
NEW YORK (Reuters Health), Aug 11 - When cardiac resynchronization improves left ventricular (LV) function in heart failure patients, it improves their cerebral blood flow as well, a small study has shown.
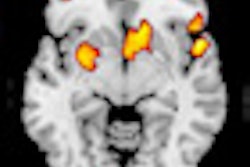
"Cerebral blood flow is decreased in symptomatic patients with heart failure, and this might contribute to the impaired cognitive performance frequently observed in these patients," the researchers write in the July issue of the American Journal of Cardiology. Cardiac resynchronization therapy (CRT) improves their cognition along with their heart failure symptoms and quality of life, but little is known about the effect of CRT on cerebral blood flow.
Dr. Rutger van Bommel and colleagues at Leiden University Medical Center in the Netherlands followed 32 heart failure patients after CRT device implantation. They also followed another 14 patients, matched for age, gender, New York Heart Association class, and LV function, who were not candidates for CRT.
At six months, 16 CRT patients had responded; that is, they had reductions in LV end-systolic volume of at least 15%. On transcranial Doppler exams, responders also had significant increases in peak systolic velocity (from 83 cm/s at baseline to 100 cm/s; p = 0.001), end-diastolic velocity (from 29 to 37 cm/s; p < 0.001), and mean velocity (from 47 to 58 cm/s; p < 0.001).
Neither the nonresponders nor the control patients had any significant changes in cerebral blood flow.
There was a strong correlation between reduction in left ventricular end-systolic volume and an increase in mean velocity on transcranial Doppler, the authors say.
"It is clinically relevant in that CRT improves not only cardiac function, but with improved cardiac function, blood flow to the brain improves," coauthor Dr. Jeroen Bax told Reuters Health by e-mail. "With that, it is anticipated that cognitive function may improve. It also shows that CRT has a more global effect, rather than just regional on the heart only."
By Dave Levitan
Source: http://link.reuters.com/hef54n
Am J Cardiol 2010;106:73-77.
Last Updated: 2010-08-11 11:41:08 -0400 (Reuters Health)
Related Reading
Coronary MR protocol picks veins favorable for resynchronization therapy, May 22, 2007
Copyright © 2010 Reuters Limited. All rights reserved. Republication or redistribution of Reuters content, including by framing or similar means, is expressly prohibited without the prior written consent of Reuters. Reuters shall not be liable for any errors or delays in the content, or for any actions taken in reliance thereon. Reuters and the Reuters sphere logo are registered trademarks and trademarks of the Reuters group of companies around the world.


![Overview of the study design. (A) The fully automated deep learning framework was developed to estimate body composition (BC) (defined as subcutaneous adipose tissue [SAT] in liters; visceral adipose tissue [VAT] in liters; skeletal muscle [SM] in liters; SM fat fraction [SMFF] as a percentage; and intramuscular adipose tissue [IMAT] in deciliters) from MRI. The fully automated framework comprised one model (model 1) to quantify different BC measures (SAT, VAT, SM, SMFF, and IMAT) as three-dimensional (3D) measures from whole-body MRI scans. The second model (model 2) was trained to identify standardized anatomic landmarks along the craniocaudal body axis (z coordinate field), which allowed for subdividing the whole-body measures into different subregions typically examined on clinical routine MRI scans (chest, abdomen, and pelvis). (B) BC was quantified from whole-body MRI in over 66,000 individuals from two large population-based cohort studies, the UK Biobank (UKB) (36,317 individuals) and the German National Cohort (NAKO) (30,291 individuals). Bar graphs show age distribution by sex and cohort. BMI = body mass index. (C) After the performance assessment of the fully automated framework, the change in BC measures, distributions, and profiles across age decades were investigated. Age-, sex-, and height-adjusted body composition reference curves were calculated and made publicly available in a web-based z-score calculator (https://circ-ml.github.io).](https://img.auntminnieeurope.com/mindful/smg/workspaces/default/uploads/2026/05/body-comp.XgAjTfPj1W.jpg?auto=format%2Ccompress&fit=crop&h=100&q=70&w=100)





![Overview of the study design. (A) The fully automated deep learning framework was developed to estimate body composition (BC) (defined as subcutaneous adipose tissue [SAT] in liters; visceral adipose tissue [VAT] in liters; skeletal muscle [SM] in liters; SM fat fraction [SMFF] as a percentage; and intramuscular adipose tissue [IMAT] in deciliters) from MRI. The fully automated framework comprised one model (model 1) to quantify different BC measures (SAT, VAT, SM, SMFF, and IMAT) as three-dimensional (3D) measures from whole-body MRI scans. The second model (model 2) was trained to identify standardized anatomic landmarks along the craniocaudal body axis (z coordinate field), which allowed for subdividing the whole-body measures into different subregions typically examined on clinical routine MRI scans (chest, abdomen, and pelvis). (B) BC was quantified from whole-body MRI in over 66,000 individuals from two large population-based cohort studies, the UK Biobank (UKB) (36,317 individuals) and the German National Cohort (NAKO) (30,291 individuals). Bar graphs show age distribution by sex and cohort. BMI = body mass index. (C) After the performance assessment of the fully automated framework, the change in BC measures, distributions, and profiles across age decades were investigated. Age-, sex-, and height-adjusted body composition reference curves were calculated and made publicly available in a web-based z-score calculator (https://circ-ml.github.io).](https://img.auntminnieeurope.com/mindful/smg/workspaces/default/uploads/2026/05/body-comp.XgAjTfPj1W.jpg?auto=format%2Ccompress&fit=crop&h=112&q=70&w=112)








