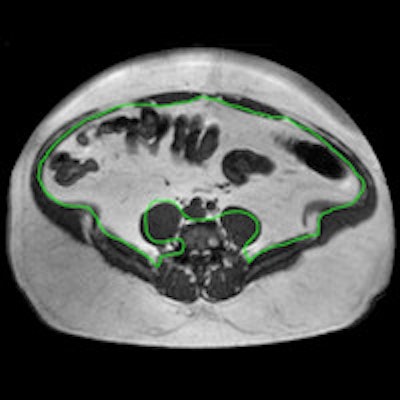
MRI analysis of abdominal fat can give an indication of cardiovascular risk in overweight and obese people, and new protocols developed at the Leipzig obesity clinic and presented at the German Congress of Radiology (DRK) can reduce this previously time-consuming task to a matter of minutes.
Not all fat is equal. Very overweight people have a higher risk of heart attack and other cardiovascular disease if the fat is concentrated in the abdomen, and visceral fat is also a much stronger indicator than the subcutaneous variety of the likelihood of diabetes mellitus, with all its consequences.
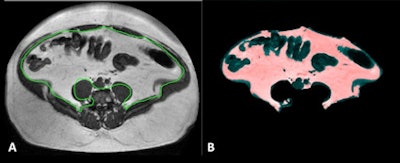 Above: MRI section of a 39-year-old patient, measured at the second and third lumbar vertebrae. The visceral fat is enclosed by the green line in A, and shaded pink in B. Sections of the large intestine are visible in the abdomen. Clinical images courtesy of Klinik für Diagnostische und Interventionelle Radiologie, Universitätsklinikum Leipzig. Below: MRI sections at the second and third lumbar vertebrae in two obese patients. Patient A had much more visceral fat (inside the green line) than patient B, but both had an almost identical body mass index of around 45 kg/m2.
Above: MRI section of a 39-year-old patient, measured at the second and third lumbar vertebrae. The visceral fat is enclosed by the green line in A, and shaded pink in B. Sections of the large intestine are visible in the abdomen. Clinical images courtesy of Klinik für Diagnostische und Interventionelle Radiologie, Universitätsklinikum Leipzig. Below: MRI sections at the second and third lumbar vertebrae in two obese patients. Patient A had much more visceral fat (inside the green line) than patient B, but both had an almost identical body mass index of around 45 kg/m2."Because of this correlation between abdominal fat and cardiovascular risk, it can be a good idea to use MRI to measure abdominal fat in overweight patients," explained Dr. Alexander Schaudinn of the diagnostic and interventional radiology clinic/IFB AdipositasErkrankungen at Leipzig University Hospital.
.png?auto=format%2Ccompress&fit=max&q=70&w=400) Patients at the Leipzig obesity clinic. Image courtesy of IFB Adipositas.
Patients at the Leipzig obesity clinic. Image courtesy of IFB Adipositas.Until now, this has been a very elaborate process. The whole abdomen has to be measured centimeter by centimeter, from the diaphragm to the pelvic floor. The patient has to spend almost 15 minutes in the scanner, and it then takes up to half an hour to analyze an average of 40 sections. But in a study using MRI data from 192 overweight men and women, Schaudinn and his colleagues have found a much quicker way of doing this.
Presenting the study at a scientific session this week at the 96th DRK, he said they started by measuring abdominal fat volumes section by section in the conventional manner, and then compared the results with two much quicker methods in which fat was extrapolated from a single section and from blocks of five sections.
"We can estimate total abdominal fat very accurately from one section," he said. "But if we use blocks of five, the result is even closer to that of a complete analysis."
 Dr. Alexander Schaudinn from Leipzig University Hospital. Image courtesy of Alina Simmelbauer.
Dr. Alexander Schaudinn from Leipzig University Hospital. Image courtesy of Alina Simmelbauer.The team also assessed how the five sections should be chosen to give as accurate a result as possible. In women, they should be taken at the third and fourth lumbar vertebrae, while in men the results are more accurate if a slightly higher measurement is taken at the second and third lumbar vertebrae.
So could this method be used to monitor the results of weight reduction treatment? Analyzing blocks of five sections instead of the usual 40 saves a lot of time -- it takes around four minutes -- and this could make abdominal fat measurement easier in everyday clinical practice, according to Schaudinn.
He thinks the technique will also be valuable in clinical studies involving overweight patients.
"One interesting question is whether our method can assess how abdominal fat is changed by diet, exercise, or stomach reduction surgery. We're now carrying out a further study of this, and we're hoping to present the results soon," he concluded.
Editor's note: This article is an edited version of a translation of an article published in German online on 13 May 2015 by the German Radiological Society (DRG, Deutsche Röntgengesellschaft). Translation by Syntacta Translation & Interpreting. To read the original article, visit the DRG website.











![Overview of the study design. (A) The fully automated deep learning framework was developed to estimate body composition (BC) (defined as subcutaneous adipose tissue [SAT] in liters; visceral adipose tissue [VAT] in liters; skeletal muscle [SM] in liters; SM fat fraction [SMFF] as a percentage; and intramuscular adipose tissue [IMAT] in deciliters) from MRI. The fully automated framework comprised one model (model 1) to quantify different BC measures (SAT, VAT, SM, SMFF, and IMAT) as three-dimensional (3D) measures from whole-body MRI scans. The second model (model 2) was trained to identify standardized anatomic landmarks along the craniocaudal body axis (z coordinate field), which allowed for subdividing the whole-body measures into different subregions typically examined on clinical routine MRI scans (chest, abdomen, and pelvis). (B) BC was quantified from whole-body MRI in over 66,000 individuals from two large population-based cohort studies, the UK Biobank (UKB) (36,317 individuals) and the German National Cohort (NAKO) (30,291 individuals). Bar graphs show age distribution by sex and cohort. BMI = body mass index. (C) After the performance assessment of the fully automated framework, the change in BC measures, distributions, and profiles across age decades were investigated. Age-, sex-, and height-adjusted body composition reference curves were calculated and made publicly available in a web-based z-score calculator (https://circ-ml.github.io).](https://img.auntminnieeurope.com/mindful/smg/workspaces/default/uploads/2026/05/body-comp.XgAjTfPj1W.jpg?auto=format%2Ccompress&fit=crop&h=112&q=70&w=112)





