
A new method for classifying breast microcalcifications using x-ray phase-contrast imaging was presented at the RSNA 2014 meeting. The technique may help improve early breast cancer diagnosis, increase diagnostic accuracy, and reduce the number of biopsies of suspicious lesions, Swiss researchers believe.
Microcalcifications are calcium deposits that may be present in areas of accelerated cell turnover, an indicator of early invasive breast cancer or precancerous changes in breast tissue. Two types exist, with type I microcalcifications being most associated with benign lesions and type II most often found in malignant lesions. Each has a different chemical composition and different absorption and scattering properties.
Marco Stampanoni, PhD, from ETH Zurich and the Paul Scherrer Institut in Switzerland, described an approach that he and his colleagues have developed, which exploits the complementary nature of microcalcification absorption and small-angle scattering signals obtained simultaneously with an x-ray grating interferometer on a conventional x-ray tube.
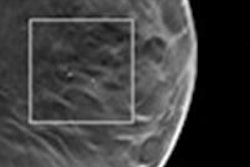
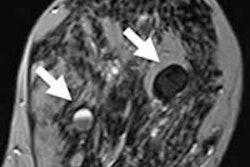
 If confirmed, the new method would allow discrimination between type I (green) and type II (red) microcalcifications in a noninvasive way.
If confirmed, the new method would allow discrimination between type I (green) and type II (red) microcalcifications in a noninvasive way.The method relies on the observation that some microcalcifications show opposite absorption and small-angle scattering signals. The novel technique is highly sensitive to the morphological and structural information of the microcalcifications, where conventional absorption-based x-ray mammography is not.
Stampanoni explained that the two types of microcalcifications are notably difficult to distinguish using conventional mammography. Coarse morphological information can be obtained from absorption-based images, but not the microstructure. Nor can conventional mammography determine the thickness of a microcalcification.
"By considering the small-angle scattering signal as complementary to the absorption signal, our method can analyze the differences in the attenuation coefficient as well as in scattering power of the microcalcifications to decouple the thickness parameter," he explained.
Distinguishing features
Stampanoni's presented hypothesis assumes that for any given microcalcification thickness, one type gives a weaker absorption signal, but a stronger small-angle scattering signal, than the other. Type I microcalcifications generally show a smaller attenuation signal and are crystalline in nature, whereas type II are not. Therefore, type I microcalcifications are expected to give a higher scattering signal than type II.
 Marco Stampanoni is professor for x-ray imaging at ETH Zurich and head of the tomography group of the Swiss Light Source at the Paul Scherrer Institut in Switzerland.
Marco Stampanoni is professor for x-ray imaging at ETH Zurich and head of the tomography group of the Swiss Light Source at the Paul Scherrer Institut in Switzerland.The researchers initially studied whole-breast samples obtained from patients who had undergone mastectomies after being diagnosed with invasive breast cancer. They are currently testing their hypothesis that the positive predictive value (PPV) of phase-contrast x-ray imaging using Talbot-Lau grating interferometry is two times larger than that of conventional mammography, using biopsy samples of 20 patients with suspicious microcalcifications undergoing vacuum-assisted breast biopsy.
An article published earlier this year in Nature Communications describes the technique, validation, and classification research in detail (Nature Comm., 15 May 2014). Stampanoni emphasized that although the research identified some deposits showing opposite scattering and absorption behaviors that very likely had different chemical (composition) and physical (morphology and grain size) properties, much stronger statistical evidence is still needed to support the hypothesis.
He noted the initial research was severely biased by the fact that all samples were from patients with cancer. Therefore, the likelihood of finding type II microcalcifications was much larger than that for type I.
"We need to access tissue samples from a larger variety of patients, carrying both types of microcalcifications," he said. "These need to be investigated using our technology and we need to validate each measurement with comprehensive histopathology. This type of study will be much more involved and much more difficult than all that has been undertaken so far. It will require significant effort on the clinical and technical sides. And there are ethical issue relating to obtain a diversified sampling of tissues that need to be addressed."
"However," Stampanoni concluded, "if our hypothesis is validated by future research, it may help reduce the number of biopsies that prove to be unneeded, or in the case of a patient with widespread microcalcifications, to select the optimal biopsy site. This would benefit women with suspicious findings and also help reduce the cost of breast cancer detection and diagnosis."
© IOP Publishing Limited. Republished with permission from medicalphysicsweb, a community website covering fundamental research and emerging technologies in medical imaging and radiation therapy.










![Overview of the study design. (A) The fully automated deep learning framework was developed to estimate body composition (BC) (defined as subcutaneous adipose tissue [SAT] in liters; visceral adipose tissue [VAT] in liters; skeletal muscle [SM] in liters; SM fat fraction [SMFF] as a percentage; and intramuscular adipose tissue [IMAT] in deciliters) from MRI. The fully automated framework comprised one model (model 1) to quantify different BC measures (SAT, VAT, SM, SMFF, and IMAT) as three-dimensional (3D) measures from whole-body MRI scans. The second model (model 2) was trained to identify standardized anatomic landmarks along the craniocaudal body axis (z coordinate field), which allowed for subdividing the whole-body measures into different subregions typically examined on clinical routine MRI scans (chest, abdomen, and pelvis). (B) BC was quantified from whole-body MRI in over 66,000 individuals from two large population-based cohort studies, the UK Biobank (UKB) (36,317 individuals) and the German National Cohort (NAKO) (30,291 individuals). Bar graphs show age distribution by sex and cohort. BMI = body mass index. (C) After the performance assessment of the fully automated framework, the change in BC measures, distributions, and profiles across age decades were investigated. Age-, sex-, and height-adjusted body composition reference curves were calculated and made publicly available in a web-based z-score calculator (https://circ-ml.github.io).](https://img.auntminnieeurope.com/mindful/smg/workspaces/default/uploads/2026/05/body-comp.XgAjTfPj1W.jpg?auto=format%2Ccompress&fit=crop&h=112&q=70&w=112)




