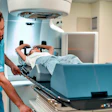
Swiss researchers performing a feasibility study with a new breast CT scanner found that the system turned in high-quality images at low radiation dose. The combination could mean that breast CT could be ready for cancer screening, according to a study published online on 2 March in Investigative Radiology.
In fact, a team from the University of Zurich in Switzerland believes that breast CT has the potential to further improve breast lesion detection and characterization compared with mammography and digital breast tomosynthesis -- particularly because it does not require breast compression, and the photon-counting detector technology reduces radiation dose to levels comparable to those of a conventional mammogram.
"Previous studies investigating the use of conebeam breast CT in comparison to mammography reported higher radiation doses for breast CT, especially when referring to a screening setting," wrote a group led by Dr. Nicole Berger. "More recently, new strategies have strongly increased the dose efficiency due to the use of novel photon-counting detector technology, resulting in dose levels for breast CT comparable to those of screening mammography or lower."
Yet another benefit to breast CT is that it can be used with contrast, Berger and colleagues wrote.
"The possibility to perform contrast-enhanced examinations indicates a possible usage of breast CT comparable to breast MR imaging with the additional capability to simultaneously detect microcalcifications and soft-tissue contrast enhancement," the researchers noted.
Holy grail?
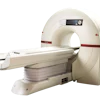
Researchers continue to seek ways to screen for breast cancer that will minimize potential harms and maximize benefits, and Berger's team is no different. This study used data from start-up firm Advanced Breast-CT's dedicated spiral breast CT system, nu:view, which has a photon-counting detector based on cadmium telluride (CdTe) crystals. It's the first clinical in vivo application of nu:view, which received CE Mark certification in September of last year.
Questions have arisen as to whether the resolution of breast CT is high enough to depict microcalcifications. The new detectors address this concern.
"Up to now, resolution of breast CT did not reach high enough resolution to visualize microcalcifications, which the new dedicated breast CT can provide. ... The high resolution, but also the possibility to evaluate the images in different planes, increases and facilitates the characterization of lesions regarding suspicious features such as conspicuity, calcifications, and asymmetries, as well as masses," the researchers wrote.
For the current study, 12 women referred for breast cancer screening underwent bilateral breast CT in the prone position as well as breast ultrasound. Three of the 12 women had previous mammography available for comparison.
Two radiologists interpreted 15 breast CT exams, which they evaluated for image quality using the following measures: spatial resolution, contrast resolution, signal-to-noise ratio, and contrast-to-noise ratio. The researchers used final reports from the breast CT evaluations with ultrasound assessment as the reference standard.
Finally, study participants gave feedback about both positioning and overall comfort during the exam using a scale of 1 to 5 (with 5 equal to maximum comfort).
The major pectoral muscle was included in 15 breast CT scans (62.5%); a glandular component was partially missing in two (8.3%) of the 24 scanned breasts. Berger's group found a "ring" artifact in all scans, although it did not influence image interpretations.
Breast CT identified three masses that were confirmed to be simple cysts on ultrasound. Ultrasound identified another five simple cysts and two solid benign lesions. In all of the breast CT exams, 12 calcifications were identified, with a median size of 1.1 mm; both readers identified all three masses and 11 of 12 calcifications on breast CT.
As for the women's feedback about the comfort of the exam, the majority (75%) ranked it a 4 on a scale of 1 to 5; all women with prior mammography ranked the breast CT exam as more comfortable due to the absence of compression.
With respect to radiation dose, Monte Carlo simulations on phantoms found that mean dose was in the range of 5.08 mGy. For point of comparison, Hendrick et al in 2010 found radiation dose from two-view digital mammography of 3.7 mGy and for film-screen mammography of 4.7 mGy.
"The new dedicated spiral breast CT equipped with a photon-counting detector provides high-quality images at low radiation dose and shows considerable potential for screening and diagnosis of breast cancer, along with improved patient comfort compared with conventional mammography," Berger and colleagues concluded.