Dear Cardiac Imaging Insider,
This issue features some important stories from the recent International Symposium on CT (ISCT), where presenters showed off CT's value in cardiac imaging that expanded on its traditional home base of coronary CT angiography (CCTA).
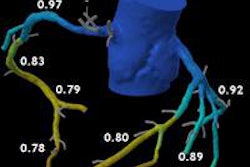
Among the presentations, Dr. Koen Nieman from Erasmus University Medical Center in the Netherlands looked beyond recent high-profile clinical trials of fractional flow-reserve CT (FFR-CT) to talk about how it works in daily clinical practice. Nieman covers the strengths of the technique as a replacement for myocardial perfusion imaging to assess the impact of coronary artery stenosis at CCTA. He also offers tips on what to watch out for to avoid introducing inaccuracies into the diagnosis. Get the scoop on FFR-CT here.
Of course, myocardial perfusion imaging (MPI), especially the CT variety, isn't going away, according to a talk by Dr. Thomas Henzler from the University of Mannheim in Germany. In fact, CT MPI is growing stronger as researchers learn simpler techniques for getting the functional information that CT MPI has to offer with less time and effort. Henzler credits Japanese researchers for one intriguing idea in a story you'll find here.
In another ISCT presentation, Dr. Hans-Christoph Becker looks at cardiomyopathy, another type of heart disease in which CT's value is often overlooked in favor of MRI. Becker looks at the different categories of cardiomyopathies, highlighting CT's particular strengths and weaknesses across the board. Learn what to look for in CT imaging of cardiomyopathy by clicking here.
Moving on from CT, a study presented at the Society of Nuclear Medicine and Molecular Imaging found that symptomatic patients need not have coronary calcium to be at high risk of myocardial infarction. To be sure, coronary artery calcification can be a key early sign of atherosclerosis that often precedes obstructive coronary artery disease by many years. But a lack of coronary artery calcium doesn't mean the patient won't go on to have an event, Dr. Samia Massalha and colleagues conclude.
We invite you to scroll through the links below for all the news in cardiac imaging, right here in your Cardiac Imaging Community.








![Overview of the study design. (A) The fully automated deep learning framework was developed to estimate body composition (BC) (defined as subcutaneous adipose tissue [SAT] in liters; visceral adipose tissue [VAT] in liters; skeletal muscle [SM] in liters; SM fat fraction [SMFF] as a percentage; and intramuscular adipose tissue [IMAT] in deciliters) from MRI. The fully automated framework comprised one model (model 1) to quantify different BC measures (SAT, VAT, SM, SMFF, and IMAT) as three-dimensional (3D) measures from whole-body MRI scans. The second model (model 2) was trained to identify standardized anatomic landmarks along the craniocaudal body axis (z coordinate field), which allowed for subdividing the whole-body measures into different subregions typically examined on clinical routine MRI scans (chest, abdomen, and pelvis). (B) BC was quantified from whole-body MRI in over 66,000 individuals from two large population-based cohort studies, the UK Biobank (UKB) (36,317 individuals) and the German National Cohort (NAKO) (30,291 individuals). Bar graphs show age distribution by sex and cohort. BMI = body mass index. (C) After the performance assessment of the fully automated framework, the change in BC measures, distributions, and profiles across age decades were investigated. Age-, sex-, and height-adjusted body composition reference curves were calculated and made publicly available in a web-based z-score calculator (https://circ-ml.github.io).](https://img.auntminnieeurope.com/mindful/smg/workspaces/default/uploads/2026/05/body-comp.XgAjTfPj1W.jpg?auto=format%2Ccompress&fit=crop&h=112&q=70&w=112)





