"Two aprons do not halve your dose. They just wreck your back."
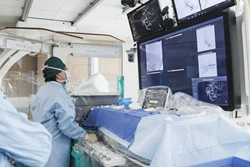
 "The most important target group for radiation protection in the IR environment is the operator, the healthcare worker who is there all the time," said Peter Reimer, MD, of the Städtisches Klinikum Karlsruhe. Courtesy of Claudia Tschabuschnig
"The most important target group for radiation protection in the IR environment is the operator, the healthcare worker who is there all the time," said Peter Reimer, MD, of the Städtisches Klinikum Karlsruhe. Courtesy of Claudia Tschabuschnig
With that line, Peter Reimer, MD, of the Städtisches Klinikum Karlsruhe in Germany, opened an ECR 2026 session arguing that interventional radiology (IR) still treats radiation safety too much like annual compliance training and not enough like a clinical skill. The patient, he continued, is not the primary target for radiation protection in the IR suite. The healthcare worker is. Staff are there every day. Dose accumulates across a career. And the training model has not kept pace.
First major update in 16 years
CIRSE and SIR released updated joint guidelines on radiation protection in February 2026, the first revision since 2010. The document covers new ground in several directions. Whereas the previous guidelines addressed only fluoroscopically guided interventions, the updated version now covers CT-guided procedures and radioembolization, and includes a new section on musculoskeletal risks.
That addition reflects a shift that has been building in the IR literature: the hazards of working in a high-dose environment are not only radiological. The guideline states that garments exceeding 0.5-mm lead-equivalent thickness offer no meaningful added fetal protection, while increasing physical strain on the pregnant staff member.
The same logic extends across the whole workforce. Heavier shielding adds musculoskeletal risk without adding protection. Reimer also noted a positive clarification the old guidelines lacked: pregnant staff can continue working in the IR suite provided standard protection measures are in place. Overprotection, he said, does not improve safety. It creates a different kind of harm.
The document was developed by a 12-member international panel led by Don Miller and is open access on both the CIRSE and SIR websites.
What the annual lecture cannot do
The cultural argument came up in the panel discussion that followed. Reimer described his own experience with real-time dosimetry: discovering mid-procedure that parameters had been carried over from the previous patient, with a completely different intervention profile.
"Before I start working, I check the parameters," he said at ECR 2026. "They always tell me we are ready to go. But the lead shield is somewhere, the under-table thing is somewhere, and the parameters are from the previous patient."
One attendee described a lung biopsy case at her institution where the performing radiologist was receiving five times the necessary dose, simply because she was standing on the wrong side of the C-arm. No one had told or shown her.
Another panelist noted that radiographers routinely wore lead aprons with the back clasp open because the aprons felt lighter, and no one had flagged it until real-time monitoring made the dose consequence visible.
"It was much easier to initiate this cultural change," the panelist told the room.
The panel also surfaced a finding that applies beyond fluoroscopy: under-table lead shields, standard in IR suites, are almost never deployed in CT-guided procedures, despite being easily fixed to the CT table rail and shown in studies to significantly reduce operator dose. It is not a hardware problem. Nobody does it because nobody taught them to, a change the panel argued makes unsafe practice easier to correct once the dose becomes visible.
What departments need to do now
The new CIRSE/SIR guideline calls for a practical, team-based approach covering all healthcare workers in the interventional suite, including radiographers, nurses, and physicians, with radiation safety aligned to modern, evidence-based workplace standards.
Yet, in practice, the shift Reimer described would mean more than updating a policy document. It would require departments to treat radiation protection as part of procedural training: optimizing room setup before each case, enforcing shield placement, reviewing dose data in real time, and involving the entire team, not just the operator, in how dose is managed. Real-time dosimetry, the panel agreed, makes that possible. It turns an invisible problem into a visible one.
The evidence base for continuous, hands-on training is growing. Whether IR departments will act on it, or schedule another annual lecture, remains the open question.