German researchers have reported that contrast agent application can be omitted in juvenile idiopathic arthritis (JIA) patients when using an augmented knee MRI protocol comprising proton density (PD)-weighted sequences.
"Unenhanced MRI can detect disease activity of the knee joint in patients with JIA with equally high accuracy compared to contrast-enhanced MRI," noted Dr. Van Dai Vo Chieu, from the Institute for Diagnostic and Interventional Radiology at Hannover Medical School, and colleagues in an article posted on 6 December by European Radiology.
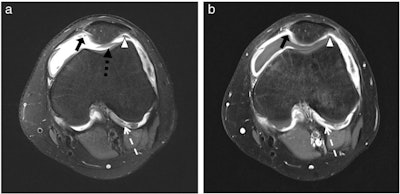 A 12-year-old girl with extended oligoarthritis. Axial images demonstrate joint effusion and synovial membrane thickening, notably at the junction of the lateral condyle and the cruciate ligament (white dotted arrow), medial (black arrow), lateral (white arrowhead), and dorsal (black dotted arrow) to the patella, notably visible on image. (A) Proton-density-weighted fat-saturated sequence. (B) Contrast-enhanced T1-weighted turbo spin echo fat-saturated sequence. Figure courtesy of Dr. Van Dai Vo Chieu et al and European Radiology.
A 12-year-old girl with extended oligoarthritis. Axial images demonstrate joint effusion and synovial membrane thickening, notably at the junction of the lateral condyle and the cruciate ligament (white dotted arrow), medial (black arrow), lateral (white arrowhead), and dorsal (black dotted arrow) to the patella, notably visible on image. (A) Proton-density-weighted fat-saturated sequence. (B) Contrast-enhanced T1-weighted turbo spin echo fat-saturated sequence. Figure courtesy of Dr. Van Dai Vo Chieu et al and European Radiology.JIA is a heterogeneous group of inflammatory musculoskeletal diseases comprising all forms of arthritis that begin before the age of 16, persist for more than six weeks, and are of unknown etiology and pathophysiology. The yearly incidence in developed countries is between two and 20 cases per 100,000 children, making it one of the most common chronic inflammatory diseases in kids, they explained.
Inflammation in the affected joints leads to synovial proliferation with consecutive secretion of synovial fluid and synovial hypertrophy, and this can lead to cartilage lesions and bone erosions, resulting in pain and disability.
Minimizing time to treatment after onset of synovial inflammation is reported to improve long-term outcomes, according to the authors. MRI and Doppler ultrasound are frequently used to detect inflammation within the joint before destruction occurs as well as for monitoring disease progression and treatment response.
Ultrasonography is commonly used to monitor joint effusion and synovial hypertrophy, but MRI is considered the most sensitive technique for evaluating joint inflammation, they added.
Study logistics
In the Hannover study, 53 knee joint MRI examinations were performed between January 2015 and January 2020 on a 3-tesla system in 27 patients (age, 11.4 ± 3.6 years; 21 girls, 6 boys). MRI protocols comprised PD-weighted sequences, in addition to the widely used standard protocol.
The JIA subgroups consisted of oligoarticular arthritis (n = 16), extended oligoarthritis (n = 6), rheumatoid factor-negative polyarticular arthritis (n = 3), enthesitis-related arthritis (n = 1), and psoriatic arthritis (n = 1).
The MRI scans were retrospectively analyzed by three experienced radiologists in two readings, using the juvenile arthritis MRI scoring (JAMRIS) system and a modified international prophylaxis study group (IPSG) classification. In the first reading session, only unenhanced MR images were evaluated. In a second reading session, all images before and after contrast medium application were included. To avoid bias, an interval of at least two weeks was set between the two readings.
"The intra- and inter-reader agreement was high for unenhanced and enhanced MRI JAMRIS scores, which indicate relatively good applicability of the scoring system, even for less experienced readers," the authors wrote.
The clinical juvenile arthritis disease activity score (JADAS10) was calculated (including clinical assessment and laboratory workup) and correlated with MRI scores.
When using the clinical JADAS10 as a reference standard for the detection of disease activity, moderate accuracy for both unenhanced and enhanced MRI scores, both JAMRIS and IPSG, was noted, which might be caused by the fact that the majority of patients had either no or minimal clinical disease activity, they pointed out.
Research implications
A limitation of the study is that not all MRI scans were conducted with a dedicated knee coil. In patients requiring MRI of both knees, the exam was carried out in some patients in one single exam using a multichannel body matrix.
Also, only a small number of patients were involved because this was a single-center study with a retrospective study design. For most patients, no follow-up MRI was available to evaluate and correlate with clinical therapy response.
"This is the first study to show unenhanced MR images acquired on a [3-tesla] MRI to detect synovial thickening of the knee joint as reliably as on enhanced MR images," the authors concluded.