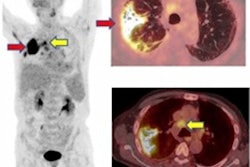
Four patients with suspected COVID-19 underwent FDG-PET/CT at a Chinese hospital. The authors presented their findings online in the European Journal of Nuclear Medicine and Molecular Imaging on 25 March.
Most of the initial use of imaging for COVID-19 has focused on CT, ultrasound, and x-ray. But COVID-19 patients may also have other health issues, for which radiopharmaceutical-based imaging is indicated. In these cases, it's important for nuclear medicine departments to follow strict infection control protocol.
In the new paper, a group from Wuhan shared their experiences with the modalities in a small group of COVID-19 patients.
"In our department, four highly suspected patients with COVID-19 underwent FDG-PET/CT in January 2020," wrote the authors, led by Dr. Xiao Zhang from Union Hospital and Tongji Medical College. "PET and SPECT are routine examinations for clinical diagnosis of various diseases and appropriate protective measures should be carried out during this epidemic."
The Chinese Society of Nuclear Medicine and the editorial board of the Chinese Journal of Nuclear Medicine and Molecular Imaging also issued their set of recommendations on safety measures nuclear medicine departments can take during the COVID-19 pandemic.
Among the guidelines, Union Hospital's nuclear medicine department requires patients initially to undergo a chest CT scan and a reverse transcription polymerase chain reaction (RT-PCR) test for SARS-CoV-2, the virus that causes the novel coronavirus disease, to make sure patients do not have COVID-19 before they proceed to radiopharmaceutical imaging.
"In nonendemic areas, it is also necessary to recognize and classify all patients, verify the history and clinical symptoms of every patient," the authors added.
When the risks outweigh the benefits, patients with a confirmed or suspected case of COVID-19 are asked to postpone their radiopharmaceutical imaging appointment and treatment. However, if the procedure is necessary for their wellbeing, Zhang and colleagues recommended the patients stay in an "isolated room equipped with a high-efficiency particulate air filter." These patients also should be scheduled as the last scan of the day to reduce the chances of other patients or staff contracting COVID-19 in follow-up appointments.
"All patients and accompanying persons must wear a protective mask during the entire examination," the researchers advised. "It [also] is important to try to shorten the examination time and limit the patients' activities."
As for nuclear medicine department staff, many of the safety recommendations already are well-established, such as wearing appropriate medical attire with a cap and mask and practicing good hand hygiene by washing often.
Technologists who inject radiotracers into patients with confirmed or suspected COVID-19 also should wear safety goggles or a face shield, an isolation gown, disposable latex gloves, and shoe covers. If special treatments are needed in case of emergency, "upgraded protections for respiratory and eyes are necessary" for the staff, Zhang and colleagues wrote.
And, of course, gantries, instruments, the scanners, and all other equipment should be cleaned and disinfected as soon and thoroughly as possible.
"We hope our experience could help to safely conduct nuclear medicine work, reduce the risk of disease transmission, and guarantee medical quality and safety," Zhang and colleagues concluded.








![Overview of the study design. (A) The fully automated deep learning framework was developed to estimate body composition (BC) (defined as subcutaneous adipose tissue [SAT] in liters; visceral adipose tissue [VAT] in liters; skeletal muscle [SM] in liters; SM fat fraction [SMFF] as a percentage; and intramuscular adipose tissue [IMAT] in deciliters) from MRI. The fully automated framework comprised one model (model 1) to quantify different BC measures (SAT, VAT, SM, SMFF, and IMAT) as three-dimensional (3D) measures from whole-body MRI scans. The second model (model 2) was trained to identify standardized anatomic landmarks along the craniocaudal body axis (z coordinate field), which allowed for subdividing the whole-body measures into different subregions typically examined on clinical routine MRI scans (chest, abdomen, and pelvis). (B) BC was quantified from whole-body MRI in over 66,000 individuals from two large population-based cohort studies, the UK Biobank (UKB) (36,317 individuals) and the German National Cohort (NAKO) (30,291 individuals). Bar graphs show age distribution by sex and cohort. BMI = body mass index. (C) After the performance assessment of the fully automated framework, the change in BC measures, distributions, and profiles across age decades were investigated. Age-, sex-, and height-adjusted body composition reference curves were calculated and made publicly available in a web-based z-score calculator (https://circ-ml.github.io).](https://img.auntminnieeurope.com/mindful/smg/workspaces/default/uploads/2026/05/body-comp.XgAjTfPj1W.jpg?auto=format%2Ccompress&fit=crop&h=112&q=70&w=112)






