
The U.K.'s Healthcare Safety Investigation Branch (HSIB) released a report on 17 December regarding the placement and assessment of nasogastric tubes that calls for national training standards in England.
The report was spurred by the case of a young man who had a tube accidentally placed into his lungs while being treated in a critical care ward following a cycling accident. He was then given liquid feed into his lungs for two days before the error was detected.
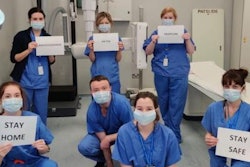
In addition to the most recent case, the HSIB found 14 incidents of misplaced nasogastric tubes from April-September and said COVID-19 has added to the challenges around confirming correct intubation. Correct tube placement can be confirmed by pH testing or x-ray imaging.
The HSIB recommends the British Society of Gastrointestinal and Abdominal Radiology (BSGAR) work with the College of Radiographers (CoR) and Health Education England (HEE) to develop a national training program for x-ray-based confirmation of tube placement. It would also be beneficial for critically ill patients with tubes to have their x-rays confirmed by a radiologist or appropriately trained radiographer, the report added.
Following the report, the Royal College of Radiologists (RCR) and BSGAR will explore training options with CoR and HEE in the new year.
To read the full report, click here.









![Overview of the study design. (A) The fully automated deep learning framework was developed to estimate body composition (BC) (defined as subcutaneous adipose tissue [SAT] in liters; visceral adipose tissue [VAT] in liters; skeletal muscle [SM] in liters; SM fat fraction [SMFF] as a percentage; and intramuscular adipose tissue [IMAT] in deciliters) from MRI. The fully automated framework comprised one model (model 1) to quantify different BC measures (SAT, VAT, SM, SMFF, and IMAT) as three-dimensional (3D) measures from whole-body MRI scans. The second model (model 2) was trained to identify standardized anatomic landmarks along the craniocaudal body axis (z coordinate field), which allowed for subdividing the whole-body measures into different subregions typically examined on clinical routine MRI scans (chest, abdomen, and pelvis). (B) BC was quantified from whole-body MRI in over 66,000 individuals from two large population-based cohort studies, the UK Biobank (UKB) (36,317 individuals) and the German National Cohort (NAKO) (30,291 individuals). Bar graphs show age distribution by sex and cohort. BMI = body mass index. (C) After the performance assessment of the fully automated framework, the change in BC measures, distributions, and profiles across age decades were investigated. Age-, sex-, and height-adjusted body composition reference curves were calculated and made publicly available in a web-based z-score calculator (https://circ-ml.github.io).](https://img.auntminnieeurope.com/mindful/smg/workspaces/default/uploads/2026/05/body-comp.XgAjTfPj1W.jpg?auto=format%2Ccompress&fit=crop&h=112&q=70&w=112)





