German researchers have shown that in high-risk breast cancer patients, MR mammography is a cost-effective alternative to mammography in a yearly screening setting. Their study analyzed the comparative cost-effectiveness of MR mammography (MRM) versus conventional imaging in a screening setting, with particular focus on the impact of its specificity.
"An interesting result from this study is that according to our analysis there are far less cost-effective imaging techniques than MR. A society that is willing to afford ultrasound as a screening tool should be far more willing to 'invest' in MRM," noted lead author Dr. Clemens Kaiser head of breast diagnostics at the University Hospital of Mannheim, in an article published online on 29 January in the European Journal of Radiology.
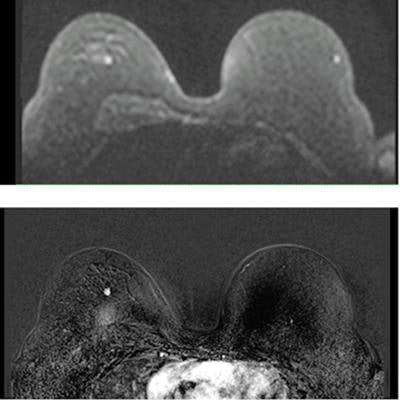
 Examples of MR mammography images, courtesy of the University Hospital of Mannheim.
Examples of MR mammography images, courtesy of the University Hospital of Mannheim.The results showed that MRM was cost-effective. Based on current recommendations for economic evaluations the team defined a willingness to pay threshold (WTP) of $100,000 per quality-adjusted life years (QALYs). Therefore, an incremental cost-effectiveness ratio (ICER) below this WTP was assumed to be an indicator of cost-effectiveness.
The study team used decision-analytic modeling and Markov models to evaluate cumulative costs of each screening modality and their subsequent treatments as well as cumulative outcomes in quality-adjusted life years.
In a base-case analysis, screening with mammography versus MRM and treatment resulted in overall costs of $36,201.57 versus $39,050.97 and a cumulative effectiveness of 19.53 QALYs versus 19.59 QALYs. This resulted in an ICER of $45,373.94 per QALY for MRM.
Ultrasound and mammography plus ultrasound resulted in ICER values higher than the WTP. In the sensitivity analyses, MR mammography remained a cost-effective strategy for screening high-risk patients as long as the specificity of the technique did not drop below 86.7%.
| Costs and economic impact of breast imaging strategies | ||||
| Strategy | Cumulative costs | Incremental costs | Cumulative effects (QALYs) | Incremental effects (QALYs) |
| Mammography | $36,201.57 | N/A | 19.53 | N/A |
| Ultrasound (US) | $36,667.66 | $466.10 | 19.53 | 0.001 |
| Mammo and US | $37,984.17 | $1,782.60 | 19.55 | 0.016 |
| MRM | $39,050.97 | $2,849.40 | 19.59 | 0.063 |
The probabilistic sensitivity analysis, which involved 30,000 iterations of varying input parameters, revealed on average higher costs but also higher effectiveness of the MR mammography strategy in high-risk patients. In a WTP-dependent analysis, a WTP of more than $30,400 per QALY indicated that MRM was cost-effective in the majority of iterations. A direct comparison of MRM and mammography showed the higher costs of MRM while being associated with a higher cumulative effectiveness in the vast majority of cases.
 Acceptability curve for several levels of WTP. With increasing WTP to more than $51,625 per QALY, MRM is the cost-effective option in the majority of iterations of probabilistic sensitivity analysis. Image courtesy of Dr. Clemens Kaiser et al. Originally published in the European Journal of Radiology.
Acceptability curve for several levels of WTP. With increasing WTP to more than $51,625 per QALY, MRM is the cost-effective option in the majority of iterations of probabilistic sensitivity analysis. Image courtesy of Dr. Clemens Kaiser et al. Originally published in the European Journal of Radiology.This research was conducted in order to complete a series of studies the team has published lately on the cost-effectiveness of MRM as a screening tool in various patient populations.
"Cost issues are one of the major concerns against using MRM in a broader set of indications, which is why we have been trying to fill the data gap. This paper indicates that MRM is diagnostically superior as well as cost-effective," Kaiser told AuntMinnieEurope.com. "There is seemingly no reason not to use MRM as a screening tool for patients with dense breasts."
MR mammography is affordable for any healthcare system in the western hemisphere based on a WTP of $100,000 per QALY, he added.
The initial higher imaging costs of MR are easily outweighed by long-term benefits of the detection of small cancers, with data suggesting that it therefore should be used as an imaging tool more frequently in extended indications, such as screening for breast cancer in dense breasts, he noted.
"MRM has an outstanding accuracy -- in contrast to any other x-ray-based imaging technique -- and this independently from breast density. However, because there is no data on screening women independently from breast density with MRM it is unclear as to whether it is cost-effective as a regular screening tool for all women," he said.
 Dr. Matthias Dietzel, MHBA.
Dr. Matthias Dietzel, MHBA.Co-author Dr. Matthias Dietzel, MHBA, a breast radiologist and professor of radiology at the Friedrich Alexander University, Erlangen, noted that cost analysis was extremely important when deciding on screening strategies.
"The oversimplified conversation that MR is more expensive compared to mammography and therefore should be abandoned as a financial burden too great is not true. If we invest in a better modality which detects cancer earlier and at a better stage in dense breasts, this will save money and most probably improve quality of life of the patients."






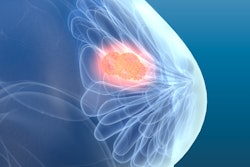






![Overview of the study design. (A) The fully automated deep learning framework was developed to estimate body composition (BC) (defined as subcutaneous adipose tissue [SAT] in liters; visceral adipose tissue [VAT] in liters; skeletal muscle [SM] in liters; SM fat fraction [SMFF] as a percentage; and intramuscular adipose tissue [IMAT] in deciliters) from MRI. The fully automated framework comprised one model (model 1) to quantify different BC measures (SAT, VAT, SM, SMFF, and IMAT) as three-dimensional (3D) measures from whole-body MRI scans. The second model (model 2) was trained to identify standardized anatomic landmarks along the craniocaudal body axis (z coordinate field), which allowed for subdividing the whole-body measures into different subregions typically examined on clinical routine MRI scans (chest, abdomen, and pelvis). (B) BC was quantified from whole-body MRI in over 66,000 individuals from two large population-based cohort studies, the UK Biobank (UKB) (36,317 individuals) and the German National Cohort (NAKO) (30,291 individuals). Bar graphs show age distribution by sex and cohort. BMI = body mass index. (C) After the performance assessment of the fully automated framework, the change in BC measures, distributions, and profiles across age decades were investigated. Age-, sex-, and height-adjusted body composition reference curves were calculated and made publicly available in a web-based z-score calculator (https://circ-ml.github.io).](https://img.auntminnieeurope.com/mindful/smg/workspaces/default/uploads/2026/05/body-comp.XgAjTfPj1W.jpg?auto=format%2Ccompress&fit=crop&h=112&q=70&w=112)




