The incidence of severe gastrointestinal illness due to eating undercooked or raw fish and seafood is rising, and CT is proving valuable in these patients. A group of Spanish radiologists have shared their clinical experiences.
Anisakiasis is a parasitosis with principally gastrointestinal involvement, associated with the ingesting of anisakis nematode larvae in undercooked fish or seafood. More than 90% of the approximately 20,000 yearly cases occur in Japan, but a rising trend has been observed in Europe and North America, according to Dr. Roberto Fornell-Pérez and colleagues at the Basurto University Hospital in Bilbao.
"The presence of different radiological signs makes it advisable to include anisakiasis in the differential diagnosis of acute abdomen," they wrote in an article posted on 13 November by Insights into Imaging. "Intestinal and multifocal involvement rates are greater than previously reported."
The symptoms are nonspecific, usually presenting as an acute abdominal condition of variable severity, and on occasion associated with allergic symptoms. The latency period of the ingestion of parasites and clinical manifestations is variable, depending on the affected area of the digestive tract, the researchers explained.
The interval in gastric involvement is usually less than 24 hours, but the interval in intestinal cases is usually greater (up to a week), which makes the association between the emergency conditions and the high-risk food difficult in carrying out the anamnesis.
"The diagnostic suspicion is oriented towards more common inflammatory conditions such as appendicitis, cholecystitis or diverticulitis," they pointed out. "Diagnostic certainty is provided by direct observation of the parasites in endoscopic tests or in surgery. However, in the context of a non-specific acute abdominal condition, it is frequent to turn to assessment by means of imaging tests."
The posing of possible anisakiasis through radiological findings could be key in guiding the clinician in unsuspected cases, mainly in intestinal cases, given the nonspecific clinical manifestations and the longer time transpired from contamination, they added.
Key findings and analysis
At Basurto University Hospital, 231 cases of acute abdominal condition were diagnosed as gastrointestinal anisakiasis between January 2010 and December 2021. Emergency radiological studies were carried out in 144 patients, of whom 75 were women. The mean age was nearly 54 (range 15 to 94).
A simple abdominal x-ray was performed in 129 cases, abdominopelvic ultrasound in 43 cases, and abdominopelvic CT in 111 cases. Of that total, 108 patients had either abdominal plain films and ultrasound (37) or abdominal plain films and CT (96), while 21 patients had abdominal plain films as the only imaging test. Both ultrasound and CT were performed in 31 of the cases, whereas 25 patients received all three imaging tests.
As for the endoscopic studies, gastroscopy was performed one to five days after admittance in nine cases of gastric involvement (two with visible parasites, seven with mild inflammatory changes; mean 2.7 days) and five cases with exclusively intestinal involvement through imaging (three with mild gastric inflammatory changes, two normal [ranging from 0 to six days]; mean 2.4 days). In another six cases, a colonoscopy was performed (two with mild inflammatory changes, four normal [ranging from two to five days]; mean 3.7 days).
Surgery was chosen in only one case due to an obstruction of an undetermined cause, observing erythematous petechial spotting in the ileum as the only finding.
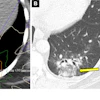
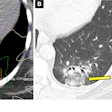
"In the cases of gastric involvement, in CT in decreasing order, wall stratification, wall thickening, perienteric fat stranding and ascitic fluid are predominant," the team wrote. "On the other hand, in the intestinal cases, the wall thickening, fat stranding, engorgement of the adjacent mesenteric vessels and ascitic fluid were more frequent. Furthermore, the ultrasound in intestinal cases showed with greater frequency ascitic fluid and wall thickening."
You can read the full article here.