A simple additional x-ray can help determine whether penetrating objects have breached cortical bone, according to a team in Canada.
Researchers at the University of Saskatchewan described and tested a technique they named the "high noon" view in 21 patients, the majority of whom had sustained nail-gun injuries. The extra projection was easy to acquire and improved both accuracy and radiologist confidence over standard views alone, noted lead author Myles Mabee, MD, and colleagues.
“The addition of the ‘high noon’ view improved diagnostic accuracy for assessing cortical involvement, statistically improved diagnostic confidence by participating radiologists, and, in most cases, was deemed subjectively helpful,” the group wrote. The study was published March 30 in the Journal of Medical Imaging and Radiation Sciences.
Determining whether a penetrating foreign body has reached cortical bone is a clinically important question in emergency settings, as osseous involvement influences antibiotic prescribing, surgical planning, and infection risk, the authors explained. The standard protocol in these cases calls for two orthogonal radiographic views, but these may not optimally visualize the bone–foreign body interface when overlapping structures obscure the relevant anatomy, they noted.
The researchers hypothesized that that there is diagnostic benefit in the addition of a radiologic view acquired along the long axis of the foreign body attempting to follow its exact track.
“We have named this the ‘high noon’ view, akin to the sun directly overhead, casting minimal shadows onto structures below,” the group wrote.
To test the method, the researchers launched a pilot project and enrolled 21 participants (19 men, two women; mean age 36 years old) presenting with a penetrating foreign body at four participating sites. Nail gun injuries to the hand and fingers were the most common presentation.
All patients received routine radiographic views plus the high noon view, which is acquired by rotating the x-ray tube so the central beam runs coaxial with the long axis of the foreign body. Technologists were permitted up to three attempts if the initial acquisition appeared suboptimal.
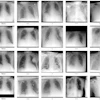
 Routine hand views (a) and ‘high noon’ view (b) of a 31-year-old male with penetrating nail gun injury (case 4). The lack of cortical bone involvement is much better visualized on the high noon view.Journal of Medical Imaging and Radiation Sciences
Routine hand views (a) and ‘high noon’ view (b) of a 31-year-old male with penetrating nail gun injury (case 4). The lack of cortical bone involvement is much better visualized on the high noon view.Journal of Medical Imaging and Radiation Sciences
According to the results, a single high noon acquisition was sufficient in 17 of 21 cases (81%), with a maximum of two attempts needed in the remaining four. Accuracy for correctly identifying the absence of cortical involvement improved from 71% to 100% for one reviewer and from 52% to 81% for the second. Likert confidence scores improved significantly for both reviewers (p < 0.001 and p = 0.033, respectively). The view was subjectively rated as helpful in 57% and 62% of cases by the two reviewers, and both endorsed its routine use going forward.
Technologists reported that the high noon view integrated smoothly into existing workflows without meaningful added time, required no additional equipment, and was described as straightforward and engaging to perform, according to the group.
“The intervention required no additional equipment, cost, or considerable workflow disruption, supporting real-world applicability,” the researchers wrote.
They called for larger multicenter studies incorporating cases with confirmed cortical breach to the establish the sensitivity of the view for detecting osseous involvement. Nonetheless, the authors noted the high noon view has already been adopted as standard protocol at their institution.
"Given its clinical utility, this is now part of our routine clinical care, and we recommend its use at other institutions as well," Mabee and colleagues concluded.
The full study is available here.