Dear MRI Insider,
Both radiologists and clinicians are wary about using biomarkers, particularly because these biomarkers are often acquired with very different imaging protocols, which make the quantitation across sites and equipment variable.
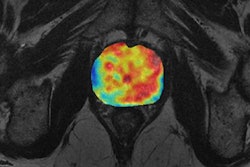
That's the view of Prof. Nandita deSouza and her colleagues at the European Imaging Biomarkers Alliance. They've just released a comprehensive set of recommendations designed to promote the understanding and use of validated imaging biomarkers as decision-making tools in clinical trials and routine practice. The European Society of Radiology has endorsed their 16-page document.
Many important research findings were unveiled at last week's European Society of Cardiology (ESC) congress in Paris. For instance, a study from Leipzig, Germany, that involved nearly 2,500 MRI scans cast new light on white-matter lesions in heart failure patients. The presenters linked the probability of white-matter lesions to the duration of heart failure. Patients with a longstanding diagnosis had more of these lesions compared with those more recently diagnosed.
Our second story from the ESC congress focuses on the latest analysis of mortality rates involving heart disease and cancer in high- and low-income countries. The international group of authors had some surprises for attendees.
Meanwhile, investigators from the U.K. have used 3D MRI to work out a patient's cardiac muscle strain. They think their method can boost the accuracy of quantifying cardiac health without the need for gadolinium contrast.
Prof. Henrik Thomsen, an expert on contrast media safety, remains concerned about gadolinium in tap water. He believes there's an urgent need for more effective water purification systems and better monitoring of gadolinium levels. His comments come in response to a new study of gadolinium contamination in tap water and tap water-based soft drinks from fast-food outlets at six large German cities.
This letter features some of the numerous articles posted over the past few weeks in the MRI Community. Please see below for the full list of our coverage.









![Overview of the study design. (A) The fully automated deep learning framework was developed to estimate body composition (BC) (defined as subcutaneous adipose tissue [SAT] in liters; visceral adipose tissue [VAT] in liters; skeletal muscle [SM] in liters; SM fat fraction [SMFF] as a percentage; and intramuscular adipose tissue [IMAT] in deciliters) from MRI. The fully automated framework comprised one model (model 1) to quantify different BC measures (SAT, VAT, SM, SMFF, and IMAT) as three-dimensional (3D) measures from whole-body MRI scans. The second model (model 2) was trained to identify standardized anatomic landmarks along the craniocaudal body axis (z coordinate field), which allowed for subdividing the whole-body measures into different subregions typically examined on clinical routine MRI scans (chest, abdomen, and pelvis). (B) BC was quantified from whole-body MRI in over 66,000 individuals from two large population-based cohort studies, the UK Biobank (UKB) (36,317 individuals) and the German National Cohort (NAKO) (30,291 individuals). Bar graphs show age distribution by sex and cohort. BMI = body mass index. (C) After the performance assessment of the fully automated framework, the change in BC measures, distributions, and profiles across age decades were investigated. Age-, sex-, and height-adjusted body composition reference curves were calculated and made publicly available in a web-based z-score calculator (https://circ-ml.github.io).](https://img.auntminnieeurope.com/mindful/smg/workspaces/default/uploads/2026/05/body-comp.XgAjTfPj1W.jpg?auto=format%2Ccompress&fit=crop&h=112&q=70&w=112)





