For BI-RADS 0 cases, researchers from Austria have found breast MRI can reliably exclude malignancy with a sensitivity of 100%, which means it's just as accurate as needle biopsy for excluding breast cancer.
The American College of Radiology (ACR) defines BI-RADS 0 cases as breast findings that are incompletely assessed on conventional mammography or ultrasound and, thus, need additional imaging. The exact localization of potential disease is unclear (i.e., architectural distortion or multiple masses).
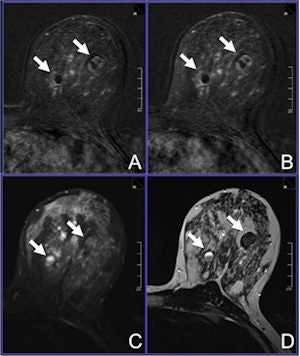
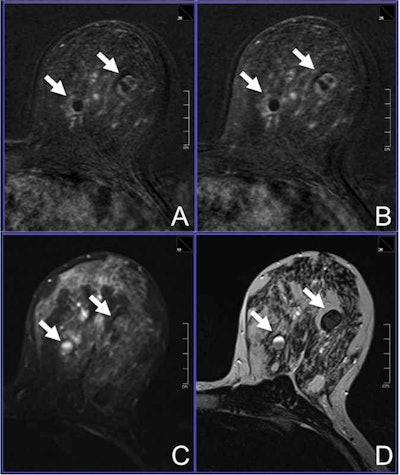
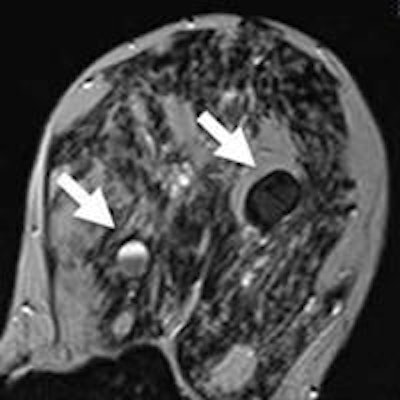
A 42-year-old woman was referred to MRI due to dense breast tissue and multiple cystic lesions, several of them showing inhomogeneous echogeneity and dorsal acoustic shadowing, classified as BI-RADS 0. A: Early contrast-enhanced T1-weighted subtraction. B: Delayed contrast-enhanced T1-subtraction. C: Short tau inversion-recovery image. D: T2-weighted, turbo spin-echo image reveals the lesions to be proteinaceous cysts (arrows). Image courtesy of Dr. Claudio Spick.
Breast MRI is a good option as the modality has already proved itself to be the optimal strategy for lesion diagnosis and patient management in certain clinical situations, according to Dr. Claudio Spick from the biomedical imaging and image-guided therapy department at the Medical University of Vienna (European Journal of Radiology, 19 October 2014). However, there is no clear consensus about the use of breast MRI (when there are equivocal findings) as a problem-solving tool for BI-RADS 0 findings on conventional imaging, he wrote in an email to AuntMinnieEurope.com.
What the guidelines say
According to the European Society of Breast Imaging (EUSOBI) recommendations, one of the most important indications for breast MRI is problem-solving in cases of inconclusive findings at conventional imaging. Due to a lack of evidence, the European Society of Breast Cancer Specialists (EUSOMA) recommendations and ACR guidelines state there is no evidence in favor of breast MRI for characterizing equivocal findings at conventional imaging when additional mammographic views or needle biopsy procedures can be performed.
"These statements leave broad space for interpretation and, as a consequence, reimbursement problems occur," Spick wrote. "Thus, patients cannot receive MRI for problem-solving, but have to undergo a number of additional examinations and even unnecessary invasive procedures with all associated physical and psychological drawbacks."
He and his colleagues sought to evaluate the diagnostic performance of breast MRI if used as a problem-solving tool in BI-RADS 0 cases. In Austria, using breast MRI for BI-RADS 0 cases is clinically established and reimbursed, although this is not always the case in other countries.
They included 687 women in the study, each of whom underwent high-resolution, 3D, dynamic, and contrast-enhanced breast MRI. Until 1 July 2012, imaging was conducted on a 1.5-tesla system from Siemens Healthcare (Magnetom Symphony) and after that on a 3-tesla system from Siemens (MagnetomVerio). Of the patients, 111 were categorized as BI-RADS 0.
Research findings
The breast MRI findings were stratified by clinical presentations, conventional imaging findings, and breast density. The results were compared with the reference standard -- histopathology or an imaging follow-up of at least one year.
Conventional imaging showed 27% of the BI-RADS 0 patients had mammographic masses, 51.4% had mammographic architectural distortions, 4.5% had mammographic microcalcifications, and 15.3% had ultrasound-only findings. Also, two patients had palpable findings without imaging correlates.
There were 15 true-positive, 85 true-negative, 11 false-positive, and zero false-negative breast MRI findings.
- Sensitivity: 100%
- Specificity: 88.5%
- Positive predictive value: 57.7%
- Negative predictive value: 100%
The results show that breast MRI is as accurate as needle biopsy for excluding breast cancer, Spick wrote in his email. "Furthermore, BI-RADS 0 cases are not lesions directly accessible by percutaneous needle biopsy. In complicated cases, you cannot be sure whether your needle hit the lesion or not, and follow-up examinations are regularly recommended after biopsy. The patient does still not feel secure. A negative MRI finding is much more helpful both clinically and psychologically."
As a consequence, radiologists and perhaps patients may prefer breast MRI to other means of further workup. Of course, if there is a solid lesion that is detected with mammography and can be seen with ultrasound, a biopsy is the simplest way to exclude cancer, he added.
"However, in clinical practice radiologists are often faced with multiple breast lesions and complicated cases," Spick wrote. "These ones can be safely evaluated with breast MRI."
Study limitations
The study has some limitations, however. The reasons for referral in terms of imaging findings were heterogeneous so subgroup analyses are underpowered. Yet the authors are quick to point out they have sufficiently answered the main research question as to whether malignancy can be reliably excluded using MRI for BI-RADS 0 patients.
Of note, the rate of malignancy in their study was 13.5% and, thus, higher than in previous studies, they added. "This might be due to a possible selection bias by referring physicians, sending more problematic cases for further workup with breast MRI."
As mentioned, in Austria, breast MRI as a problem-solving tool is reimbursed by insurance companies, explaining the relatively high rate of MRI referred for problem-solving, the authors explained.
"However, this should not be seen as a limitation, as our study population reflects the actual clinical situation investigated," they wrote. "Further, the 1.5 T MRI system of our institution was replaced by a new 3 T system during the time of this study. The patient numbers included in this study do not allow for a detailed analysis whether the more modern equipment improved our diagnostic accuracy in terms of specificity."
A final limitation is the researchers defined a follow-up interval of 12 months for histologically unverified cases, while the current clinical standard is 24 months.
Whether using breast MRI to exclude malignancy for BI-RADS 0 patients is cost-effective remains to be seen as there is a lack of systematic data, the researchers acknowledged.
"Many people think breast MRI may exclude malignancy but at the cost of additional findings that need further follow-up," Spick wrote. "Although our study shows that rate cannot be high, future research should stratify findings into known versus incidental lesions identified by MRI."