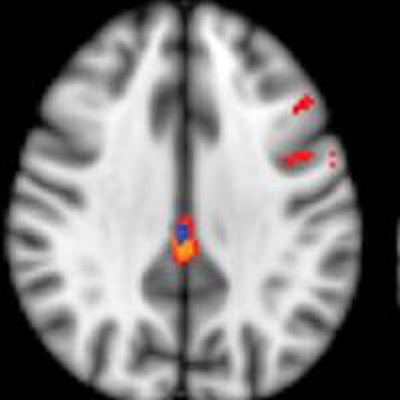
Using arterial spin-labeled (ASL) MRI, Swiss researchers found evidence of cognitive decline in the brains of healthy elderly individuals before symptoms appeared, according to a new study published online on 7 October in Radiology.
Initial ASL-MRI scans showed decreased cerebral blood flow in the posterior cingulate cortex region of the brain in approximately half of the healthy subjects in the study, who later developed subtle cognitive decline.
Given the results, the research team, led by Dr. Aikaterini Xekardaki from University Hospitals of Geneva, believes that ASL has the "potential to serve as a biomarker in the very early diagnosis of preclinical dementia" and may be an alternative to neuropsychological testing (Radiology, 7 October 2014).
The posterior cingulate cortex is associated with the default mode network, which is active when the brain is not concentrating on a specific task. Less perfusion indicates decreased neural activity; thus, declines in this network are seen in patients with mild cognitive impairment and are more pronounced in those with Alzheimer's disease.
Early diagnosis
Early signs of mild cognitive impairment and dementia are particularly important because while it's unlikely that medication will be able to restore lost cognitive function, it might stop or slow cognitive decline.
"Therefore, diagnosis should be done at the earliest possible stage," co-author Dr. Sven Haller, an associate professor of neuroscience at the University of Geneva, told AuntMinnieEurope.com. "The difficulty here is to discriminate 'normal' forgetfulness in aging from the earliest manifestation of cognitive decline, which will eventually lead to dementia."
Conventional MRI provides structural information, while ASL-MRI offers functional information by measuring cerebral blood flow. "ASL is, therefore, complimentary to conventional MRI," Haller said. "Moreover, functional alterations in the brain probably can be detected earlier than structural alterations, but this is a topic of current debate."
While previous studies have shown that ASL-MRI might be helpful in discerning mild cognitive impairment and Alzheimer's disease, "we went one step earlier and investigated cognitively intact elderly individuals at the time of imaging," he added.
The study included 148 consecutive healthy control subjects scanned between October 2010 and January 2011. ASL-MRI was performed at baseline on all participants with a whole-body, 3-tesla scanner (Magnetom Trio, Siemens Healthcare), and a neuropsychological assessment was used to assess cognitive ability.
Eighteen months after the baseline evaluation, subjects again underwent neuropsychological assessment. If the results were lower by at least 0.5 for two or more of the tests administered, they were placed in the deteriorated cognitive function group.
The low follow-up threshold of neuropsychological decline of -0.5 standard deviation compared with baseline was used "to explore the initial phases of cognitive decline in healthy control subjects," the authors explained.
Follow-up declines
At the 18-month follow-up, the researchers found that 75 subjects had remained stable. The remaining 73 had deteriorated cognitively and also showed reduced perfusion in their ASL-MRI exams at baseline, particularly in the posterior cingulate cortex.
"About half of [the subjects] developed subtle cognitive decline at 18 months," Haller said. "ASL at baseline was able to discriminate stable versus deteriorating controls and ASL was able to detect the earliest form of cognitive decline."
The researchers also discovered similar ASL patterns between the control subjects with reduced cognitive function and patients with mild cognitive impairment (65 patients with mild cognitive impairment were also examined for the study). The finding indicates that people with deteriorated cognitive function "already have perfusion alterations at baseline imaging despite apparent normal cognition because of mobilization of the neurocognitive reserve," they wrote.
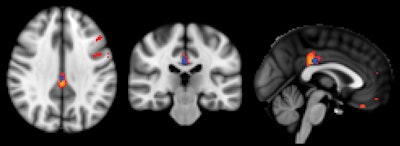 ASL-MRI showed decreased relative cerebral blood flow in the posterior cingulate cortex in subjects with deteriorated cognitive function versus those with stable cognitive function. Image courtesy of Radiology.
ASL-MRI showed decreased relative cerebral blood flow in the posterior cingulate cortex in subjects with deteriorated cognitive function versus those with stable cognitive function. Image courtesy of Radiology.Regarding the performance of ASL-MRI, the scan "simply prolongs an already existing MRI investigation for a few minutes without irradiation or contrast agent and is therefore minimally [disruptive] for the patients," Haller said. "Yet it provides complimentary information, which might help the early diagnosis of cognitive decline" and improve the identification of patients at risk, potentially leading to treatment that could slow or stop further decline.
The researchers also speculated that ASL-MRI could become a standalone test or an adjunct to PET imaging for dementia.
Haller and colleagues plan to increase their study sample and follow the current subjects "to see whether participants with the earliest form of cognitive decline will further progress to dementia, and to see whether ASL may also discriminate participants with slow versus fast cognitive decline," he said.










![Overview of the study design. (A) The fully automated deep learning framework was developed to estimate body composition (BC) (defined as subcutaneous adipose tissue [SAT] in liters; visceral adipose tissue [VAT] in liters; skeletal muscle [SM] in liters; SM fat fraction [SMFF] as a percentage; and intramuscular adipose tissue [IMAT] in deciliters) from MRI. The fully automated framework comprised one model (model 1) to quantify different BC measures (SAT, VAT, SM, SMFF, and IMAT) as three-dimensional (3D) measures from whole-body MRI scans. The second model (model 2) was trained to identify standardized anatomic landmarks along the craniocaudal body axis (z coordinate field), which allowed for subdividing the whole-body measures into different subregions typically examined on clinical routine MRI scans (chest, abdomen, and pelvis). (B) BC was quantified from whole-body MRI in over 66,000 individuals from two large population-based cohort studies, the UK Biobank (UKB) (36,317 individuals) and the German National Cohort (NAKO) (30,291 individuals). Bar graphs show age distribution by sex and cohort. BMI = body mass index. (C) After the performance assessment of the fully automated framework, the change in BC measures, distributions, and profiles across age decades were investigated. Age-, sex-, and height-adjusted body composition reference curves were calculated and made publicly available in a web-based z-score calculator (https://circ-ml.github.io).](https://img.auntminnieeurope.com/mindful/smg/workspaces/default/uploads/2026/05/body-comp.XgAjTfPj1W.jpg?auto=format%2Ccompress&fit=crop&h=112&q=70&w=112)





