It's possible to keep diagnostic mammography exam intervals short, even during a pandemic, according to a study conducted by Canadian researchers and published on 18 June in European Radiology.
The team of researchers, led by Dr. Priscila Crivellaro from St. Michael's Hospital in Toronto, also found that a higher percentage of patients completed their follow-up on their initial visit in 2020, compared with one year prior.
"Our study showed a statistically significant decrease in the diagnostic interval for patients from the pandemic group who did not require tissue sampling for completion of their assessment, as well as for patients requiring tissue sampling with a final benign diagnosis," the study authors wrote.
Before the COVID-19 pandemic hit North America, wait times for follow-up imaging tests and biopsies were determined by booking availability in the breast imaging department, as well as the time it took to access the referring clinician report.
But since screening mammography came to a temporary halt during the first few months of the pandemic -- allowing medical facilities to preserve resources for possible frontline interactions and giving staff the opportunity to self-isolate if needed -- diagnostic screening was also delayed: a situation that can increase patient anxiety, risk of lymph node metastasis, tumor size, and rates of local recurrence and mortality among women with early-stage breast cancer, according to the group.
To avoid this delay, during the pandemic, St. Michael's radiology department was restructured to a rapid diagnostic unit with the goal of completing all diagnostic tests in the least number of visits possible, according to Crivellaro and colleagues.
The team sought to assess whether this restructuring did in fact maintain appropriate time-to-diagnosis timelines, even in the pandemic, through a study that included data from 77 breast imaging patients during April to June, 2020, when the pandemic struck North America, and from 64 patients from April to June, 2019, before the pandemic.
The restructuring was effective: Crivellaro's group found that the time to diagnostic exam actually decreased during the pandemic. It also found that in the pandemic group, 50.6% of patients had their diagnostic assessment completed during the initial screening visit, compared with the 23.4% in the prepandemic group (p = 0.0009).
| Diagnostic interval reductions in breast imaging patients during and before COVID-19 pandemic | |||
| Patient type | Prepandemic group | Pandemic group | p-value |
| Entire cohort | 15 days | 1 day | < 0.0001 |
| Patients not requiring tissue sampling | 11 days | 1 day | < 0.0001 |
| Patients requiring tissue sampling with benign pathology | 33 days | 9 days | 0.0002 |
From these results, study authors said that despite reductions in manpower and clinical services during the pandemic, it is possible to maintain a diagnostic breast imaging service for women at high clinical suspicion for breast cancer.
"Departmental restructuring and patient navigation during pandemic times [can] either maintain or shorten the diagnostic interval for patients presenting for diagnostic mammography," the group concluded.





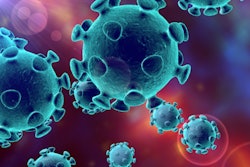




![Overview of the study design. (A) The fully automated deep learning framework was developed to estimate body composition (BC) (defined as subcutaneous adipose tissue [SAT] in liters; visceral adipose tissue [VAT] in liters; skeletal muscle [SM] in liters; SM fat fraction [SMFF] as a percentage; and intramuscular adipose tissue [IMAT] in deciliters) from MRI. The fully automated framework comprised one model (model 1) to quantify different BC measures (SAT, VAT, SM, SMFF, and IMAT) as three-dimensional (3D) measures from whole-body MRI scans. The second model (model 2) was trained to identify standardized anatomic landmarks along the craniocaudal body axis (z coordinate field), which allowed for subdividing the whole-body measures into different subregions typically examined on clinical routine MRI scans (chest, abdomen, and pelvis). (B) BC was quantified from whole-body MRI in over 66,000 individuals from two large population-based cohort studies, the UK Biobank (UKB) (36,317 individuals) and the German National Cohort (NAKO) (30,291 individuals). Bar graphs show age distribution by sex and cohort. BMI = body mass index. (C) After the performance assessment of the fully automated framework, the change in BC measures, distributions, and profiles across age decades were investigated. Age-, sex-, and height-adjusted body composition reference curves were calculated and made publicly available in a web-based z-score calculator (https://circ-ml.github.io).](https://img.auntminnieeurope.com/mindful/smg/workspaces/default/uploads/2026/05/body-comp.XgAjTfPj1W.jpg?auto=format%2Ccompress&fit=crop&h=112&q=70&w=112)






