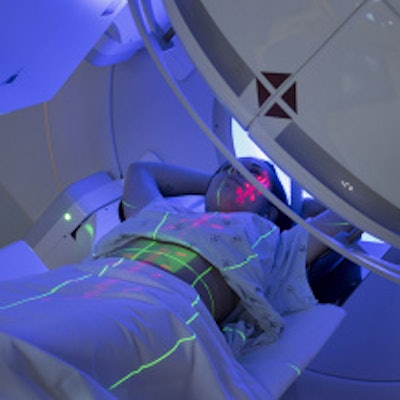
The U.K. government's decision to expand access to diagnostic scans for general practitioners (GPs) in a bid to cut waiting times and speed up a cancer diagnosis has generated intense debate.
As of this month, GPs will be able to directly request CT scans, ultrasounds, or brain MRIs for patients with concerning symptoms but who fall outside the National Institute for Health and Care Excellence (NICE) guideline threshold for an urgent suspected cancer referral.
The Society of Radiographers (SoR) Chief Executive Richard Evans has reacted by calling for a staffing increase, amid fears that the scheme will overwhelm services. "It's important that the growth in workforce is prioritized to support initiatives such as this," he noted in a statement.
Under the NHS' Direct Access scheme, around 67,000 patients who would normally be diagnosed with cancer through non-urgent testing will now be eligible for fast-tracking. This could give them a better chance of having their disease picked up at an earlier stage, when survival chances are higher, according to the SoR.
Evans said that while the principle of primary care clinicians referring patients directly for imaging is a welcome one, the NHS plan makes no reference to the serious workforce shortage currently causing pressure for imaging services.
Dr. Kath Halliday, president of the Royal College of Radiologists, has also issued a response to the initiative.
"Expanding direct access to diagnostic scans across all GP practices is welcome, but GPs aren't radiologists and as scans become ever more complex, it's essential that GPs are able to book the right scan, avoiding costly repeat scanning and devastating delays in treatment," she stated.
"We developed the iRefer Clinical Decision-Making System to enable GPs to book the right scan first time, speeding up diagnosis and saving patient lives, as well as saving money and time. We wholly welcome today's announcement, the positive impact it will have for patients and any pressure reduction for our stretched radiology departments," Halliday added.











![Overview of the study design. (A) The fully automated deep learning framework was developed to estimate body composition (BC) (defined as subcutaneous adipose tissue [SAT] in liters; visceral adipose tissue [VAT] in liters; skeletal muscle [SM] in liters; SM fat fraction [SMFF] as a percentage; and intramuscular adipose tissue [IMAT] in deciliters) from MRI. The fully automated framework comprised one model (model 1) to quantify different BC measures (SAT, VAT, SM, SMFF, and IMAT) as three-dimensional (3D) measures from whole-body MRI scans. The second model (model 2) was trained to identify standardized anatomic landmarks along the craniocaudal body axis (z coordinate field), which allowed for subdividing the whole-body measures into different subregions typically examined on clinical routine MRI scans (chest, abdomen, and pelvis). (B) BC was quantified from whole-body MRI in over 66,000 individuals from two large population-based cohort studies, the UK Biobank (UKB) (36,317 individuals) and the German National Cohort (NAKO) (30,291 individuals). Bar graphs show age distribution by sex and cohort. BMI = body mass index. (C) After the performance assessment of the fully automated framework, the change in BC measures, distributions, and profiles across age decades were investigated. Age-, sex-, and height-adjusted body composition reference curves were calculated and made publicly available in a web-based z-score calculator (https://circ-ml.github.io).](https://img.auntminnieeurope.com/mindful/smg/workspaces/default/uploads/2026/05/body-comp.XgAjTfPj1W.jpg?auto=format%2Ccompress&fit=crop&h=112&q=70&w=112)





