Patients with knee osteoarthritis who underwent either genicular artery embolization (GAE) or a sham procedure experienced equal pain reduction after a year, according to a recent study.
The finding is from a comparison among 58 participants with mild to moderate knee osteoarthritis who were unresponsive to conservative treatment, and further found no MRI differences between the groups in synovitis reduction, noted lead author Tijmen van Zadelhoff, MD, of Erasmus MC in Rotterdam, the Netherlands, and colleagues.
“Our results suggest that the pain reduction observed in patients treated with GAE is mainly due to a placebo effect, and that this placebo effect is sustained after 12 months,” the group wrote. The study was published April 20 in European Radiology.
Knee osteoarthritis (KOA) is the most prevalent degenerative joint disorder, resulting in pain, reduced mobility, and diminished quality of life. Conventional treatment options have limitations, including incomplete pain relief and risks associated with surgery, the authors noted.
Alternatively, GAE is a minimally invasive treatment that blocks small vessels that supply blood to the synovium, which is a key contributor to KOA pain. Early uncontrolled studies have shown promising improvements in pain and synovitis, yet overall, evidence remains inconclusive, according to the group.
In this study, the researchers hypothesized that if there was a true and lasting effect of GAE, the pain reduction in the GAE group would be sustained on longer-term follow-up, while the pain in the sham group would relapse. They recruited 58 patients with knee osteoarthritis who had experienced knee pain for at least six months and had not responded to at least six months of conservative treatment.
Participants received either GAE (n = 29) or a sham procedure (n = 29) in which a groin incision was made and all procedural steps were mimicked without actual embolization. Follow-up visits were conducted at one, four, eight, and 12 months. Pain was assessed using the Knee Injury and Osteoarthritis Outcome Score (KOOS) [range, zero to 100], and synovitis was evaluated with contrast-enhanced MRI at baseline, one month, and four months.
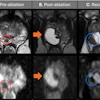
 Contrast-enhanced T1 weSPGR images of the knee of a patient from the GAE group at the level of the suprapatellar recess. The baseline image (left) shows a marked synovial enhancement. There was no change one month after treatment (middle image) and four months after treatment (right image).European Radiology
Contrast-enhanced T1 weSPGR images of the knee of a patient from the GAE group at the level of the suprapatellar recess. The baseline image (left) shows a marked synovial enhancement. There was no change one month after treatment (middle image) and four months after treatment (right image).European Radiology
“These results suggest a sustained placebo effect in the long term and do not support the clinical implementation of GAE as a treatment for KOA patients,” the group wrote.
The authors noted that the placebo effect is well-documented in knee osteoarthritis pain relief, and that research suggests that more invasive procedures tend to elicit stronger placebo responses. Thus, the relatively invasive nature of GAE may help explain the magnitude of improvement seen in the sham group, they suggested.
“Larger, sham-controlled trials with similar methodology are required to establish with greater certainty that there is no difference between GAE and a sham procedure in terms of clinical benefit,” the group concluded.
The full study is available here.