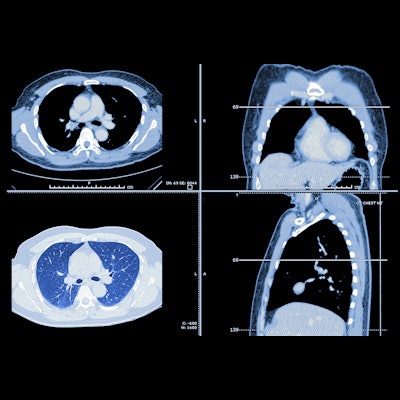
The U.K. Healthcare Safety Investigation Branch (HSIB) has published its latest findings on delays resulting from missed detection of possible lung cancer on chest x-rays of patients seen in primary care.
Lung cancer is increasing in people who have never smoked, and media messaging highlighting the close link between lung cancer and smoking, as well as the often nonspecific symptoms of lung cancer, have created a significant diagnostic challenge for general practitioners, according to HSIB.
Although a chest X-ray is the recommended first test to assess whether a patient may have lung cancer, these images are difficult to interpret, and about one in five cancers are missed, the group stated.
A CT scan should be requested if there is uncertainty regarding pathology instead of a lateral chest x-ray. If in exceptional circumstances a radiologist requests a lateral chest x-ray, the same radiologist should provide the report, the HSIB said.









![Overview of the study design. (A) The fully automated deep learning framework was developed to estimate body composition (BC) (defined as subcutaneous adipose tissue [SAT] in liters; visceral adipose tissue [VAT] in liters; skeletal muscle [SM] in liters; SM fat fraction [SMFF] as a percentage; and intramuscular adipose tissue [IMAT] in deciliters) from MRI. The fully automated framework comprised one model (model 1) to quantify different BC measures (SAT, VAT, SM, SMFF, and IMAT) as three-dimensional (3D) measures from whole-body MRI scans. The second model (model 2) was trained to identify standardized anatomic landmarks along the craniocaudal body axis (z coordinate field), which allowed for subdividing the whole-body measures into different subregions typically examined on clinical routine MRI scans (chest, abdomen, and pelvis). (B) BC was quantified from whole-body MRI in over 66,000 individuals from two large population-based cohort studies, the UK Biobank (UKB) (36,317 individuals) and the German National Cohort (NAKO) (30,291 individuals). Bar graphs show age distribution by sex and cohort. BMI = body mass index. (C) After the performance assessment of the fully automated framework, the change in BC measures, distributions, and profiles across age decades were investigated. Age-, sex-, and height-adjusted body composition reference curves were calculated and made publicly available in a web-based z-score calculator (https://circ-ml.github.io).](https://img.auntminnieeurope.com/mindful/smg/workspaces/default/uploads/2026/05/body-comp.XgAjTfPj1W.jpg?auto=format%2Ccompress&fit=crop&h=112&q=70&w=112)





