Dear AuntMinnieEurope Member,
Anybody who thought the medical imaging community had cracked the problem of CT radiation dose has had a wakeup call early in the new year.
A large international study has highlighted that massive differences in radiation dose levels persist in many countries, and the main factor behind these variations is how healthcare professionals use the equipment and conduct scans. The lead author -- a professor of radiology at the University of California, San Francisco -- has expressed serious concerns and called for urgent action in a news report in the CT Community.
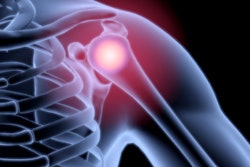
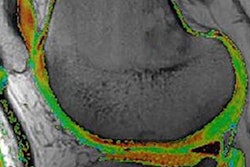
The incidence of osteoarthritis is growing fast in most developed countries, but uncertainty remains over which imaging modalities perform best in specific clinical scenarios. Three recognized musculoskeletal experts have discussed this topic in a comprehensive article posted in our MRI Community.
An increasing number of research groups are reporting success using augmented reality technology to facilitate surgery and interventional procedures, with the potential to boost overall efficiency. A French team has unveiled its findings in this field. Learn more in the Advanced Visualization Community.
In lung cancer cases, imaging techniques that can combine with artificial intelligence to catch pulmonary lesions early while they are still curable will have a widespread impact on patient outcomes and healthcare costs, according to Swiss investigators. They are convinced further development of low-dose FDG-PET can improve the specificity of lung cancer screening and open doors to other applications. Go to our report in the Molecular Imaging Community.
Meanwhile, a German team has integrated a low-field open MR scanner with a static proton research beam line and shown that, in principle, simultaneous proton irradiation and in-beam MRI is technically feasible.
Last week, we released our top 10 stories for 2018, and there were some surprises. We very much look forward to bringing you all the latest news during 2019.








![Overview of the study design. (A) The fully automated deep learning framework was developed to estimate body composition (BC) (defined as subcutaneous adipose tissue [SAT] in liters; visceral adipose tissue [VAT] in liters; skeletal muscle [SM] in liters; SM fat fraction [SMFF] as a percentage; and intramuscular adipose tissue [IMAT] in deciliters) from MRI. The fully automated framework comprised one model (model 1) to quantify different BC measures (SAT, VAT, SM, SMFF, and IMAT) as three-dimensional (3D) measures from whole-body MRI scans. The second model (model 2) was trained to identify standardized anatomic landmarks along the craniocaudal body axis (z coordinate field), which allowed for subdividing the whole-body measures into different subregions typically examined on clinical routine MRI scans (chest, abdomen, and pelvis). (B) BC was quantified from whole-body MRI in over 66,000 individuals from two large population-based cohort studies, the UK Biobank (UKB) (36,317 individuals) and the German National Cohort (NAKO) (30,291 individuals). Bar graphs show age distribution by sex and cohort. BMI = body mass index. (C) After the performance assessment of the fully automated framework, the change in BC measures, distributions, and profiles across age decades were investigated. Age-, sex-, and height-adjusted body composition reference curves were calculated and made publicly available in a web-based z-score calculator (https://circ-ml.github.io).](https://img.auntminnieeurope.com/mindful/smg/workspaces/default/uploads/2026/05/body-comp.XgAjTfPj1W.jpg?auto=format%2Ccompress&fit=crop&h=112&q=70&w=112)






