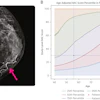
Every step in the radiomics workflow introduces nonbiological variance: scanner hardware, acquisition parameters, reconstruction algorithms, and even room temperature in MRI. None of it is biology. All of it affects results. Dr. Michelle Claire Williams, PhD, of the University of Edinburgh in Scotland, opened a session at ECR 2026 with exactly that problem.
The harmonization problem
The clinical consequence is blunt. A model trained at one site fails at another. Not because the biology changed, but because the scanner did.
 "Up to 7% of patients are reclassified into a different risk category, depending on the vendor," states Dr. Merel Huisman.All photos courtesy of Claudia Tschabuschnig
"Up to 7% of patients are reclassified into a different risk category, depending on the vendor," states Dr. Merel Huisman.All photos courtesy of Claudia Tschabuschnig
Two strategies exist. The first choice is protocol standardization. Align acquisition and reconstruction parameters prospectively, using frameworks from QIBA, EIBALL, and ACR accreditation. This is the cleanest solution, but it is also the hardest to implement retrospectively.
When that window closes -- and in real-world multicenter research it often does -- statistical harmonization steps in. These methods include ComBat and its growing family of variants: ComBat-GAM, GMM-ComBat, and NeuroHarmony. They address batch effects across linear and nonlinear covariates, longitudinal measurements, and covariance structures.
 "There are actually two ways to improve model generalisability. The first is to make the model insensitive to the site effect. The second is to remove that site effect using harmonization," says Irène Buvat.
"There are actually two ways to improve model generalisability. The first is to make the model insensitive to the site effect. The second is to remove that site effect using harmonization," says Irène Buvat.
There is one practical limit: A few dozen samples per site are typically needed to estimate feature distributions reliably. Below that threshold, the statistics don't hold. How acquisition standardization and postprocessing correction interact, and where each breaks down, was covered by Irène Buvat, PhD, from the Institut Curie in Orsay, France.
Deep learning enters the stack
Three families of deep-learning methods exist for sites where statistical correction isn't enough. Stanford University's Akshay Chaudhari, PhD, walked through all of them.
Cycle-GAN methods transform images between scanner distributions. For example, MR scans from GE HealthCare versus Siemens Healthineers equipment are transformed to make them appear as though they came from the same source, scalable to two distributions, not to five or ten. Diffusion-based generative models work on the same premise and have the same ceiling.
Variational autoencoders take a different route. Instead of transforming images to look like another scanner's output, they learn a compressed, lower-dimensional feature space inherently less sensitive to site effects. No labels required.
An open-source medical variational autoencoder developed by Chaudhari's group compresses 3D MR images by a large factor while preserving reconstruction quality. Models trained on those features showed equivalent accuracy with less noise than naive downsampling. That matters at scale.
Foundation models are the third approach. One model, trained on 20,000 abdominal CT scans alongside paired radiology reports and diagnostic codes, was tested across four external sites, including one where the scanner distribution had zero overlap with the training data -- the site used Canon scanners only, but Canon was not featured in the training set. Performance held across common and rare abdominal findings. Multimodal training builds robustness that single-site training cannot replicate.
A practical consensus emerged from the panel. Don't reach for deep learning if logistic regression will do. Match the method to the problem. ComBat for some applications. Foundation models for others. Knowing the clinical endpoint first determines which approach is appropriate. That part is still undereducated in the field.
From harmonized data to shared infrastructure
What comes next once the data is clean was the territory of the AI-SC 14, "AI in the context of the European Health Data Space," chaired by Prof. Luis Martí-Bonmatí of La Fe University and Polytechnic Hospital in Valencia, Spain, and Dr. Adrian Brady of University College Cork in Cork, Ireland.
Three things change under the European Health Data Space (EHDS), as Carla Meeuwis, MD, PhD, of Radioloog Rijnstate in Arnhem, Netherlands, laid out. Patients gain control over their own imaging data. Healthcare professionals lose administrative duplication. Researchers gain lawful, structured access to pseudonymised data across borders.
 "Patients will gain more control over the health data that healthcare providers record about them," according to Dr. Carla Meeuwis.
"Patients will gain more control over the health data that healthcare providers record about them," according to Dr. Carla Meeuwis.
The regulation entered into force in 2025, with implementation rolling out progressively into the early 2030s. Patient summaries and ePrescriptions are targeted for cross-border exchange around 2029. Medical images and imaging reports follow in the next phase.
The implications for radiology are direct. Patients will read their own reports. They gain the right to add information, clearly marked as patient-contributed, not clinician-authored. Imaging data stays at the originating institution. Researchers come to the data, not the other way around. Secure Processing Environments handle the rest.
Behind the European Electronic Health Record Exchange Format sits Xt-EHR, 27 European Union (EU) member states plus Norway, and dozens of organizations, building the harmonized use cases and information models that will make cross-border imaging exchange real.
Specifications are due by March 2027, presented by Esther Peelen of Nictiz in the Hague, Netherlands. Coverage includes patient summaries, ePrescriptions, imaging, laboratory results, discharge reports, and telemedicine. Testing frameworks are already in development.
Underneath all of it sits the technical plumbing, walked through by Dr. Marc Kämmerer, from Bochum, Germany. This is how imaging studies are embedded within the Integrating the Healthcare Enterprise (IHE) standard, how DICOM and HL7 FHIR interact, how the IHE Integrated Reporting Applications hub connects AI tools, image viewers, and report recording systems. The infrastructure is real. The standards are converging. The timeline is fixed.
The diversity imperative
Connecting both sessions was an argument from Prof. Martí-Bonmatí. Cancer Imaging Europe (EUCAIM), the EU-funded pan-European cancer imaging infrastructure, is not just a repository. It is a compliance-by-design model for large-scale research data governance.
Tiered participation: catalogue access, federated query, distributed processing. Institutions at different levels of technical and governance maturity can participate without exclusion. Layered, risk-based anonymization is designed to overcome what speakers called the "anonymization wall," the point where privacy requirements produce datasets so depleted they are no longer scientifically useful.
Eight research projects currently access the EUCAIM infrastructure, covering lung nodule characterization, pancreatic lesion detection, breast microcalcification classification, glioma MRI datasets, and prostate cancer radiomics. Institutions across Spain, Italy, Poland, the Netherlands, and Greece are participating.
That data diversity, the kind that makes discovery possible, depends entirely on harmonization. The two sessions were not running in parallel by coincidence.
The goal is stated. The regulatory framework is in place. The infrastructure is being built. What remains is execution, and the clinical education to make clear that harmonization is not a statistical formality. It is what makes the data mean what it says.