An artificial intelligence-based computer-aided detection (CAD) system that analyzes prostate MR images for tumors improves the targeting of core biopsies for cancer diagnosis, according to Italian research presented at ECR 2017. With additional fine-tuning, the system could be implemented to improve patient care by significantly outperforming systematic transrectal ultrasound-guided (TRUS) biopsy to point out likely areas of malignancy.
In their study, researchers from the University of Rome enrolled nearly 100 patients with suspected prostate cancer, comparing with histology both the target biopsy area according to the Prostate Imaging and Data Reporting System (PI-RADS version 2), and the Watson elementary CAD scheme (Watson Medical) scheme on MRI. When CAD was applied to areas within PI-RADS version 2, targeted biopsy areas, known as target-in-target, improved localization of prostate cancers occurred.
 Analyzing MRI T2-weighted images, DW images, and DCE images, Watson Elementary creates a colorimetric map depicting the suspiciousness of regions of interest for prostate cancer, based on a Malignancy Attention Index (MAI) ranging from 0 (blue) to 1 (red). The artificial intelligence-based algorithm in the CAD system is based on a per-voxel correlation with histology-confirmed malignancy. The study analyzed regions scoring MAI 0.6 or higher that were within the contours of suspicious areas identified by radiologists. All images courtesy of Dr. Riccardo Campa.
Analyzing MRI T2-weighted images, DW images, and DCE images, Watson Elementary creates a colorimetric map depicting the suspiciousness of regions of interest for prostate cancer, based on a Malignancy Attention Index (MAI) ranging from 0 (blue) to 1 (red). The artificial intelligence-based algorithm in the CAD system is based on a per-voxel correlation with histology-confirmed malignancy. The study analyzed regions scoring MAI 0.6 or higher that were within the contours of suspicious areas identified by radiologists. All images courtesy of Dr. Riccardo Campa."The CAD system improved our detection rate when used to identify target-into-target areas," said Dr. Riccardo Campa from the University of Rome in his talk. Campa's co-authors were Dr. Vincenzo Salvo, Dr. Maurizio Del Monte, Dr. Valeria Panebianco, and radiology section chief Dr. Carlo Catalano.
The European Association of Urology has confirmed that TRUS biopsy is now the gold standard, but new approaches to improve early detection, such as MRI-guided biopsy and ultrasound-MRI fusion biopsy, are gaining traction for their ability to outperform systematic core biopsy, he said.
"Recent studies say targeted biopsy is exceeding the 12-core systematic biopsy in detection rate, especially in clinically significant prostate cancer," Campa said, adding that the use of MRI in particular is growing rapidly for use in prostate cancer diagnosis.
Until recently, however, CAD has been absent from the prostate cancer equation, even though it has already become indispensible for detecting a wide range of pathologies in other branches of medicine, he continued.
Testing out CAD
The purpose of their study was to improve the TRUS-MRI fusion biopsy in the detection rate of prostate cancer with the aid of a CAD system, namely the investigational Watson Elementary CAD system that processes multiparametric MRI images including T2-weighted, diffusion-weighted (DW), and delayed contrast-enhanced (DCE) image sets and generates screen representations of the analyses that can be analyzed in all spatial dimensions, Campa explained. DCE images can be analyzed temporally.
Watson Elementary works by analyzing apparent diffusion coefficient (ADC) values and pharmacokinetic parameters such as k-trans values and their voxel-by-voxel correspondences. It generates a colorized voxel-by-voxel map of suspiciousness level that indicates the malignancy attention index (MAI) that facilitates the identification and localization of regions of interest, he noted. The MAI ranges from 0, not suspicious, to 1, highly suspicious, for prostate cancer. By applying color overlays, the CAD system offers efficient overviews of various regions of interest in the prostate anatomy.
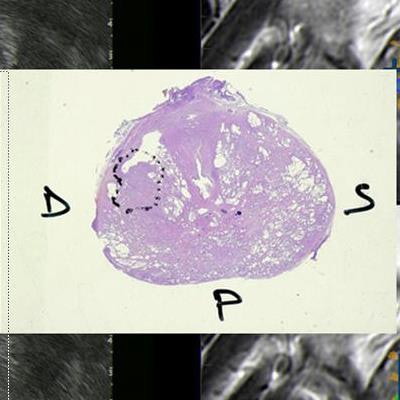
 Core biopsies were acquired within suspicious regions that were delineated by radiologists, and also scored MAI 0.6 or higher. The red lines indicate the radiological analysis contours. Using this target-into-target method increased the percentage of tumor detected per core by 25%.
Core biopsies were acquired within suspicious regions that were delineated by radiologists, and also scored MAI 0.6 or higher. The red lines indicate the radiological analysis contours. Using this target-into-target method increased the percentage of tumor detected per core by 25%.The study enrolled 96 patients with prostate-specific antigen scores ranging from 4 ng/dl to 18 ng/dl and no previous biopsies that were positive for prostate cancer. Images were acquired on a 3-tesla Discovery 750 MR scanner (GE Healthcare) using a 32-channel superficial coil. T2-weighted images were acquired in the axial and coronal planes; diffusion-weighted images were acquired for six different B values up to 1,500 s/mm2.
Two experienced radiologists performed the radiological analysis using PI-RADS v2. Watson Elementary CAD was then applied for its analysis and delineation of suspicious areas. Selection of areas for biopsy included PI-RADS areas with a density of 3 or greater, a volume of 0.1 cc or greater, and an MAI value of 0.6 or greater, Campa said.
"When the CAD target overlapped with the radiology target, we performed a biopsy in the overlapping area called target-into-target," he said.
The investigators obtained between one and four cores for each target. MRI-TRUS fusion biopsies were performed using the Koelis Urostation and MyLab Class C (Esaote).
To evaluate CAD's diagnostic value, receiver operating characteristic (ROC) curves were created from both the CAD and the radiologic analyses, including ADC and k-trans values of each target type. The prostate cancer detection rate was determined by the percentage of positive targets obtained in biopsy. The overall detection rate performance of biopsy was 85% for clinically significant cancer for both PI-RADS and Watson systems. CAD also increased the percentage of tumor detected per core by 25%, targeting the precise cancer zone into the lesion to be biopsied in the target-into-target system.
Better targeting with CAD
"The results show that radiological analysis yields better diagnostic performance compared to CAD," he said. To yield high specificity, the cutoff value for the f PI-RADS score must be set between 3 and 4, Campa added.
 Dr. Riccardo Campa from the University of Rome.
Dr. Riccardo Campa from the University of Rome.The diagnostic performance of Watson Elementary in the detection of prostate cancer is similar to that of PI-RADS v2, he concluded, but Watson elementary CAD system is "useful in identifying the most involved area by cancer within the focus bordered with MRI," he said. As a result, Watson can help direct the tumor biopsy to improve the percentage of tumor per core.
As for limitations, "we speculate that CAD is too k-trans-based, with too much importance give to the DCE image sets in contrast to the PI-RADS score, and that it is too focused on transitional zone in contrast with the epidemiological data," Campa said.
CAD improved the detection rate specifically when used in target-into-target areas, he said. Analysis of these areas can help guide the decision to biopsy in PI-RADS 3 patients, but "we need more data from prostatectomy to analyze MAI values to achieve significant results in this subgroup," he said. As a result, CAD is a useful adjunct to expert radiological analysis.