Researchers using MRI have shown that very low calorie diets (600 to 800 calories per day) can cause a transient deterioration in heart function, according to research presented at the CMR 2018 meeting in Barcelona, Spain.
The study suggests patients with heart disease should seek medical advice before embarking on this kind of diet, according to a team led by Dr. Jennifer Rayner of the University of Oxford in the U.K.
"Crash diets have become increasingly fashionable in the past few years," Rayner said in a statement released by the European Society of Cardiology (ESC), which organizes the meeting under the auspices of the European Association of Cardiovascular Imaging (EACVI). "These diets ... can be effective for losing weight, reducing blood pressure, and reversing diabetes. But the effects on the heart have not been studied until now."
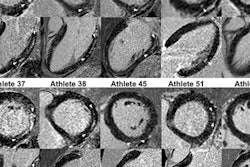
Rayner and colleagues used MRI to investigate the impact of low calorie diets on heart function and the distribution of fat in the abdomen, liver, and heart muscle, including 21 obese volunteers with an average body mass index (BMI) of 37. Participants followed a very low calorie diet for eight weeks. Each underwent an MRI exam at the beginning of the study period and after one week and eight weeks.
The researchers found after one week study participants' total body fat had fallen by an average of 6%, visceral fat by 11%, and liver fat by 42%. Patients also experienced improvements in insulin resistance, fasting total cholesterol, triglycerides, glucose, and blood pressure.
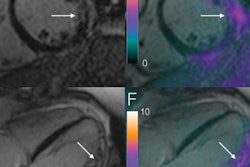
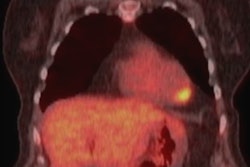
But also after one week, the study participants' heart fat content had risen by 44%, which was associated with deterioration in the heart's ability to pump blood. However, by eight weeks, heart fat content and function had improved beyond what they had been before the diet began, and all other measurements -- including body fat and cholesterol -- continued to improve, the group found.
"The sudden drop in calories causes fat to be released from different parts of the body into the blood and be taken up by the heart muscle," Rayner said. "After the acute period in which the body is adjusting to dramatic calorie restriction, the fat content and function of the heart improved."







![Overview of the study design. (A) The fully automated deep learning framework was developed to estimate body composition (BC) (defined as subcutaneous adipose tissue [SAT] in liters; visceral adipose tissue [VAT] in liters; skeletal muscle [SM] in liters; SM fat fraction [SMFF] as a percentage; and intramuscular adipose tissue [IMAT] in deciliters) from MRI. The fully automated framework comprised one model (model 1) to quantify different BC measures (SAT, VAT, SM, SMFF, and IMAT) as three-dimensional (3D) measures from whole-body MRI scans. The second model (model 2) was trained to identify standardized anatomic landmarks along the craniocaudal body axis (z coordinate field), which allowed for subdividing the whole-body measures into different subregions typically examined on clinical routine MRI scans (chest, abdomen, and pelvis). (B) BC was quantified from whole-body MRI in over 66,000 individuals from two large population-based cohort studies, the UK Biobank (UKB) (36,317 individuals) and the German National Cohort (NAKO) (30,291 individuals). Bar graphs show age distribution by sex and cohort. BMI = body mass index. (C) After the performance assessment of the fully automated framework, the change in BC measures, distributions, and profiles across age decades were investigated. Age-, sex-, and height-adjusted body composition reference curves were calculated and made publicly available in a web-based z-score calculator (https://circ-ml.github.io).](https://img.auntminnieeurope.com/mindful/smg/workspaces/default/uploads/2026/05/body-comp.XgAjTfPj1W.jpg?auto=format%2Ccompress&fit=crop&h=112&q=70&w=112)






