need support in bearing in mind optimization and radiation protection," said Prof. Elke Ruth R. Gizewski, MD, of the Medical University of Innsbruck.Courtesy of Claudia Tschabuschnig
"We as seniors really have to guide our young staff to have this in mind, even though they need support in bearing in mind optimization and radiation protection," said Prof. Elke Ruth R. Gizewski, MD, of the Medical University of Innsbruck.Courtesy of Claudia Tschabuschnig
Prof. Elke Ruth R. Gizewski, MD, of the Medical University of Innsbruck in Austria, walked through the dose implications of mechanical thrombectomy in detail at ECR 2026. Staff scatter in neuro-IR is lower than in body procedures because the radiation field is smaller. But patient dose can be substantial, and the eye lens demands specific attention.
Tandem occlusion cases with carotid artery stenting were shown to have significantly higher dose-area product values than isolated MCA occlusions, while fluoroscopy time alone does not explain the difference. Each additional thrombectomy attempt compounds the exposure. Biplane imaging, used routinely for roadmapping and navigation, exposes both eyes to the lateral beam. Gizewski was direct: that requires active decision-making at each step, not a default setting. Do you need the second plane right now? If not, turn it off.
Meanwhile a real-time dosimetry study published in European Radiology confirmed that interventionalists' supporting hands receive the highest dose equivalents regardless of procedure type, a finding Gizewski connected directly to magnification. Each step up increases dose, sometimes substantially. Use what you need. Know what it costs.
At the same time a 2025 workload survey published in the European Physical Journal found significant interspecialty variations in tube current distributions across IR procedures, concluding that discipline-specific radiation protection protocols are needed rather than blanket guidance. Neuro-IR, with its small fields, high frame rates, and biplane setups, is exactly the kind of subspecialty where generic advice falls short.
She also pointed to a training effect visible in published data. Operators with higher procedure volumes consistently showed lower dose-area product values. "We as seniors really have to guide our young staff to have this in mind," Gizewski said at ECR 2026, "even though they need support in this time for bearing in mind optimization and radiation protection."
A simulator training research published in Scientific Reports has shown that repeated hands-on practice substantially decreases the time needed to perform simulated vascular interventions, a proxy for procedural proficiency, which is associated with lower radiation exposure in clinical practice. The evidence base is growing. The question is whether the field will build training around it.