German researchers are reporting early success in performing PET/CT with a novel gallium-68-labeled (Ga-68) prostate-specific membrane antigen (PSMA) ligand to detect prostate cancer recurrence after radical prostatectomy.
The study's findings, published in the May issue of the Journal of Nuclear Medicine, could help with early detection of prostate cancer recurrence and lead to more appropriate and successful treatment of the disease.
Dr. Matthias Eiber, from Technische Universität München, and colleagues found that the hybrid PSMA ligand identified a large number of positive findings in the clinically important range of low PSA values (less than 0.5 ng/mL). They noted that the Ga-68-PSMA-ligand with PET/CT achieved higher detection rates than tracers such as choline or other imaging modalities such as MRI.
The study evaluated 248 patients with biochemical recurrence of prostate cancer (median PSA level, 1.99 ng/mL; range, 0.2-59.4 ng/mL) after radical prostatectomy. All were given contrast-enhanced PET/CT after injection of 155 ± 27 MBq Ga-68-PSMA-ligand.
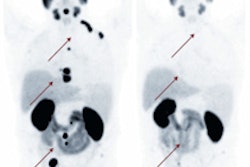
For 222 (89%) of the patients, the test detected higher than normal levels of PSMA. Whereas detection rates increased with higher PSA velocity, no significant association could be found for PSA doubling time (JNM, May 2015, Vol. 56:5, pp. 668-674).
In addition, the Ga-68-PSMA-ligand with PET (compared to CT) exclusively provided pathological findings in 81 (33%) patients. In 61 (25%) patients, it exclusively identified additional involved regions.
The findings will enhance the use of PET in the diagnostic workup of patients with recurrent prostate cancer, according to the researchers. They also speculated that the tracer may gain acceptance outside of Europe, pending regulatory clearance in other countries.







![Overview of the study design. (A) The fully automated deep learning framework was developed to estimate body composition (BC) (defined as subcutaneous adipose tissue [SAT] in liters; visceral adipose tissue [VAT] in liters; skeletal muscle [SM] in liters; SM fat fraction [SMFF] as a percentage; and intramuscular adipose tissue [IMAT] in deciliters) from MRI. The fully automated framework comprised one model (model 1) to quantify different BC measures (SAT, VAT, SM, SMFF, and IMAT) as three-dimensional (3D) measures from whole-body MRI scans. The second model (model 2) was trained to identify standardized anatomic landmarks along the craniocaudal body axis (z coordinate field), which allowed for subdividing the whole-body measures into different subregions typically examined on clinical routine MRI scans (chest, abdomen, and pelvis). (B) BC was quantified from whole-body MRI in over 66,000 individuals from two large population-based cohort studies, the UK Biobank (UKB) (36,317 individuals) and the German National Cohort (NAKO) (30,291 individuals). Bar graphs show age distribution by sex and cohort. BMI = body mass index. (C) After the performance assessment of the fully automated framework, the change in BC measures, distributions, and profiles across age decades were investigated. Age-, sex-, and height-adjusted body composition reference curves were calculated and made publicly available in a web-based z-score calculator (https://circ-ml.github.io).](https://img.auntminnieeurope.com/mindful/smg/workspaces/default/uploads/2026/05/body-comp.XgAjTfPj1W.jpg?auto=format%2Ccompress&fit=crop&h=112&q=70&w=112)






