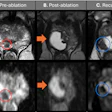
A doctor in Florida guides a stroke procedure. The patient lies in France. So does the robot that follows the doctors instructions.
What sounds like the future has already arrived. Inside interventional radiology, the technologies gaining ground are not the most advanced, but the most usable ones. A session at ECR 2026 laid out exactly which ones are landing and which ones are still waiting for a runway.
Robotics: Uneven, but moving
 "The robot should be used as a tool -- it cannot substitute clinical judgment," said Stavros C. Spiliopoulos, MD, PhD.Courtesy of Claudia Tschabuschnig
"The robot should be used as a tool -- it cannot substitute clinical judgment," said Stavros C. Spiliopoulos, MD, PhD.Courtesy of Claudia Tschabuschnig
Stavros C. Spiliopoulos, MD, PhD, of Attikon University Hospital in Athens, Greece, limited his scope to systems physically involved in the procedure: ones with an arm, not navigation software.
For CT-guided biopsy and ablation, the case is largely made. Several systems are commercially available in Europe: Micromate by Interventional Systems, Maxio by Perfint Healthcare, CAS-One IR by Cascination, and Epione by Quantum Surgical.
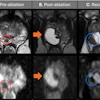
CAS-One IR adds post-ablation confirmation with 3D multi-trajectory planning across up to 20 needle paths, margin estimation, and recurrence risk scoring. Most larger systems require general anesthesia -- a practical and cost barrier that shapes adoption more than most technical specifications do.
Micromate, Spiliopoulos' own department's choice at Attikon, works with sedation alone and has shown reduced case duration, lower radiation exposure, and submillimeter needle accuracy, he said. One study with Epione reported nearly 71% of cases required no trajectory adjustment, no adverse events, and 86% local tumor control at six months.
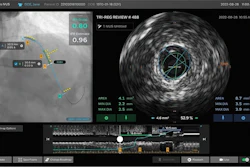
On the vascular side, Sentante, developed by a Lithuanian company, has completed first-in-human neurovascular procedures, works with standard catheters and guidewires, and offers haptic feedback -- something few current systems can claim. It performed that transatlantic stroke case. Liberty by Microbot Medical is in limited U.S. market release, with CE marking expected by late 2027.
Cost, training requirements, and logistical complexity still slow the transition from demonstration to routine practice. Spiliopoulos raised the critical question at the end of the panel.
"We are being pushed by technology to ask where it fits," he said. "The question is what are we trying to improve -- where do we need it, not where do we fit it."
AI: The workflow gains
 "Software-based assessment of ablation margins after treatment is becoming mandatory," said Irene Bargellini, MD, PhD. Courtesy of Claudia Tschabuschnig
"Software-based assessment of ablation margins after treatment is becoming mandatory," said Irene Bargellini, MD, PhD. Courtesy of Claudia Tschabuschnig
Irene Bargellini, MD, PhD, of the Candiolo Cancer Institute in Candiolo, Italy, made the case that AI in IR is not one thing. It is appearing before, during, and after procedures, and the applications already in use are rarely the ones generating conference excitement.
Large language models integrated into electronic medical records can compress a patient's full clinical history into a usable brief before the case begins -- saving an estimated 10 to 15 minutes per patient. Stroke triage software already detects occlusions and sends automated alerts to the full multidisciplinary team. Commercial vendors now offer tools handling semiautomatic lesion segmentation, virtual ablation zone estimation, and automated needle-tip tracking during procedures.
The strongest clinical claim from Bargellini: software-based ablation margin assessment is moving toward becoming standard practice. A randomized phase II trial from MD Anderson Cancer Center in the U.S. demonstrated that automated margin assessment after treatment improves outcomes, consistent with the COVER-ALL trial, which showed that AI-based confirmation software significantly increased minimal ablative margins compared with standard assessment.
Radiomics-based patient selection tells a different story. More than 130 publications on radiomics and chemoembolization in three years, and routine clinical application remains out of reach. Most studies stop at validation without demonstrating real-world impact on decisions or outcomes.
HIFU: Feasibility, not routine
David Maintz, MD, PhD, of University Hospital of Münster in Germany, presented MR-guided HIFU for two indications outside current approvals: pancreatic cancer and facet joint syndrome.
Pancreatic cancer carries a five-year survival rate of 11% in Germany and is the sixth leading cause of cancer death globally. Maintz's feasibility study has enrolled eight patients, all of whom met the primary endpoint -- confirmed non-perfused volume in the treated area.
All were discharged the following day, with no severe adverse events. Three patients have since died; their average survival was 15 months. For facet joint syndrome, six of a planned 10 patients have been treated, with rapid pain relief and quality of life improvement sustained at 90 days.
No comparative data against radiotherapy exist for either indication. This is feasibility work: it shows MR-guided HIFU in the pancreas is possible and safe in early experience, not that it outperforms existing options.
The session ran two registers in parallel. The loud one -- remote stroke robots, pancreatic HIFU, haptic catheters -- is real, and early. The quiet one -- margin confirmation, record summarization, automated triage -- is already in rooms, already saving time, already changing outcomes.
Bargellini's practical answer to what to deploy now was not robotics. It was the software doing its job in the background.
Full coverage of ECR 2026 is available here.