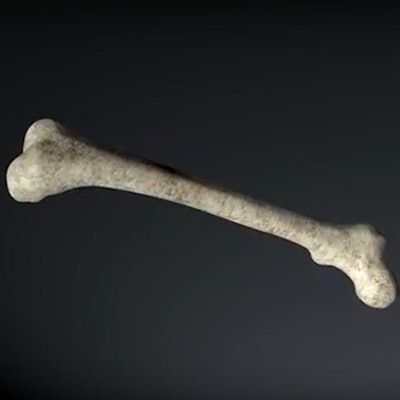
Researchers at Trinity College in Dublin have devised an experimental 3D bone scanning technique that may improve the diagnosis of bone injuries without the use of ionizing radiation, according to a new study published in Chemical Communications.
The technique begins with researchers attaching luminescent compounds to tiny gold structures to form nanoagents that are attracted to calcium-rich surfaces. These structures appear when bones form even the tiniest cracks, the authors noted in a statement.
The biologically safe nanoagents target and highlight the cracks formed in damaged bones, allowing researchers to produce a complete 3D image of the damaged regions (Chemical Communications, September 2016, Vol. 18-52:72, pp. 10,858-10,861).
Daily bone damage
Everyday activity stresses the bones and causes microcracks to develop, explained Dr. Clive Lee, professor of anatomy in the Royal College of Surgeons in Ireland (RCSI) and the Royal Hibernian Academy and visiting professor of biomechanics in Trinity College Dublin. Bones are normally repaired by a modeling process, but when the microcracks develop too fast they can grow faster than the remodeling process and ultimately weaken bones, he added. The process occurs in athletes and in the elderly, who develop especially extensive fractures when osteoporosis is present.
The current imaging standard, x-ray, can see the bone and major fractures but provides little information about bone structure and quality. By using the nanoagent to label microcracks and detecting them with MRI, the team hopes to study bone quality and quantity and deliver appropriate therapy, especially regarding the diagnoses of weak bones before they break.
The high resolution of the technique is a major advantage, along with the lack of radiation, the researchers said.
The project comes from many years of collaboration between Trinity chemists and engineering experts from the RCSI.
The technique results in a highly detailed 3D map of bone damage showing microcracks using noninvasive luminescence imaging, the authors wrote. With the nanoagent, bone damage can be demonstrated in a manner that wasn't possible previously, and the work represents a major step in the development of targeted contrast agents for use in clinical applications.
Science Foundation Ireland funded the project, which also benefited from collaboration with scientists at RCSI, led by Lee.











![Overview of the study design. (A) The fully automated deep learning framework was developed to estimate body composition (BC) (defined as subcutaneous adipose tissue [SAT] in liters; visceral adipose tissue [VAT] in liters; skeletal muscle [SM] in liters; SM fat fraction [SMFF] as a percentage; and intramuscular adipose tissue [IMAT] in deciliters) from MRI. The fully automated framework comprised one model (model 1) to quantify different BC measures (SAT, VAT, SM, SMFF, and IMAT) as three-dimensional (3D) measures from whole-body MRI scans. The second model (model 2) was trained to identify standardized anatomic landmarks along the craniocaudal body axis (z coordinate field), which allowed for subdividing the whole-body measures into different subregions typically examined on clinical routine MRI scans (chest, abdomen, and pelvis). (B) BC was quantified from whole-body MRI in over 66,000 individuals from two large population-based cohort studies, the UK Biobank (UKB) (36,317 individuals) and the German National Cohort (NAKO) (30,291 individuals). Bar graphs show age distribution by sex and cohort. BMI = body mass index. (C) After the performance assessment of the fully automated framework, the change in BC measures, distributions, and profiles across age decades were investigated. Age-, sex-, and height-adjusted body composition reference curves were calculated and made publicly available in a web-based z-score calculator (https://circ-ml.github.io).](https://img.auntminnieeurope.com/mindful/smg/workspaces/default/uploads/2026/05/body-comp.XgAjTfPj1W.jpg?auto=format%2Ccompress&fit=crop&h=112&q=70&w=112)





