In response to new data showing large variation in the availability and quality of multiparametric MRI (mpMRI) in the U.K., Prostate Cancer UK is calling on the National Health Service (NHS) to prioritize a rollout of the imaging technique for prostate cancer detection.
A freedom of information (FOI) request from Prostate Cancer UK found a 63% increase in access to mpMRI overall in the U.K., but the NHS data also show that many hospitals in Wales and Northern Ireland don't offer the scans, according to the organization. Furthermore, there is significant variation in the availability and quality of mpMRI in England and Scotland, Prostate Cancer UK noted.
Only 57% of areas across the U.K. are providing scans before biopsy to the highest evidence-based standards, while 13% -- including North and West Wales, Northern Ireland, parts of North West England, and parts of Scotland -- do not offer mpMRI, Prostate Cancer UK said.
As a result, the organization is calling on NHS decision-makers in areas without access to mpMRI to prioritize whatever changes are needed to make prebiopsy mpMRI available. The group is also lobbying the NHS on a national level to address the variation in the level and quality of scans being given across the U.K.
"This groundbreaking diagnostic tool is the biggest leap forward in prostate cancer diagnosis for decades, and it is, therefore, appalling that health officials in some areas are still not seeing this as a priority," said Prostate Cancer UK Director of Support and Influencing Heather Blake in a statement. "We urge health departments and commissioners in the worst offending areas to step up and focus their efforts on getting mpMRI before biopsy to men without delay."
The FOI request also found that almost one-third of areas providing mpMRI before biopsy were not providing the study to a sufficiently high standard, with many not using a dynamic contrast agent that proved in the Prostate MR Imaging Study (PROMIS) trial to increase the scan's accuracy, Prostate Cancer UK said. Furthermore, 41% of those locations that do scan to the PROMIS standard are either restricting access to men who fir at particular age or prostate-specific antigen level or just not offering it to all men who could benefit, according to the organization.




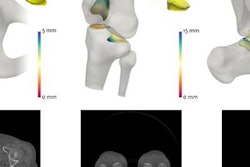






![Overview of the study design. (A) The fully automated deep learning framework was developed to estimate body composition (BC) (defined as subcutaneous adipose tissue [SAT] in liters; visceral adipose tissue [VAT] in liters; skeletal muscle [SM] in liters; SM fat fraction [SMFF] as a percentage; and intramuscular adipose tissue [IMAT] in deciliters) from MRI. The fully automated framework comprised one model (model 1) to quantify different BC measures (SAT, VAT, SM, SMFF, and IMAT) as three-dimensional (3D) measures from whole-body MRI scans. The second model (model 2) was trained to identify standardized anatomic landmarks along the craniocaudal body axis (z coordinate field), which allowed for subdividing the whole-body measures into different subregions typically examined on clinical routine MRI scans (chest, abdomen, and pelvis). (B) BC was quantified from whole-body MRI in over 66,000 individuals from two large population-based cohort studies, the UK Biobank (UKB) (36,317 individuals) and the German National Cohort (NAKO) (30,291 individuals). Bar graphs show age distribution by sex and cohort. BMI = body mass index. (C) After the performance assessment of the fully automated framework, the change in BC measures, distributions, and profiles across age decades were investigated. Age-, sex-, and height-adjusted body composition reference curves were calculated and made publicly available in a web-based z-score calculator (https://circ-ml.github.io).](https://img.auntminnieeurope.com/mindful/smg/workspaces/default/uploads/2026/05/body-comp.XgAjTfPj1W.jpg?auto=format%2Ccompress&fit=crop&h=112&q=70&w=112)





