As AI gains ground in all subspecialties, this is no less true in emergency, but how reliable is the tool for life-or-death situations?
In a dedicated “ESR Meets France” session at ECR 2026 in March, French experts met and discussed the latest thinking on AI, based on their own emergency departments’ real-life use, in the aptly named “Problem-solving with AI in emergencies: The French experience."
Providing an overview on AI tools in thoracic emergency, Prof. Mathieu Lederlin, head of the thoracic and cardiovascular imaging department in Pontchaillou University Hospital in Rennes and former JFR president (2025), noted that such tools improve detection sensitivity and can be used as a safety net and/or triage tool for some specific conditions. However, impact on interpretation time is more uncertain and there was as yet no evidence of improved survival with AI.
“In the future we will need large-scale prospective trials with hard end-points such as mortality to determine impact on the healthcare system,” he said.
He pointed to how, in the here-and-now, deploying AI to aid detection of pulmonary embolism (PE) could potentially save lives, particularly in cases where it could support less-experienced radiologists.
Clot detection
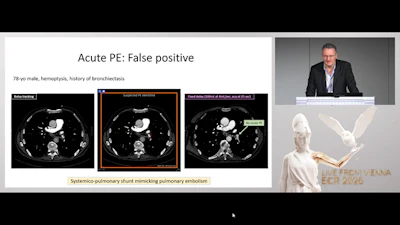
“Pulmonary embolism is one of the most deadly and urgent thoracic emergencies, and AI has good sensitivity and specificity for the automatic detection of clots," Lederlin said. "Performance is approximately the same as that of a radiologist, while some papers have shown that AI can detect acute PE missed by some radiologists so it could serve as a safety net and also as a tool for triage and prioritization. However, the negative predictive value is not 100% and its impact on reading and reporting time is uncertain."
Specifically, he noted that while AI can perform time-consuming tasks like the calculation of clot burden, the software had limitations: performance depended on the quality of the injection. Furthermore, there could be false-negative results in isolated subsegmental or chronic pulmonary embolism, or false positives due to artifacts, lymph nodes, or pulmonary veins.
As a case in point, he described how in a 41 year-old patient suffering from chest pain for three days, AI deemed there was no pulmonary embolism, but missed the occlusion of the coronary artery.
For diagnosing pneumothorax on x-ray, commercially available AI tools showed 100% sensitivity with a detection gain of up to 22% compared to radiology residents, and up to 30% with non-radiology residents, according to the literature. However, in terms of triage, human management was paramount due to the substantial rate of false positives, he added.
Lederlin also nodded to AI’s potential to recognize acute aortic syndrome on non-contrast CT, via studies that have shown that AI performs this task better than radiologists. Evidence from a recent Chinese study showed excellent negative predictive values, suggesting it could be used to rule out dissection in low-risk patients, without the use of contrast.
Eyeing other recent studies, Lederlin pointed to how AI, when applied to aortic CT angiography, can recognize dissection and classify type A and type B dissections quickly. Its main use could be triage and prioritization particularly in teleradiology.
However, there were pitfalls:
“Pay attention to false negatives. While AI can recognize dissection, it cannot recognize all the types of aortic syndrome such as intramural hematoma or penetrating ulcers,” he noted. “There are also false positives: If the CT scan is not ECG-gated, the software can wrongly recognize a dissection. So in acute aortic syndrome careful technique and accurate CT protocol is, for the moment, more important than AI,” he said.
Human expertise remains essential, whether upstream to analyze request relevance, choose the protocol, and adapt in real time, or downstream to interpret the results in the clinical context, manage false positives, and propose differential diagnoses, Lederlin continued.
“It is important to keep a clinical and critical eye on AI,” he noted.
Chatbot assistance
Speaking about AI’s integration in abdominal emergency, Prof. Ingrid Millet from Lapeyronie University Hospital in Montpellier, looked at how AI tools might help radiologists speed up workflow. She showcased an imagined AI chatbot, “Abdoguard”, which while currently a work of fiction, might point the way for AI developers.
And how might it work? “Abdoguard” would analyze the clinical and biological data contained in an emergency CT request and propose "red flag diagnoses." For example, if the pelvo-abdominal CT request was for a 45-year old man with no specific history and in pain since the previous day with vomiting, epigastric guarding, and with a CRP of 20, WBC at 13,500 but all other lab tests normal, the chatbot would suggest different hypotheses such as acute pancreatitis, perforated ulcer, acute cholecystitis, mesenteric ischemia, or myocardial infarction.
The chatbot would also propose a protocol, expedite it to the technician after human approval, and would analyze the images produced, flagging the abnormal exam and its suspicious features, as well as quantifying other findings such as free gas and fluid. Next, the chatbot would produce a preliminary report with proposed management, which the radiologist could choose to select -- or not.
 Prof. Ingrid MilletECR 2026
Prof. Ingrid MilletECR 2026
Returning to current reality and echoing Lederlin, she noted how beyond image interpretation AI could be used for workflow optimization, notably in worklist triage with flagging (free gas, blood, high-grade obstruction), and for structured reporting assistance through auto-extracting key findings and quantitative parameters, suggesting impression templates, and helping to find relevant reports.
“Some tools are available on the market, but these need to be assessed in departments, in daily practice,” Millet noted. “The future abdominal emergency radiologist will remain the expert enhanced by AI that is able to integrate decisions, supervise AI results, and orchestrate workflow. This is where the real impact could happen -- for now the objective is to reduce time to diagnosis.”
Chairing the session, Prof. Minerva Becker pointed to how France has always been at the forefront of imaging progress, leading the way in clinical innovation and academic research. This session was an expression of the enduring partnership between ESR and the France’s national society (SFR), at a time when European countries now more than ever needed to collaborate to meet shared challenges.
Her co-chair, Prof. Marie-France Bellin, noted that AI has had a transformational role in emergency, and would provide the cornerstone of acute patient care at a time when patient volumes and increasingly complex pathologies challenge rapid diagnosis.